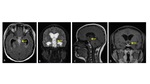
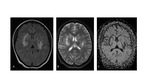
We reviewed our teaching file of patient with central nervous system pathology associated with decreased visual acuity due to lesions of the visual pathway.
The best cases were selected.
A review of the medical literature was perfomed to explain the selected cases.
Visual pathway lesions can be classified into three groups: pre-chiasmatic,
chiasmatic and retro-chiasmatic. [1,3,4]
VISUAL PATHWAY CLASSIFICATION
PRE-CHIASMATIC
Globe
Abnormalities of the globe result in monocular vision loss,
as distinguished from visual field defects.
The most common intraocular tumor of childhood is the retinoblastoma,
a congenital retinal tumor that arises from neuroectodermal cells.
The incidence is 1 in 15000 live births.
The average age of diagnosis is 13 to 18 months.
It manifiests with leukocoria,
glaucoma,
strabismus or vision loss.
Retinoblastoma is unilateral in two thirds of patients.
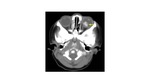
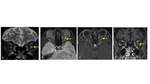
It is important to know that calcification is seen in up to 85% of the cases. Fig. 3 MRI is helpful for evaluating tumor extension beyond the globe.
Variable signal intensity has been reported in retinoblastoma.
It usually shows intermediate to high signal on T1WI and low signal on T2WI.
Gradient echo images may show marked hypointensity in áreas of calcification. [1,2]
In adults, choroidal melanoma is the most common primary tumour of the eye.
Its clinical manifestation depends on the location.
On CT,
it appears as elevated,
hyperdense sharply marginated lenticular lesions which enhances with contrast.
MRI is the modality of choice for evaluation of choroidal melanoma.
On T1WI it is seen as moderately high signal mass lesion,
while on T2WI the signal is low.
With contrast,
it enhances and fat suppression is useful for detect extraocular extensión. Fig. 4 [5]
Optic nerve
Optic nerve pathology also results in monocular vision loss. Optic nerve gliomas are relatively uncommon neoplasm representing 4% of gliomas and 4% of all orbital tumors.
90% appear before age 20.
Symptoms include decreased visual acuity,
proptosis,
nystagmus and strabismus.
Anterior visual pathway gliomas may be limited to one nerve,
both or extend into the optic chiasm an optic tracts.
There is an important association with neurofibromatosis type 1 patients.
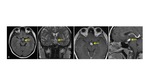
Fig. 5 At imaging,
optic nerve glioma produces fusiform enlargement of the optic nerve.
MRI is the imaging modality of choice for evaluating the extent of gliomas.
They usually are hypointense to isointense relative to brain on T1WI and hyperintense on T2WI.
With contrast,
enhancement is variable.
Prechiasmatic gliomas tend to have less enhacement tan chiasmatic or retrochiasmatic gliomas [1,3,6]
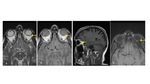
Optic nerve meningiomas are another entity that can affect the optic nerve.
Most frequently they arise from the sheath sourrounding the nerve.
They account for one third of primary tumors of the optic nerve/sheath complex and represent less tan 1% of all meningiomas.
Symptoms at presentation include progressive vision loss and proptosis.
Then patients can develop disc edema and optic nerve atrophy.
There is an association with neurofibromatosis type 2 when optic nerve meningioma is bilateral.
They usually grow along the intraorbital portion of the nerve.
Typically they are hyperdense compared with the nerve on CT,
calcification is frequently seen,
intense enhacement is characteristic and can also show hiperostosis in bone adjacent to the meningioma (near the optic canal).
MRI is superior for evaluating extension.
The intensity is variable.
They enhance intensely afer contrast.
Tubular meningiomas may produce “tram-track sign” with cephalo spinal fluid seen between the nerve and the tumor. Fig. 6 [1,3,8]
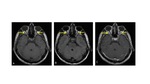
Other cause of prechiasmatic lesion is optic neuritis,
an acute inflammatory process.
The most common cause is multiple sclerosis.
It can be unilateral o bilateral and occurs in young patients (average 30 years).
The optic nerve is a favored site for demyelinating disease and this pathology is the initial manifestation in 15-20% of patients.
During optic neuritis,
about 50% will develop multiple sclerosis.
Symptoms include decrease in visual acuity but they can be asymptomatic.
At imaging,
appears as enlargement of the optic nerve with contrast enhancement. Fig. 7 [1,8]
CHIASMATIC
Bitemporal hemianopsia is the hallmark of optic chiasm pathology,
whether by extrinsec compresion or by an intrinsec chiasmatic lesion.
Glioma is the most common intrinsic lesion of the chiasm,
and may arise in the chiasm primarily or spread to it from the optic nerve.
Gliomas in this location may arise from hypothalamus.
Imaging findings previously described – same features-. Fig. 8 [1,4]
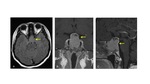
Pituitary macroadenomas by definition have a diameter greater tan 10 mm.
They grow silently (nonsecreting) until they compress the chiasm.
When they reach chiasm usually have a “8” or “snowman” shape with waist being formed by the diaphragm sella.
Their density and intensity used to be similar to the brain without contrast and have moderate enhancement with contrast.
They can present cystic degeneration and/or hemorrhage,
so may have heterogeneous appearance.
Fig. 9 [1,4,8]. Rathke’s cleft cyst or pars intermedia cyst is a differential diagnosis. Fig. 10 [1,4]
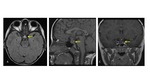
Craniopharyngiomas are another pathology that can compromise the chiasm.
They arise from a remnant of Rathke´s cleft and are located partially or completely within the suprasellar cistern.
They have two incidence peaks,
one in children and the other around the fifth decade.
Frequently they are calcified and have mixed cystic and solid composition (with enhancenment of solid part).
Cystic portion has low attenuation on CT and high signal on T2WI,
but signal on T1WI is variable.
They can also compress the chiasm. Fig. 11 [1,9]
Meningioma is already described (same features).
RETRO-CHIASMATIC
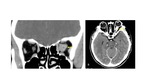
Optic tracs, lateral geniculate nucleus and optic radiations lesions are rarely involved. Occipital cortex lesions manifiest with homonymus hemianopsia or quadrantanopsia with macular sparing.
In this location,
infarcts are the most common abnormality,
even though vascular malformation and trauma may occur.
In addition,
there are cases described in the literature of posterior reversible encephalopathy syndrome (PRES) with transitory visual symptoms.
Below we share a case of these that we had in our institution. Fig. 12 [5,9]