From October 2005 to January 2018 we enrolled in our Hospital,
323 patients (aged from 9 to 79 years,
median age 43 years) with clinical suspect of foreign bodies located in the soft tissues.
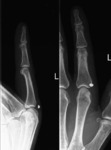
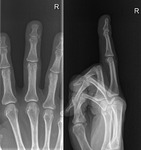
All patients had traditional radiograms and ultrasound investigation.
The diagnosis in 55.7% of cases (195/348) was made in the acute
phase,
immediately after the trauma.
In 153/348 patients (44.3%) the time interval between the traumatic event and the diagnosis was variable between a minimum of 4 days to a maximum of 2 years,
with an average of 6.5 months.
All patients had traditional radiograms and ultrasound investigation using Toshiba aplio 500 ultrasound systems with high-frequency linear-array probes 10-12 Mhz.
The same radiologist expert in musculoskeletal sonography who had performed the diagnostic tests,
with the assistance of a nurse and of a radiographer in training,
subsequently removed the FB under ultrasound guidance in the outpatient’s clinic (Figs.
1-4).
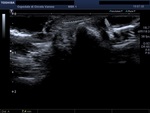
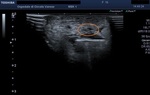
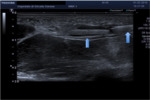
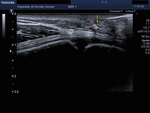
The removal procedure involved the diagnostic ultrasound examination to establish the exact location of the FB,
its morphology and its relations with nearby eloquent structures (vessels,
nerves,
tendons) (Fig.
5).
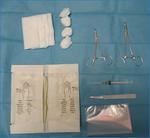
This initial step enables us to plan the treatment and to select the material,
the appropriate ultrasound probe,
and logistics (patient’s position,
operator,
the ultrasound device and the material required).
After disinfecting the patient’s skin,
under sterile conditions (sterile probe cover,
sterile gloves,
mask),
a 22- to 25-G needle is inserted to reach the FB and local anaesthetic with 2-3 ml of lidocaine chlorhydrate 2% administered under ultrasound guidance.
In most cases,
injection of the anaesthetic close to the FB will detach it from the surrounding tissues thereby facilitating subsequent removal (Fig.
6).
The anaesthetic continues to be injected while retracting the needle to anaesthetize the needle path to be used during removal.
Under constant ultrasound guidance,
the skin is then incised,
together with the underlying fascia if necessary,
with a scalpel (Fig 7-8); the incision must be just wide enough for the surgical forceps to be inserted,
or in case of a particularly large FB,
wide enough for the FB to pass through.
The tip of the scalpel must reach the FB to create a complete linear passage between the skin and the FB.
The operator using his/her dominant hand to insert the surgical forceps through the incision reaches the FB,
following its passage in real time on ultrasound longitudinal scans.
The arms of the forceps are then slightly opened,
displacing the tissues surrounding the FB.
In order to grip the object (at this stage,
axial scanning planes are useful to facilitate prehension) and then remove it.
The procedure is terminated with skin disinfection and the skin flaps of the wound closed with Omnistrips.