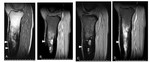
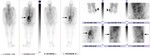
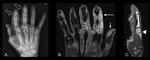
Pathologic correlates with signs of osteomyelitis
Acute OM
-
Soft tissue swelling: result of a leaky vasculature from infectious process,
causing edema and due to penetration of the periosteum from the infection(1).
-
Osteopenia and lucent lesions: spread of infection within the medullary space,
Haversian and Volkmann canals; resulting in abscess and destruction of the trabeculae(1).
-
Cortical fissuring: due to spread of infection through haversian system with osteoclastic bone resorption(5)(Figure 7).
-
Subperiosteal abscess: due to spread of infection into the cambium from the medullary cavity but can also be from direct seeding.
Once the infection is in the cambium it spreads diffusely and is contained at the periphery of the physis by the perichondrium(where the fibrous periosteum and bony cortex meet).
Can cause ischemia from stripping away of periosteum blood vessels.
If granulation tissue is present around the abscess,
consider subacute OM(2)(Figure 2 and 8).
-
Fatty globules and/or fat-pus level within abscess: due to lysis of bone marrow fat from bacterial enzymes or due to ischemia of bone marrow fat resulting in adipocyte lysis and release of intracellular marrow fat(2)(Figure 9).
Subacute OM
Chronic OM
-
Sequestration,
involucrum and cloaca: Sequestrum is a devitalised piece of bone from necrosis because of metaphyseal vessel thromboses and interruption of periosteal vessels(1); involucrum is the surrounding new bone formation of a thick sheath of periosteum when the sequestrated bone involves an entire bone segment(8)(Figure 10).
Cloaca is the result of bacteria penetrating the involucrum resulting in an opening,
which can allow for drainage of infectious and necrotic material(1,8)(Figure 11).
-
Periostitis and involucrum: are a result of subperiosteal abscess raising the periosteum and new bone formation(1).
-
Sinus tracts: are due to soft tissue fistulas because of external migration of dead pieces of the cortex in association with skin and subcutaneous tissue breakdown(1).
Imaging modalities
Radiograph
First study obtained,
are negative in the first 7-10 days; some specificity for late diagnosis,
lacks sensitivity.
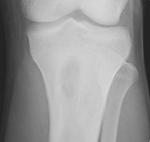
First findings that can be seen are soft tissue changes with blurring of the soft tissue planes and mass formation(1,9).
For findings in the bone to be apparent,
the infection must involve at least 1 cm and compromise 30-50% of bone mineral content(1).
Early bone changes can be identified in children in 5-7 days and in adults in 10-14 days; which are osteopenia,
periosteal thickening,
endosteal scalloping,
loss of trabecular architecture,
lytic lesions and new bone apposition(1).
In the subacute and chronic phases,
radiolucent abscess can be detected; including a Brodie's abscess(Figure 12).
In indolent courses of the disease,
the appearance of necrotic bone in the form of sequestra or sclerosis is not seen for several weeks(1).
Computed tomography(CT)
Excellent to demonstrate subtle osseous changes,
disadvantages are radiation exposure and decreased soft tissue contrast (as compared to MRI).
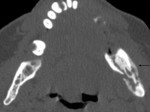
CT can demonstrate chronic OM,
including the rare subtype of sclerosing osteomyelitis of Garre(Figure 13); in which lamellae of newly formed periosteal bone can be seen outside of the cortex,
resulting in the typical 'onion skin' appearance(10,11).
CT is most useful for detecting sequestra,
cloaca,
involucra or intraosseous gas(1).
Detection of sequestra is important as it is a focus of ongoing infection(8).
CT scan also be utilized to help guide biopsies.
Magnetic Resonance Imaging(MRI)
Modality of choice to investigate OM in adults and children(1,2).
Superb spatial resolution and anatomical detail with high sensitivity,
can detect marrow changes 3-5 days after the onset of infection.
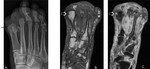
The ability to reflect bone marrow edema allows for early detection of OM; T1 and STIR are the most sensitive and specific sequences,
can detect alteration of normal marrow in 1 to 2 days after onset of infection(Table 1 and Figures 15-18).
Necrotic bone can also be adequately detected in chronic osteomyelitis(Figures 19 and 20)(1).
Limitations are cost,
contrast reaction and presence of surgical hardware.
In young infants and neonates,
T1WI are ineffective because their highly hematopoietic marrow is rich in water and poor in fat; STIR and T2WI are also less reliable in this age group.
In infants with localized epiphyseal infections,
an unenhanced MRI will not be able to demonstrate disease(2).
Nuclear Medicine Imaging
Nuclear medicine is highly sensitivity but lacks specificity in detecting OM; positive studies can be seen 10 to 14 days before apparent on plain radiographs(1).
The three most commonly utilized studies are a 99mTc-MDP triple phase bone scan,
67Gallium scan,
tagged white blood cell (WBC) scan with either 111Indium or 99mTc-HMPAO.
These scans are often used in conjunction with other imaging modalities to supplement findings or to aid in equivocal cases,
as well as when MRI is contraindicated.
We have provided a proposed algorithm for nuclear medicine imaging (Figure 21)(9,12).
Bone scans are done with 99mTc-labeled phosphates and phosphonates and can demonstrate infection in 24 hours.
A triple phase bone scan is the test of choice in uncomplicated OM.
The sensitivity is more than 90%,
but the specificity is less than 50%(13).
Triple phase bone scan is comprised of an immediate perfusion(also called blood flow phase),
in which hyperemia will be seen in the location of OM.
An immediate blood pool phase will demonstrate increased activity due to extravasation through leaky vasculature because of an inflammation/infectious state.
The delayed bone scan images will show increased activity in OM due to bone turnover (Figures 22 and 23)(9).
Differentiating cellulitis from OM can be difficult with the triple phase scan(9).
| Disease process |
Blood flow phase |
Immediate blood pool |
Delayed bone scan |
| Cellulitis |
Increased |
Increased |
Normal |
| OM |
Increased |
Increased |
Increased |
Nuclear medicine imaging is avoided in children due to amount of radiation exposure,
i.e.,
a 99mTc-MDP scan in a one year old would result in 2.8 mSv in effective dose(2).
False negatives on a triple phase bone scan can occur as subperiosteal collections are cold,
likely the result of ischemia(2).
Gallium scan is performed with 67Gallium-citrate,
which is an inflammatory marker and a weak bone agent.
In OM there will be increased accumulation of the radiopharmaceutical (Figure 24).
In equivocal bone scans,
gallium activity exceeding the bone scan activity or distributed more than the bone scan are consistent with OM.
Gallium studies which are normal or less spatially distributed than the bone scan are unlikely to represent OM.
A gallium study that demonstrates similar activity to the bone scan is considered nondiagnostic.
Gallium scan is particularly useful in the spine as bone scans are nonspecific and difficult to obtain in this location because of overlying vasculature and blood pool structures.
WBC scan has a high false negative rate in spinal infections and is often seen as a nonspecific photopenic area.
A gallium scan can also be used to monitor disease activity as appropriate antibiotic treatment will result in decreased activity,
in which bone scans can stay falsely positive in chronic healing/sterile infections due to bone turnover(9).
Tagged WBCs with either 111Indium or 99mTc-HMPAO,
have a high sensitivity for musculoskeletal infections,
approximately 85-100%.
There has been no reported differences in regards to accuracy between these two agents in their ability to detect infection on 24 hour imaging.
The greatest differences are in the biological half life,
availability,
cost,
and resolution.
WBC scans will show accumulation of radiopharmaceutical in areas of inflammation and infection (Figure 25 and 26),
as chemotaxis results in WBC migration.
WBC scan is the test of choice for prosthesis infections,
as bone scans can remain positive for one year following the placement of cemented prosthesis and up to 2-3 years after the placement of non-cemented prosthesis.
WBC scans can be done with bone scans of the hands/feet for better anatomical detail and to separate soft tissue from bone activity,
as WBC scans demonstrate less soft tissue activity.
Of note,
normal bone marrow will take up tagged WBCs and bone marrow imaging with 99mTc-sulfur colloid can be obtain to clarify results(9,12).
| Disease process |
Tagged WBC activity |
Sulfur colloid activity |
| OM |
Increased |
None |
|
Non-infectious process
(i.e.,
expanded marrow)
|
Increased |
Increased |
Bone scans are very nonspecific,
WBC and gallium scans can be positive in inflammatory,
noninfectious states.
In addition,
the extended time required for these studies and lack of anatomical detail has lead to investigation of alternative radiopharmaceuticals.
Alternatives include in vivo leukocyte labeling agents radiolabeled anti-granulocyte antibodies and antibody fragments,
as well as infection-specific radiolabeled fragments of ubiquicidin.
111Indium-biotin scintigraphy is useful in spinal infections,
as it is not taken up by normal bone marrow and can be more specific for bacterial infections(13,14).
SPECT/CT and PET/CT improve accuracy and can better localize radiopharmaceutical uptake to differentiate soft tissue and bone infections.
Although 111Indium-biotin is not yet commercially available,
a study has shown a sensitivity and specificity of 92% in diagnosing OM of the spine when utilized with SPECT/CT(13).
PET utilized agents are radioactive fluorine attached to fluorodeoxyglucose (18F-FDG); gallium-68,
which has a shorter half life and better image quality than 67Gallium; as well as 124I-FIAU,
which is a bacteria specific thymidine kinase substrate.
Even though 18F-FDG-PET is not currently widely used in practice due to non-reimbursement by insurance,
it is the preferred nuclear medicine technique for vertebral osteomyelitis; studies have shown sensitivity of 89-100% and specificity of 88%(13).
18F-FDG-PET can be used with a history of trauma or surgery,
as scans normalize within 3-4 months; scans normalizes after 1 year following prosthesis placement.
FDG-pet can be useful in diabetic foot osteomyelitis,
with many studies showing sensitivity and specificity as high as 74% and 91%,
respectively(13).
Studies also suggest possible differentiation of diabetic neuropathic foot from infection,
represented by lower SUV measurements(15).