Choledochal cysts are relatively rare congenital disorders of the biliary tree,
usually presented in infancy or in childhood [1-7].
They may manifest as focal or diffuse dilatations of the biliary tree.
These cysts occur most often in East Asian populations; the incidence in Japan is 1 in 13,000 versus 1 in 100,000 in Western populations.
The female/male ratio is 3:1 to 4:1 [1,
2,
8].
Many theories exist about the etiology of choledochal cysts.
The most often cited theory is one that Babbit et al proposed in 1969 [9].
They reported a series of patients with anomalous junction of the pancreaticobiliary ducts,
sometimes also referred to as anomalous pancreaticobiliary junction (APBJ),
who were found to have associated type I choledochal cysts.
Developmentally,
the CBD and PD normally unit within the sphincter of Oddi to form a common channel.
The normal length of the common channel is 0.2 - 1.0 cm [10].
It is postulated that the anomalous union of the CBD and the pancreatic duct (PD) outside the duodenal wall and proximal to the sphincter of Oddi mechanism is responsible for choledochal cyst formation [10-16].
The etiology is also believed to be biochemical in nature because the anomalous union produces an abnormal channel which allows pancreatic enzymes to enter the biliary tree.
This results in the weakening of the CBD wall and favors the formation of a cyst.
Two unique features of APBJ are generally used to define choledochal cysts.
The first feature is the formation of a long common channel,
which results from the union of the PD and the CBD outside the duodenal wall.
The second feature relates to the angle of the junction between the PD and the CBD [11].
Normally,
an acute angle forms between the PD and the distal CBD as they converge on,
and are enclosed by the sphincter of Oddi.
In Babbit’s model the distal CBD inserts into the PD in a more or less T-shaped arrangement,
which places the pancreaticobiliary junction proximal to the main sphincter mechanisms of the ampulla of Vater and the main PD sphincter [17].
The resultant anatomic variation produces a situation in which pancreatic juice can freely reflux into the bile duct,
because pancreatic secretory pressure exceeds hepatic biliary secretory pressure.
The prevalence of APBJ is reported to be 60 to 90% in patients with biliary cysts [17].
Some other theories for partial duct obstruction include the mechanisms responsible for the sphincter of Oddi dysfunction and inadequate autonomic innervation.
Tyler et al found that some patients with biliary cysts have fewer ganglion cells than would be expected.
These investigators proposed that there might have been viral damage to the ganglion cells.
Embryologic variations have also been proposed.
It has been postulated that the malformation of the large intrahepatic bile ducts in Caroli disease and the large extrahepatic ducts in choledochal cysts has been associated with faulty remodeling of the embryonic ductal plate [17].
None of the theories seems to tie the various types of biliary cysts together.
The most common classification scheme currently used is the 1977 Todani modification of the1959 Alonso-Lej classification [4,
18].
Type I choledochal cysts are the most common (80%) and,
along with type IVa,
are associated with an abnormally long common channel (>20mm) between the distal bile duct and the pancreatic duct.
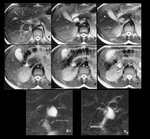
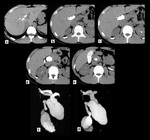
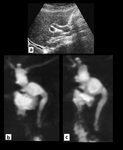
Type I (Fig.1) cysts are extrahepatic cystic dilatations which can extend from the confluence of the biliary radicals to the pancreaticobiliary junction.
Type I can be further subdivided into Ia (cystic dilatation of the CBD),
Ib (segmental dilatation of the CBD)(Fig.2) and Ic (fusiform dilatation of both the common hepatic and the CBD).
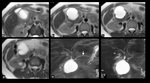
Type II (Fig.
3) choledochal cysts are true diverticula of the extrahepatic ducts and are very rare (2%).
Some cases closely resemble gallbladder duplication.
Type III (Fig.4) cysts,
the “choledochoceles”,
are confined to the intraduodenal portion of the CBD.
They are also rare (1.4-5%).
They may have separate or combined entrances of the distal bile duct and ventral portion of the pancreatic duct.
It is in dispute whether choledochocele represents true dilatation of the biliary tree or it is an anatomic variation [19].
Type IV cysts have multiple features,
which can include an extrahepatic and intrahepatic component.
They are the second most common type of bile duct cysts (19%).
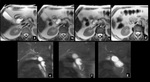
Type IV cysts can be further subdivided into type IVa involving both the extrahepatic and intrahepatic bile duct (Fig.5),
as well as type IVb,
involving multiple segmental dilatations of the extrahepatic bile duct (Fig.
6).
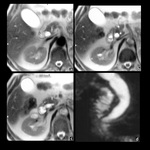
Type V cysts can include one or more intrahepatic biliary cysts but are not associated with extrahepatic biliary cysts.
They may be distributed in a portion of the liver or be distributed throughout the liver.
Type V biliary cyst is also known as Caroli disease.
Todani et al added type V in Alonso Lej’s classification scheme,
but it has a different embryonic origin and seems to be a distinct entity [10].
Visser et al recommended abandoning these numerical designations altogether so that classification of choledochal cysts could be simpler and easier to understand [3].
They recommended referring to the anomalies using the descriptive terms already in common use: choledochal cyst,
choledochal diverticulum,
choledochocele,
and Caroli disease with the term congenital choledochal cyst reserved for the condition made up of Todani types Ia through Ic and IVa.
Choledochal cysts usually present in infants with pain,
jaundice and a palpable abdominal mass [20].
Although abdominal pain is the most common presenting symptom in adult cases the large majority have nonspecific clinical symptoms.
Further,
secondary hepatobiliary disease in adults may obscure the primary condition.
Complications of choledochal cysts in adults include cholelithiasis,
cholecystitis,
recurrent cholangitis,
biliary stricture,
cloledocholithiasis,
recurrent acute pancreatitis,
and malignant transformation into cholangiocarcinoma [1,
21,
22].
The incidence of biliary tract cancer in patients with choledochal cysts increases with age.
Delays in diagnosis and treatment can often extend for years resulting in an increased risk of malignant degeneration. Most of the cancers are seen in the setting of the type I or type IV cysts (those with involvement of the extrahepatic duct and more likely to be associated with APBJ) [10,
17].
Cancers are also seen in some patients with Caroli disease (7%) because of biliary stasis,
chronic inflammation,
and prolonged exposure of the bile duct epithelium to high concentrations of unconjugated,
secondary bile acids [17].
The primary treatment in case of choledochal cysts is surgery including cyst enterostomy,
cyst excision,
or hepaticojejunostomy [23-25].
Surgeries conducted during early childhood are more successful because inflammation or malignant changes may accompany the cysts in adulthood.
Any concurrent anomalies of the pancreaticobiliary junction increase the risk of malignancy due to the long-term exposure of the epithelium to the pancreatic enzymes.
Surgery should not be delayed because it may pave the way to malignancies [23-25].
Pathologically,
choledochal cysts have a fibrotic wall varying in thickness from a few millimeters up to 1cm.
The cyst wall consists of dense collagenous connective tissue with occasional elastic fibers and smooth muscle bundles.
A complete epithelial lining is usually absent.
However,
scattered columnal or cuboidal epithelium can be found.
An inflammatory reaction is often present.
An exception is type III (choledochocele) which is lined by either duodenal or bile duct mucosa [1,
25].