The age of the children varied between 2 months and 16 years.
Only two children were vaccinated.
Encephalitis was primary in 5 cases (9.8%),
post-infectious in 29 cases (56.8%),
indeterminate in 17 cases (33.3%).
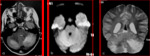
Initial computed tomography scanning (CT) was negative in three of seven cases and demonstrated hypodensities above the tentorium in four of seven cases (the subacute stage).
The CT is essentially used in the evaluation of calcifications.
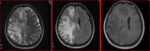
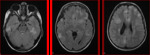
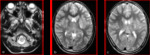
The MRI was performed in all cases and showed an abnormal signal especially above the tentorium.
The T1-weighted image (T1W),
T2-weighted image (T2W) and fluid-attenuated inversion
recovery pulse image (FLAIR) were used in routine practice to identify abnormal areas involved in viral encephalitis (abnormal hyperintense on T2W and FLAIR,
abnormal hypointense on T1W).
FLAIR imaging is more sensitive than T2W spin-echo sequences in detecting encephalitic lesions in the acute phase of the illness.
In typical cases,
MRI examination by T2W and
FLAIR imaging can detect the lesions of viral infection within the first 48 h.
Findings in contrast-enhanced T1W imaging (T1W C+) are variable (The enhancement is especially found in meningoencephalitis).
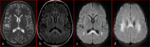
Diffusion weighted imaging (DWI) is used in the early detection of the cytotoxic edema : restricted diffusion and low apparent diffusion coefficient (ADC).
The T2* gradient-echo (GRE) imaging is very useful in detecting hemorrhagic lesions.
T1W hyperintensities are commonly seen also in hemorrhagic lesions.
MR Spectroscopy,
Magnetization transfer ratio (MTR),
Diffusion tensor imaging,
could proof useful in some cases more frequently when differentiating from non-infectious lesions.