Acute pancreatitis (AP) is defined as acute inflammatory process of pancreatic parenchyma with variable involvement of local tissues and remote organs [8].
It is the most common hepatobiliary cause for hospitalization due to wide range of clinical outcome from transient abdominal tenderness to irreversible systemic complications and sometimes death [9].
Although it is less often in children than adults,
it is the most common disease of pancreas in paediatric age group [10].
Radiologic Grading Systems
Over recent decades,
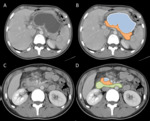
several scoring systems that include radiologic features have been introduced to predict adverse outcomes in acute pancreatitis such as Balthazar classification Fig. 2 [11],
computed tomography severity index (CTSI) Fig. 3 [12] and modified CTSI Fig. 4 [13].
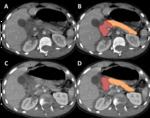
Example cases from our study cohort for scoring systems are shown in Fig. 5 in Fig. 6 .
However,
the diagnosis and management of AP was hindered due to discordance between radiologists and clinicians by confusing terminology [14].
To avoid this discrepancy,
a consortium of AP experts developed the Atlanta Classification in 1992 [14],
which underwent revision in 2012 to adapt the latest understanding of the disease [8].
Definitive Diagnostic Criteria
According to revised Atlanta Criteria,
at least two of the following three criteria for diagnosis of AP is required: abdominal pain compatible with the disease,
at least threefold increase in serum amylase or lipase levels, and imaging findings consistent with AP [15,16].
In 2012,
INSPPIRE (International Study Group of Paediatric Pancreatitis: In Search for a Cure) published a report to standardize definitions and develop diagnostic algorithms for common usage [17].
According to INSPPIRE, AP was defined as similar to revised Atlanta Criteria and Acute recurrent pancreatitis (ARP) was defined as: ≥2 distinct episodes of AP with intervening return to baseline.
Although,
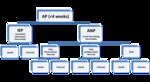
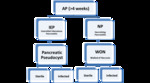
the diagnostic criteria of AP are similar,the terminology of imaging findings and definitions of the complications are more comprehensive in the revised Atlanta Criteria [8] Fig. 7 and Fig. 8 .
There are two types of AP by revised Atlanta criteria called interstitial edematous pancreatitis and necrotizing pancreatitis [9].
To identify the type of disease,
pancreatic and peripancreatic collections were defined according to the presence of necrosis and the time from the onset of symptoms.
In acute edematous pancreas,
collections that are seen less than 4 weeks after presentation are called acute peripancreatic fluid collections,
and if they persist more than 4 weeks they become pseudocyst.
Whereas,
in necrotizing pancreatitis,
collections within 4 weeks of the onset are defined as acute necrotic collections (ANC) and collections that are seen more than 4 weeks after the onset are called walled off necrosis (WON) [15].
The revised Atlanta Classification divides the acute disease course into an early phase which lasts up to 1 week,
followed by a late phase.
Imaging in early phase is not always reliable for local complications such as necrosis [15].
Severe acute pancreatitis is defined in the first phase as organ failure lasting more than 48 hours; and second phase is defined as persistent organ failure,
death or permanent complications related to AP.
For severe pancreatitis,
pancreatic necrosis is a well-known risk factor for morbidity and mortality [13].