The mode of onset of chemotherapy-induced lung disease can be acute or insidious.
Timing of clinical manifestations is variable and ranges from hours to years after the initial cycle of treatment.
Lung toxicity can also be completely asymptomatic.
Therefore,
the role of radiologists is crucial in reporting early diagnosis to referring physicians.
Drugs and patterns of drug-induced lung disease are catalogued in the international database “Pneumotox” (www.
pneumotox.com). 
High-resolution computed tomography has the highest sensitivity for detecting infiltrative lung disease.
Interstitial patterns include: nonspecific interstitial pneumonia,
organising pneumonia,
alveolar hemorrhage,
diffuse alveolar damage,
eosinophilic pneumonia,
hypersensitivity pneumonitis,
pulmonary edema,
fibrosis.
Interstitial patterns and mode of onset
| Mode of onset |
Interstitial patterns |
| Acute (minutes to hours) |
Pulmonary edema |
| Subacute (days to weeks) |
Alveolar hemorrhage
Diffuse alveolar damage
Eosinophilic pneumonia
Organising pneumonia
Pleural Effusion
|
| Chronic (months to years) |
Fibrosis |
Imaging histological correlation:
| Ground-glass |
Hypersensitivity pneumonia
Alveolar hemorrhage/ Diffuse alveolar damage
Non Specific Interstitial Pneumonia (NSIP)
Organising pneumonitis
Eosinophilic pneumonia
|
| Bilateral extensive lung consolidation |
Severe alveolar hemorrhage
Diffuse alveolar damage (DAD)
Non specific interstitial pneumonia (NSIP)
Organizing pneumonia
Eosinophilic pneumonia (upper lobes)
|
| Fibrosis |
Non Specific Interstitial Pneumonia (NSIP)
Severe diffuse alveolar damage
Usual interstitial pneumonia (UIP)
|
Interstitial patterns
1) Diffuse Alveolar Damage (DAD)
DAD is a severe acute reaction that can be caused by most therapeutic agents including antibiotics (bleomycin),
alkylating agents (cyclophosphamide,
chlorambucil,
melphalan),
antimetabolites (methotrexate). Exclusion of pulmonary congestion is essential before entertaining this specific diagnosis.
Clinical manifestations include dyspnea,
diffuse pulmonary infiltrates and acute respiratory failure.
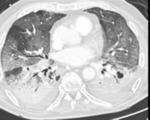
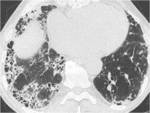
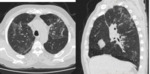
Pulmonary infiltrates are the most common radiologic manifestation,
including ground-glass,
pulmonary consolidation and white lungs Fig. 1 .
Corticosteroid therapy is recommended.
Prognosis is poor.
2) Non Specific Interstitial Pneumonia (NSIP)
The onset of symptoms is insidious.
Clinical features include: dyspnea,
dry cough,
fever.
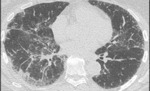
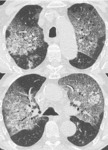
HRCT features include: patchy or diffuse ground-glass opacities,
reticular pattern,
traction bronchiectasis and honeycombing with basal distribution in advanced cases Fig. 2 .
3) Organising pneumonia
Organising pneumonia can be seen with bleomycin,
cyclophosphamide,
methotrexate.
Clinical manifestations include progressive dyspnea,
dry cough,
fever.
HRCT features include patchy migratory areas of consolidaton predominantly with a subpleural,
peribronchial distribution,
centrolobular nodules,
bronchial dilatation.
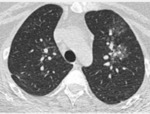
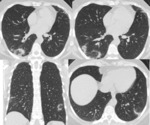
4) Alveolar hemorrhage
Ground-glass opacities are the main imaging feature of alveolar hemorrhage Fig. 3 .
5) Eosinophilic pneumonia
Drug induced eosinophilic pneumonia is a rare condition that has been reported in association with chemotherapeutic agents including Gemcitabine and Methotrexate.
The most common imaging features are bilateral patchy peripheral infiltrates with segmental consolidation,
predominantly in upper lobes.
Ground-glass opacities can be associated.
6) Hypersensitivity pneumonia:
The main imaging features are: bilateral ground-glass opacities,
centrolobular nodular opacities,
lobular and areas of air trapping.
Cases review
Bleomycin
Bleomycin is a cystotoxic antibiotic that is used as an anticancer agent in the therapy of testicular and germ cell cancers,
Hodgkin disease,
lymphomas and tumors of the head and neck. Lung toxicity is dose-dependant and is the most severe adverse effect,
occuring in 4% of patients.
Time from bleomycin initiation to onset of symptoms ranges from 1 to 6 months.
Infiltrative lung toxicities that can be induced by bleomycin are: organising pneumonia,
hypersensitivity pneumonia,
eosinophilic pneumonia and fibrosis.
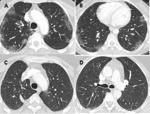
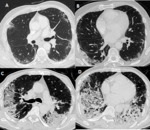
Figure 4 shows CT features of a 45 year old women who underwent Bleomycin therapy for ovarian cancer (Fig. 4 ).
The onset of respratory symptoms after 3 cycles of chemotherapy and the complete resolution of pulmonary infiltrates after withdrawal of bleomycin were strong arguments for drug-induced infiltrative lung disease.
Methotrexate
Methotrexate is a widely used agent in rheumatology.
It is also used for the treatment of lymphomas and sarcomas.
Onset time of methotrexate-induced infiltrative lung disease is variable.
Lung toxicity is not dose-dependant.
Infiltrative lung toxicities that can be seen are: non specific interstitial pneumonia,
usual interstitial pneumonia and hypersensitivity pneumonia.
Figure 5 ( Fig. 5) shows methotrexate induced UIP .
Gemcitabine
Gemcitabine-induced lung toxicity is rare.
However,
concomitant administration of other chemotherapeutic agents and chest radiation are associated with higher risk.
Figure 6 (Fig. 6) is the HRCT of a 45 year old patient with a non small cell lung cancer treated with gemcitabin combined with cisplatin.
He developed bilateral lung infiltrates after 3 cycles with fibrosis signs that appeared after 6 cycles.
Docetaxel
Docetaxel is a therapeutic agent used in lung and breast cancer.
This chemotherapeutic agent can cause fluid retention and pulmonary edema as a consequence of endothelial cells damage.
Other infiltrative lung toxicities that can be seen include hypersensitivity pneumonia and organising pneumonia.
Figure 7 ( Fig. 7 ) shows docetaxel-induced acute infiltrative lung disease in a 47 year old patient treated for breast cancer.
Figure 8 ( Fig. 8 ) shows docetaxel-induced organising pneumonia in a patient treated for breast cancer.
Chlorambucil
Chlorambucil is an alkylating agent commonly used in treatment of chronic lymphocytic leukemia.
Figure 9 (Fig. 9) shows an organising pneumonia in a patient treated for chronic lymphocytic leukemia.