I.
Anomalies of Origin
A.
High Origin
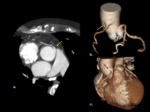
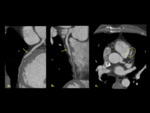
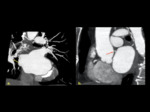
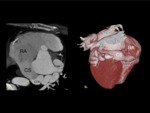
High origin CAA refers to the RCA or LCA arising 10mm above the sinotubular junction of the ascending aorta ( Fig. 1, Fig. 6 ).
It occurs most commonly on the RCA than the LCA,
and is seen in patients with bicuspid aortic valve [6].
The importance of diagnosing a high origin CAA is that it may difficult coronary artery catheterization.
Additionally,
if aortic valve surgery or aortotomy is going to be performed,
the ascending aorta should not be clamped inferior to the high origin coronary artery because it may lead to cessation of cardiac activity [6].
B.
Multiple Ostia
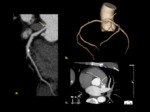
Multiple ostia can occur when the RCA and the conus branch arise from separate locations at the coronary sinus.
It can also be seen in patients were the LAD and LCX arise from separate locations and there is no LCA ( Fig. 2 ).
Multiple ostia represent a challenge for angiography and a conus branch that arises separately from the RCA is at risk for injury on heart surgery if not previously identified.
If the LAD and LCX arise separately it provides a small benefit if proximal atherosclerosis occurs [2].
C.
Single Coronary Artery
The anomalous origin of a single coronary artery from the coronary sinus may have the initial course of either the RCA or LCA,
and then it divides into two branches that follow the RCA and LCA course.
It has been described that if the single coronary artery has a interarterial course (between the aorta and pulmonary artery) it increases the risk for sudden cardiac death.
Another possible complication of a single coronary artery is the inability to form collateral vessels if proximal stenosis occurs [2].
D.
Anomalous Origin of Coronary Artery from Pulmonary Artery
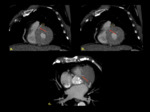
The most common presentation of this disease is the Bland Garland White Syndrome or ALCAPA (Anomalous Left Coronary Artery arising from Pulmonary Artery) in which the LCA arises from the pulmonary artery (PA) and the RCA arises from the right coronary sinus.
This condition occurs in 1/300,000 births and can have two presentations depending on the development of collaterals between the RCA and LCA.
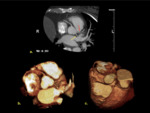
The infantile type shows no collateral vessels ( Fig. 3 ) and presents in the first weeks of life with failure to thrive,
dyspnea,
pallor or chest pain [7].
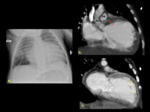
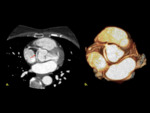
The adult onset type is known to have collateral vessels between the RCA and LCA ( Fig. 4 ) presenting with myocardial infarction,
left ventricular dysfunction or mitral regurgitation [4].
As pulmonary resistance falls,
the blood flows from the aorta to the RCA,
into the LCA in a retrograde fashion via collaterals,
and then to the PA creating a coronary steal phenomenon in which there is a left to right shunt [4]. On CT imaging findings the LCA is seen arising from the main pulmonary artery.
Other imaging findings include dilated and tortuous appearance of the LCA and RCA,
as well as dilated intercoronary collateral arteries.
II. Anomalies of Course
A.
Myocardial Bridging
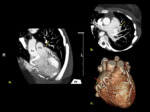
Myocardial bridging occurs when the coronary arteries pass along a tunnel of myocardium instead of running on the epicardial surface ( Fig. 5 ).
Myocardial bridging can be incomplete in which the arterial segment is partially surrounded by myocardium or complete in which the arterial segment is completely surrounded by the myocardium [7].
Myocardial bridging is most commonly seen on the middle segment of the LAD.
This condition is often clinically silent,
but some patients may present with symptoms of angina,
myocardial infarction,
arrhythmias or death.
Symptoms are believed to be the result of the direct compression on the coronary artery during systole or by the formation of atherosclerosis proximal and distal to the tunneled segment which is protected from the development of atherosclerosis [3].
B.
Interarterial Course
Interarterial course refers to a coronary artery passing between the aorta and the main pulmonary artery ( Fig. 6 ).
When a coronary artery arises from the opposite cusp or from the contralateral coronary artery it takes an interarterial course between the aorta and pulmonary arterial trunk.
This is the most common clinically significant coronary artery anomaly; it is the second cause of sudden cardiac death among young athletes [6].
An interarterial course is more commonly seen when the LCA arises from the right coronary cusp and also carries a higher mortality rate when compared to an interarterial course of the RCA [7]. Several theories have been proposed to explain the association between sudden cardiac death and interarterial course.
On physical exertion,
there may be direct compression of the interarterial artery by the aorta and pulmonary artery.
It has also been proposed that interarterial arteries have a “slit-like” orifice that is more prone to occlusion [6].
C.
Transseptal Course
When coronary arteries have an abnormal origin including origin from the contralateral coronary artery or opposite coronary sinus,
they may have a transseptal course along the upper interventricular septum ( Fig. 7 ).
Several characteristics can help to differentiate the transseptal vs interarterial course.
The transseptal course artery is covered in myocardium,
in contrast to the interarterial course artery which courses along the epicardial surface.
The transseptal course artery has a downward configuration referred to as the hammock sign.
The most common arteries having a transseptal course are the LCA and LAD [6].
D.
Retroaortic Course
A coronary artery arising from the RCA or the right coronary cusp and supplying the opposite side of the heart (LCX or LCA) may take a retroaortic course,
between the posterior aspect of the aorta and the interatrial septum ( Fig. 8, Fig. 9 ).
It is important to diagnose this anomaly prior to aortic valve replacement surgery due to possible damage to the artery encircling the aortic valve [6].
E. Prepulmonic Course
Coronary arteries found anterior to the pulmonary artery or right ventricular outflow tract are classified as having a prepulmonic course.
This course is most commonly seen with LCA,
but can also be seen if the RCA has an abnormal origin from the LAD or LCA.
An association with prepulmonic course of coronary arteries and Tetralogy of Fallot has been established,
which makes important recognizing this coronary artery anomaly prior to corrective surgery via median sternotomy [6].
III.
Anomalies of Termination
A.
Coronary Artery Fistula
Coronary artery fistula is the abnormal termination of a coronary artery in a cardiac chamber,
coronary venous system,
pulmonary artery or pulmonary vein ( Fig. 9, Fig. 10 ).
If the coronary artery terminates in a lower pressure chamber it can cause a “steal phenomenon” resembling a left to right shunt [2,
6].
Coronary artery fistulas involve the RCA in 60% of cases and the left coronary system in 40% of cases [2].
On most cases,
the fistula connects with the right sided heart chambers inducing the hemodynamics of a left to right shunt [2].
On CT imaging,
the coronary artery fistula has a dilated and tortuous appearance secondary to the shunt which leads to an increase in blood flow [2,
6].