Keywords:
Workforce, Quality assurance, Education and training, Education, Ultrasound, MR, CT, Trauma, Paediatric, Emergency
Authors:
A. Fagan1, S. ffrench-Constant1, A. S. Mehdi1, C. McNamara2, B. P. Jones1, M. Dumba1; 1London/UK, 2Dublin/IE
DOI:
10.26044/ecr2019/C-3364
Results
In total we reviewed 1443 scans,
all of which were performed outside the hours of 9am-5pm Monday to Friday. The results are displayed in fig.
1.
1276 (88.4%) of scans had no discrepancy.
167 (11.6%) of scans contained some level of discrepancy.
- 4 (0.3%) scans contained a grade 1 discrepancy
- 13 (0.9%) scans contained a grade 2 discrepancy
- 150 (10.4%) scans contained a grade 3 discrepancy
Our total rate of major discrepancy was 1.2% (i.e.
below the standard of 2% set by the RCR).
We also looked at the workload on shifts when major discrepancies occured compared to those without any discrepancy:
- Average number of scans reported on a shift during which a major discrepancy occured: 16.7 scans
- Average number of scans reported on a shift during which no discrepancy occured: 14.6 scans
We found that there was a statistically significant (p=0.001) increase in the workload on shifts when major discrepancies occured (see fig.
2).
Of note,
we did not include ultrasound scans or interruptions (e.g.
for discussions about interventional procedures).
Some example grade 1 (major) discrepancies will be reviewed below.
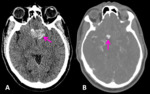
A patient underwent an unenhanced CT head which diagnosed a large suprasellar mass (fig.
3A).
This was identified and reported by the on-call registrar as a possible abscess or malignancy.
The addendum recommended that a CT angiogram should be performed to exclude an underlying aneurysm.
A 10mm aneurysm was then identified on CTA (fig.
3B) and coiled shortly afterwards.
This was labelled a 'grade 1' discrepancy as it affected the immediate management of the patient (i.e.
they would have been transferred to ITU and started on treatment e.g.
nimodipine).
A patient with abdominal pain after a laparoscopic appendicectomy underwent a CT of the abdomen and pelvis with contrast.
The registrar reported that the appendix could not be visualised,
but the consultant addendum stated there was in fact an appendicolith (fig.
4A) within the retained appendix,
and more intra-abdominal gas than would be expected after laparoscopic surgery (fig.
4B),
likely representing perforation.
The clinical impact of this discrepancy was unclear,
as the patient had returned to theatre for an exploratory laparoscopy before the consultant addendum.