1.
Biliary injury
Biliary injury is one of the most frequent complications of laparoscopic procedures (0.3% of open cholecystectomies vs 0.6% of laparoscopic cholecystectomies),
[6].
The most common causes of biliary injuries are:
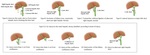
• Their cross section due to anatomical abnormalities - these anatomical abnormalities may relate to variations of the gallbladder itself,
variants of the cystic duct or in the presence aberrant hepatic ducts
• Incorrect identification of the common bile duct or common hepatic duct as the cystic duct - in cases where the cystic duct is not correctly recognized by the surgeon,
there is a risk that another part of the bile tract may be ligated.
Conditions that make it difficult to recognize the anatomy of the area are chronic fibrosis,
the presence of acute inflammation,
bleeding in the area or the presence of fat in the porta hepatis [7].
• Inadvertent placement of clips and ligaments due to the surgeon's inexperience may result in the wrong ligation of the vascular structures of the area.
• Thermal injury due to electrocautery - when attempting to ligate the vessels of Calot’s triangle with electrocautery,
a branch of the bile tree can be injured.
The most widely used classification for biliary injuries is that of Strasberg - Bismuth (Table 1).
Imaging Findings:
The role of imaging is to diagnose,
to highlight the extent of the lesion and to help design the appropriate intervention.
Initial investigation of patients suspected of biliary injuries is done with ultrasound and computed tomography (CT) scanning which can show up liquid collections (biloma,
abscess,
free fluid intraperitoneally) as well as dilatation of intra or extrahepatic bile ducts.
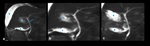
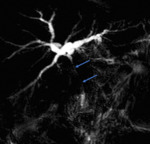
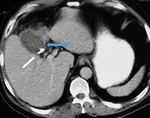
Magnetic resonance cholangiopancreatography (MRCP) is a non-invasive imaging method with high sensitivity (85% - 100%) in the bile tree mapping proximal and distal to the level of injury.
The use of a hepatocyte-selective contrast agent makes it possible to accurately identify and localize the leakage in bile ducts [5,8,9,10,11,12] (Fig.1,
2).
However,
it has certain limitations,
such as poor bile ducts opacification in the presence of stenosis/obstruction and unreliable imaging of the more peripheral intrahepatic bile ducts [13].
Endoscopic retrograde cholangiopancreatography (ERCP) is a very useful method in situations of high suspicion of biliary injuries as it can highlight the exact point of injury or leakage and has the advantage of being able to repair the damage by placing a stent or opening the constrictions by angioplasty.
2.
Biliary stricture
Stenosis is the most common late complication of biliary surgery that develops a few months to years after cholecystectomy in up to 0.6% of cases.
They are usually due to bile duct injury during cystic duct ligation,
chronic irritation from surgical clips or thermal injury during electrocautery.
They are usually found in the common bile duct near the junction point with the cystic or at the junction of the two hepatic ducts [14].
Imaging Findings:
MRCP is a good modality for imaging the bile tract,
while ERCP is the examination of choice because,
in addition to the diagnosis,
it provides the possibility for treatment by placing a stent.
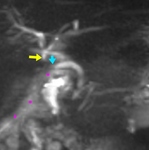
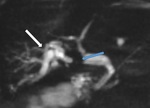
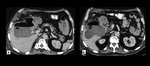
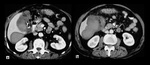
Imaging findings included dilatation of intra and extrahepatic bile ducts with gentle tapering on the point of the stenosis,
focal narrowing and / or nondepiction of a part of the duct [15] (Fig.3,
4).
Distinguishing post-operative benign stenosis from a malignant stenosis of the bile tract is really crucial.
Benign biliary strictures are smooth with tapered regular margins while malignant strictures are longer,
irregular,
with shouldered margins and proximal dilatation and exhibit mild thickening and increased enhancement of the duct wall [16].
MRCP has the advantage of being non-invasive and does not burden the patient with radiation but in some cases may overestimate the extent of the stenosis.
ERCP,
on the other hand,
provides the possibility of taking a tissue sample to clarify the benign or malignant nature of the stenosis [17].
3.
Vascular complications
Vascular injuries are the most life-threatening complications and occur usually during the trocar insertion,
the creation of the pneumoperitoneum or during the dissection of structures in the gallbladder bed and the Calot’s triangle.
These are classified as major and minor according to the damaged vessel as follows:
a.
Major vascular injury: aorta,
vena cava,
iliac vessels,
right hepatic artery,
cystic artery,
portal vein.
b.
Minor vascular injury: epigastric vessels,
mesenteric and omental vessels
Most commonly,
the epigastric vessels,
the cystic artery and the portal vein are damaged.
In some cases,
a bleeding from the gallbladder bed may occur,
without any obvious major vascular injury.
This may be due either to surgical factors (inappropriate tools,
inadequate surgeon's training,
rough technique) or to patient-related factors (liver cirrhosis,
portal hypertension,
gastrointestinal disorders,
adhesions,
acute or chronic gallbladder inflammation).
A relatively small bleeding may be a much greater problem in laparoscopic cholecystectomy than in open surgery due to the difficulty of adequately clearing the blood obscuring the surgical field.
It may also be the cause of other complications such as thermal injury of the bile ducts during the electrocautery of the bleeding vessel.
In cases where bleeding is difficult to control laparoscopically,
conversion to open cholecystectomy is required [7].
Imaging Findings:
If the bleeding is triggered intraoperatively then it can be seen by the surgeon himself.
In cases of post-operative haemorrhage ultrasonography can show heterogeneous fluid collections in the surgical area,
while in CT scan these are depicted as hyperintense collections anywhere intraperitoneally or in the abdominal wall [18].
4.
Post-operative collections – Biloma,
Abscess,
Haematoma
The term “biloma” was first proposed by Gould and Patelto in 1979 to describe a clearly defined collection of bile outside the bile tract [19].
Kuligowska and colleagues widened the term to include also intrahepatic bile collections [20].
The most common causes of post-operative bile formation are biliary injury as well as ineffective ligation of the cystic duct,
both resulting in leakage of bile.
The incidence of biloma after laparoscopic cholecystectomy has decreased significantly and nowadays accounts between 0.3-0.6% [21].
Also,
a small latent haemorrhage may result in the formation of an intra-abdominal haematoma.
Bilomas and haematomas are considered as breeding ground for developing any bacterial infection These bacteria can enter the body from puncture sites,
catheters,
surgical drains or even from the patient's own gastrointestinal system.
Thus,
in patients with sepsis,
all intrahepatic and intraperitoneal liquid collections are suspicious sources of inflammation – abscess.
Consequently,
clinical and laboratory findings should be also taken into account to establish the final diagnosis [22].
Imaging Findings:
Ultrasonography is the imaging modality for the first instance investigation of biloma.
Any well-defined sub-,
intrahepatic or even subphrenic anechoic lesion may suggest the presence of a biloma.
However,
this must be differentiated from other intra-abdominal collections such as abscesses and haematomas.
Abscesses also have a fairly low echogenicity,
but they are usually surrounded by a thick and hyper vascularized wall and may have internal sounds.
On the contrary,
haematomas are initially not encapsulated and their echogenicity gradually increases within the first 24 hours and decreases again as time passes.
Within 1-4 weeks,
internal sounds or septa can be depicted in the collection as they begin to get organized.
CT scan is also a quite useful imaging method for identifying and differentiating intraperitoneal collections.
Biloma is depicted as a liquid collection with water densities near the liver (Fig.
5).
In cases of a subcapsular biloma,
the adjacent liver parenchyma may show increased enhancement during the arterial phase.
The depiction of abscess in CT scan varies.
It is usually depicted as a hypoattenuating,
peripherally enhancing lesion.
In rare cases it may be solid (increased densities) or contain gas,
in the form of bubbles or air-fluid levels (Fig.
6).
The "double target sign" is a characteristic imaging feature of hepatic abscess in contrast-enhanced CT scan.
This is created by a hypo-attenuating center surrounded by a hyper-attenuating inner ring and a second,
low-attenuating outer ring.
The low attenuation of the center is due to the fluid content.
The inner ring represents the abscess membrane which demonstrates early contrast enhancement which persists on delayed images.
In contrast,
the outer hypothenous ring representing the edema of the adjacent liver parenchyma,
only enhances on delayed phase.
In cases where there is significant clinical suspicion of the presence of an intra-abdominal abscess and the information obtained from CT and US imaging is not sufficient,
MRI can solve the problem.
In magnetic resonance imaging the abscess is depicted with a low,
sometimes heterogeneous signal in the T1 sequences and wall enhancement after gadolinium intravenous administration.
In the T2 sequences,
it is characterized by high signal which can be surrounded by a peripheral ring of high signal due to edema in the adjacent liver parenchyma.
More important,
however,
in the final diagnosis of an abscess is the Diffusion-weighted Imaging (DWI).
The abscess cavity has a very high signal in the diffusion sequences,
while also displaying very low values on the ADC maps.
In contrast,
haematoma shows much higher densities in CT,
ranging between 30-45 HU (Hounsfield units) for unclotted blood,
and > 60HU when it coagulates [23] (Fig.7).