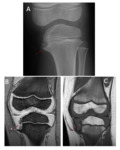
NORMAL SKELETAL MATURATION
The epiphyses,
at the distal ends of the tubular bones,
are located between the primary physis (growth plate) and the joint.
Initially,
the epiphysis is formed entirely by cartilage,
inside which,
the secondary ossification center will appear Fig. 1 [1]
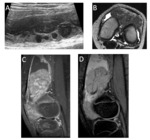
At birth hematopoietic bone marrow (BM) is present throughout the entire skeleton.
The hematopoietic BM shows low signal intensity in the T1-weighted sequences and high signal intensity in the T2-weighted sequences (less than the fluid and similar to the muscle).
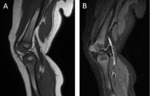
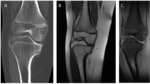
During the first year of life,
hematopoietic marrow begins the conversion to fatty marrow,
starting in the epiphysis and progressing towards the metaphysis [1] Fig. 2 .
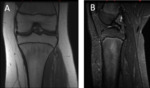
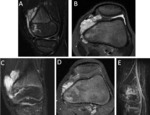
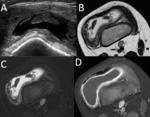
In the knee of young adults,
hematopoietic BM might remain adjacent to the physis Fig. 3 .
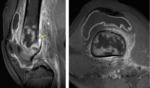
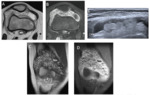
The fat conversion of hematopoietic BM in patients with anemia or who receive growth factors occurs in the opposite direction (metaphysis-diaphysis-epiphysis) [1,3] Fig. 4 .
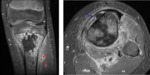
BM malignant infiltration will cause a signal intensity decrease in T1-weighted images,
lower than the muscle signal intensity[1,3] Fig. 5 .
NORMAL VARIANTS ON THE PEDIATRIC KNEE
1.
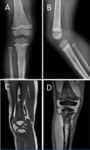
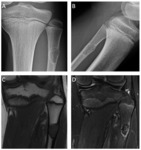
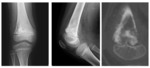
OSSIFICATION VARIANTS OF THE DISTAL FEMORAL EPIPHYSIS
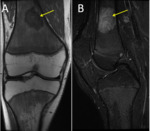
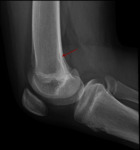
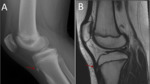
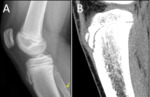
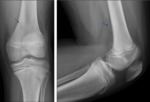
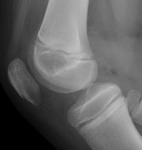
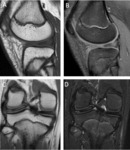
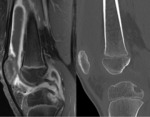
Femoral condyle ossification may be irregular,
showing in the radiography the presence of a radiolucent image located in the distal femoral epiphysis.
It may be bilateral,
and it usually involves the posterior part of the lateral condyle,
although it may sometimes affect the medial condyle or both Fig. 6 Fig. 7 .
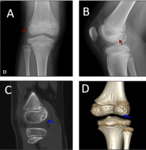
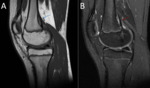
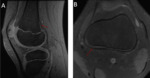
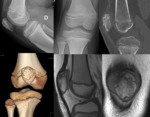
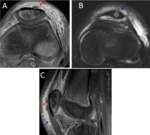
Main differential diagnosis includes the osteochondral lesion,
which usually appears in the medial region of the internal condyle and it is associated with bone marrow edema [2,3,4] Fig. 8 .
2.
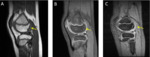
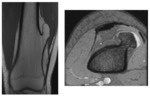
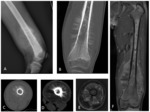
DISTAL FEMORAL CORTICAL IRREGULARITY OR CORTICAL DESMOID
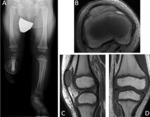
It is a benign fibrous lesion located in the posterior region of the distal metaphysis of the femur,
in the insertion of the internal gastroctemius muscle.
It appears in the radiography as a radiolucent lesion,
with a sclerotic border Fig. 9 .
MRI images show a hypointense lesion in T1-weighted sequences,
with intermediate signal intensity in T2-weighted sequences and a hypointense border in all sequences [2,
3] Fig. 10
3.
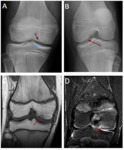
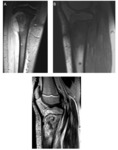
POSTERIOR METAPHYSEAL STRIPE
Subperiosteal stripe in the posterior region of the distal femoral metaphysis,
hyperintense in T2-weighted sequences,
secondary to the presence of subperiosteal fibrovascular tissue in the pediatric age Fig. 11
4.
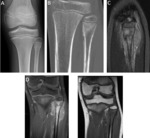
IRREGULARITY OF THE TIBIAL TUBEROSITY
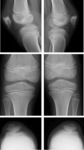
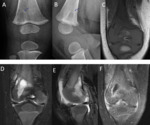
The ossification of the anterior tibial tuberosity may be irregular and fragmented.
In contrast to Osgood-Schlatter disease,
this normal variant is usually painless and pretibial soft tissue increased is not seen.[5] Fig. 12 Fig. 13
5.
PATELLA OSSIFICATION VARIANTS
The patella is usually formed from 2 or 3 ossification centers.
The bipartite patella is the most common ossification variant,
an unfused ossification center at the superolateral aspect [3,5,6,7] Fig. 14 .
Occasionally,
ossification of the normal patella may appear granular or nodular,
with radiolucent and sclerotic areas [3,5,6,7] Fig. 15 Fig. 16 Fig. 17
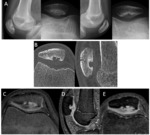
The dorsal defect of the patella is a variant,
of unknown etiology,
in which the appearance of a radiolucent image with a sclerotic border on the superolateral border of the patella is evident,
without bone marrow edema or cartilage involvement,
which should not be confused with an osteochondral fracture [3,5,6,7] Fig. 18 .
DEVELOPMENTAL DISORDERS
1.
CONGENITAL ABSENCE OF CRUCIATE LIGAMENTS
This is a very infrequent finding.
They are usually associated with other malformations,
such as longitudinal limb deficiencies.
MRI usually shows an abnormal morphology of the tibial spines,
dysplastic femoral condyles,
and absence of cruciate ligaments,
with hypertrophy of Humphrey's meniscofemoral ligament. [3,9] Fig. 19 .
2.
DISCOID MENISCUS
Dysplastic and enlarged meniscus,
with loss of the normal semilunar morphology.
It is usually more frequent on the external side.
It may be identified in the MRI sagittal sequences,
in which continuity of the anterior and posterior horn will be seen in three or more cuts.
Signs of mucinous degeneration use to be found and there is a greater probability of tears [3,8] Fig. 20 .
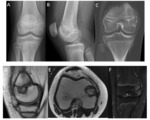
3.
BLOUNT DISEASE
Blount disease refers to a local disturbance of growth of the medial aspect of the proximal tibial metaphysis and/or epiphysis that results in tibia vara.
The medial epiphysis is wedge-shaped and the adjacent metaphysis is fragmented and depressed,
with physis bone bars. The medial meniscus usually presents associated degenerative changes [6] Fig. 21 Fig. 22 .
4.
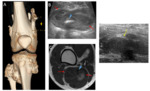
VASCULAR MALFORMATIONS
Vascular malformations can affect the bone,
synovium or extra-articular soft tissues,
although the majority presents intraarticular location.
These malformations are present at birth and grow with the child.
Main symptoms are pain,
swelling,
and spontaneous hemarthroses.
The intra-articular lesions can be low-flow (venous,
lymphatic,
capillary or mixed) or high-flow vascular malformations (malformations and arteriovenous fistulas).
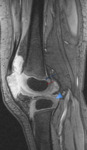
Synovial venous malformations are the most frequent in the knee.
They are usually visualized in MRI as a lobulated multiloculated mass,
with venous lakes separated by septa.
It shows intermediate signal intensity in T1-weighted sequences and hyperintense in T2-weighted sequences,
with signal voids secondary to phleboliths and heterogeneous uptake of contrast due to thrombi [3,
10,11] Fig. 23 .
INFECTIOUS DISEASES
Osteomyelitis is a bone infection that frequently affects the growing skeleton,
with half of the cases occurring in children under the age of 5. It is usually secondary to bacterial hematogenous spread (S.
aureus).
[12].
It usually affects the metaphysis of the tubular bones.
Epiphysis might be affected in children up to 2 years of age. Osteomyelitis is classically divided into acute,
subacute and chronic,
depending on the clinical features,
the duration of the disease and imaging findings.
1.
ACUTE OSTEOMYELITIS:
The x-ray imaging is usually normal during the first days[18].
MRI shows the edema in the BM and adjacent soft tissues.
The lesion shows a heterogeneous contrast-enhancement with areas of ischemia secondary to an increase in intramedullary pressure,
vascular thrombosis,
and interruption of the blood supply of the periosteum.
It is common the appearance of intraosseous and subperiosteal abscesses,
which can cross the cortical bone,
with purulent material that may drain to soft tissue [18] Fig. 24 Fig. 25 Fig. 26 .
2.
SUBACUTE OSTEOMYELITIS:
It is characterized by the appearance of the Brodie's abscess.
In the radiography,
it will be visualized as a well-circumscribed lytic lesion with sclerotic borders.
MRI shows a center of necrosis,
surrounded by a ring of granulation tissue that has an intermediate intensity in T1-weighted MRI image ("the penumbra sign") [12] Fig. 27.
3.
CHRONIC OSTEOMYELITIS:
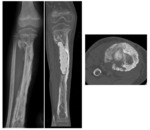
It is characteristic the appearance of fragments of necrotic bone (sequestrum),
surrounded by purulent tissue and reactive bone sclerosis (involucrum).
A defect in the cortical bone can also develop,
allowing drainage of the purulent material into adjacent soft tissue or skin (sinus tract) Fig. 28 .
INFLAMMATORY DISEASE
1.
PIGMENTED VILLONODULAR SYNOVITIS
Benign proliferative disease of unknown etiology.
The knee is the most involved joint.
It is rare in the pediatric age.
MRI demonstrates a lobulated mass (synovial proliferation).
Lesions tend to bleed,
causing hemosiderin deposition and therefore a low-intensity signal in all sequences.
There may be areas of hyperintensity in T2-weighted sequences due to synovial inflammation and joint effusion.
In the knee,
associated bone erosion is infrequent [11,
13] Fig. 29 .
2.
JUVENILE INFLAMMATORY ARTHRITIS
Chronic rheumatological disease,
more frequent in children under 16 years.
The most frequent form of presentation in the oligoarticular,
with greater involvement of the knee.
On MRI the most frequent findings are [11,
13] Fig. 30 Fig. 31 .
- Joint effusion with thickening and synovial enhancement.
-Inflammatory pannus (mass-like synovial proliferation,
with heterogeneous enhancement).
- Hoffa’s fat-pad inflammation.
- Intraarticular low-signal loose bodies (rice bodies).
- Bone erosions (chronic changes).
3.
LIPOMA ARBORESCENS
Infrequent benign synovial lesion of unknown etiology,
characterized by a massive infiltration of the synovium by mature adipocytes without atypia. The most frequent form is the monoarticular involvement of the knee.
MRI is characterized by the presence of joint effusion (with frequent synovial contrast-enhancement) and multiple synovial proliferation of adipose tissue ("rice grains").
Occasionally,
it may show the aspect of a soft tissue mass with fat signal characteristics [11,17] Fig. 32 .
NEOPLASTIC PATHOLOGY
1.
FIBROUS CORTICAL DEFECT (FCD) & NONOSSIFYING FIBROMA (NOF)
It is a frequent benign neoplasm.
It is usually found in metaphyses.
It appears as a lytic lesion with well-defined sclerotic borders.
As the lesion matures,
sclerosis increases.
MRI imaging features depend on the degree of maturation of the lesion [3] Fig. 13 Fig. 14 Fig. 33 .
2.
OSTEOCHONDROMA
This is the second most frequent benign pediatric tumor.
They usually appear in the metaphysis of long bones,
especially the distal femur and proximal tibia.
It is an extension of bone that shows continuity with the periosteum,
cortex,
and bone marrow of the native bone.
It presents a cartilaginous cap that will be visualized as an intermediate signal intensity in T1-weighted sequences and high in T2-weighted sequences.
It is usually asymptomatic,
except in complications: compression of nerves or vessels,
fracture,
inflammation of the exostosis bursa.
Malignant transformation is rare (<1%) [3,16] Fig. 34 Fig. 35 .
3.
CHONDROBLASTOMA
It is a rare benign tumor of immature cartilage,
with a peak incidence between 10 and 20 years.
It has a predilection for the epiphysis of the femur and tibia.
They often pass through the physis to the adjacent metaphysis or even the joint.
X-ray is shown as a radiolucent lesion with sclerotic borders and a chondroid matrix inside.
MRI shows a heterogeneous lobular pattern,
with a low-intermediate signal intensity in T1-weighted sequences and variable in T2-weighted sequences,
with a peripheral hypointense ring.
60% of the cases show variable contrast enhancement.
An accompanying periosteal reaction can be observed,
as well as edema of the bone marrow and the surrounding soft tissues [3] Fig. 36 .
MALIGNANT TUMOURS
1.
OSTEOSARCOMA
Osteosarcoma is the most common primary malignant tumor of the knee.
They usually appear in the metaphysis of long bones (most frequent in the femur) and it may extend to the epiphysis.
The x-ray will show a lesion with aggressive features,
permeative appearance,
with cortical destruction,
soft tissue mass and aggressive periosteal reaction.
In MRI it usually appears hypointense in T1-weighted sequences and hyperintense in T2-weighted sequences with foci of low intensity in all sequences,
secondary to its osteoid matrix [3,5].
At least one entire bone sequence must be performed to exclude other lesions (up to 15%) Fig. 37 Fig. 38 Fig. 39 .
2.
EWING SARCOMA
It is the second primary malignant tumor of childhood.
Imaging typically demonstrates an aggressive lesion,
similar to osteosarcoma.
In contrast,
it usually associates an important non-calcified soft tissue mass.
Fig. 40 .