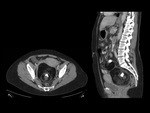
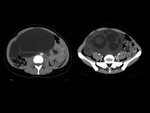
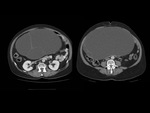
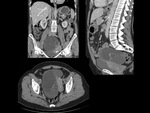
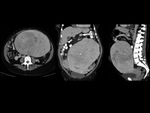
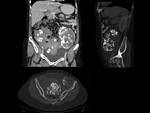
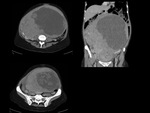
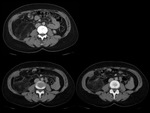
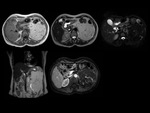
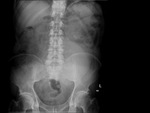
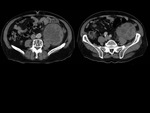
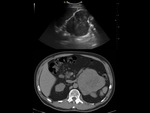
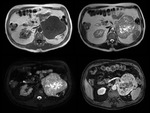
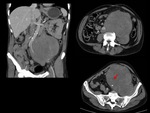
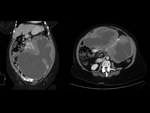
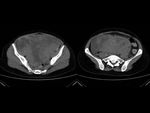
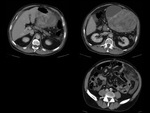
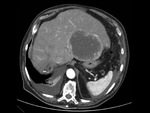
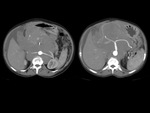
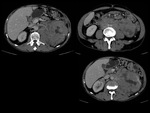
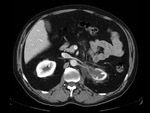
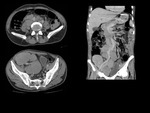
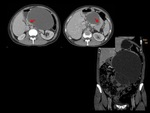
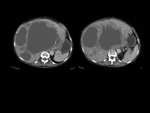
We have made a retrospective review of the giant abdominal tumors studied in our hospital in the last five years and we will show the different radiological findings in these patients.
This includes intra and extraperitoneal abdominal lesions (retroperitoneal tumors being the most frequent) and pelvic lesions (mostly ovarian tumors).
GYNECOLOGICAL PATHOLOGY
1. OVARIAN TUMORS
Ovarian neoplasms are the intraperitoneal organ tumors that most often present as large masses.
Benign ovarian tumors are more frequent than malignant ones,
teratoma being the most frequent ovarian neoplasm.
1.1 TERATOMA
There are 3 types: Mature cystic teratoma,
immature teratoma and monodermal (ovarian struma,
carcinoid tumor and neural tumor).
- Mature Teratoma:
Also called dermoid cysts.
They account for more than 95% of teratomas.
They are composed of well-differentiated tissues derived from the three germinal lines,
so it may contain bones,
teeth,
hair,
cartilage,
skin,
muscle and fat among other components.
The appearance in the different image techniques varies depending on the elements that constitute it.
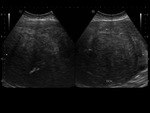
Three possible patterns in ultrasound:
- Cystic lesion with a hyperechogenic mural nodule (Rokitansky nodule)
- Partially or diffusely echogenic mass.
- Multiple thin echogenic bands,
liquid-liquid levels and echogenic images with posterior shadow due to calcifications.
The diagnostic key will be to detect by CT or MRI the presence of fat inside the lesion.
- Immature teratoma
Composed of immature tissues derived from the three germinal lines.
They behave like malignant lesions.
They can be bilateral and coexist with a mature cystic teratoma in the same ovary.
They usually present as large,
complex lesions with an irregular solid component with small foci of adipose tissue.
May have areas of necrosis,
hemorrhage and scattered amorphous calcifications.
1.2 CYSTADENOMA
Cystadenoma represents 40% of the benign ovarian tumors.
- Serous cystadenoma
It presents as cystic lesions of variable size,
usually unilocular although it may have fine septa inside,
acquiring a multilocular aspect.
The presence of papillae is very infrequent and it´s suspicious of a borderline tumor.
- Mucinous cystadenoma
It is usually larger and more often multiloculated,
although thin-walled.
They can present a more heterogeneous content with the presence of echoes inside due to hemorrhagic phenomena.
When they present papillary growths,
malignancy must be suspected.
1.3 CYSTADENOCARCINOMA
Ovarian cancer is the fifth most frequent malignancy in women and the 2nd one of gynecological origin.
Ovarian epithelial tumors constitute 85% of malignant ovarian neoplasms,
with cystadenocarcinoma being the most frequent histological type.
The most frequent histological subtypes are serous and mucinous.
They cannot usually be differentiated by image,
although serous tumors tend to be more homogeneous and mucinous tumors more heterogeneous due to the presence of mucoid material,
detritus or hemorrhage.
The criteria that point to malignancy are:
• Abundant solid papillary projections.
• Thick septums.
• Thickened and nodular walls.
Mucinous-type tumors can rupture and produce a secondary complication known as peritoneal pseudomyxoma,
which consists of the accumulation of mucinous ascites that presents attenuation values greater than the fluid,
with septa/detritus on ultrasound.
Typically it produces an imprint on the liver and spleen,
without infiltrating them,
acquiring its edges a wavy appearance
2. UTERINE MYOMAS
The myoma or leiomyoma is the most frequent gynecological tumor.
They are benign uterine tumors composed primarily of smooth muscle cells separated by varying amounts of fibrous connective tissue.
According to its location,
we distinguish subserosal,
intramural and submucosal myomas.
They usually present as multiple lesions.
Ultrasound: solid hypoechoic masses
MRI: well-defined masses,
hypointense with respect to the myometrium in T2 sequences and with intense contrast uptake.
However,
the image is very variable depending on the histopathological changes that may occur: degeneration (hyaline,
cystic,
myxoid and red),
hemorrhage,
necrosis or calcification.
PRIMARY RETROPERITONEAL NEOPLASMS
Primary retroperitoneal tumors are a heterogeneous and rare group of neoplasms that originate in the retroperitoneum,
outside the organs housed in this compartment.
They usually derive from mesenchymal,
neurogenic or embryonic remnants.
They present an indolent growth and therefore are usually detected when they have reached large size.
Most retroperitoneal masses are of a malignant nature.
The most frequent are sarcomas and within them: malignant fibrous histiocytoma,
liposarcoma and leiomyosarcoma.
1. LIPOSARCOMA
It is the most frequent retroperitoneal sarcoma.
It predominates in women from 50 to 70 years of age.
MRI is the technique of choice for diagnosis.
It usually appears as large masses (> 20 cm).
Histologically,
5 subtypes are differentiated:
- Well-differentiated: masses of fat density that may present thick,
irregular and nodular septa that enhance after the administration of contrast,
which helps to differentiate them from lipomas.
- Myxoid: occur in younger patients.
They appear as heterogeneous hypodense masses,
with thick septum that capture contrast.
- Pleomorphic,
round and undifferentiated cells: They do not have a characteristic behavior so it is difficult to differentiate them from other solid tumors.
They appear as a heterogeneous mass of soft tissue density,
it is not always possible to demonstrate the presence of fat by MRI.
2. LEIOMYOSARCOMA
It is the second most frequent malignant tumor.
It predominates in middle-aged women.
They appear as large soft tissue masses,
characteristically with extensive areas of necrosis and cystic degeneration.
They can affect the vessels by contiguity or originate from them (typically from the inferior vena cava).
3. MALIGNANT FIBROUS HISTIOCYTOMA
It is the third most common retroperitoneal sarcoma and is the most common soft tissue sarcoma of the body.
It occurs more frequently in males in the 6th-7th decade of life.
They usually present as a large solid and infiltrating mass,
with heterogeneous enhancement and areas of necrosis and hemorrhage.
The presence of dystrophic calcifications is frequent.
GIST
Gastrointestinal stromal tumors (GIST) are the most frequent mesenchymal tumors of the gastrointestinal tract.
They generally affect individuals older than 50 years.
The most frequent location is the stomach,
followed by the jejunum and ileum.
They usually present as hyper-vascular exophytic masses of well-defined margins,
with very variable size (from millimeters to 30 cm).
The larger ones may present a heterogeneous appearance due to the presence of hemorrhage,
cystic degeneration or necrosis.
They can present calcifications.
They generally displace adjacent organs and vessels,
but a direct invasion of contiguous structures is very rare.
Intestinal obstruction is uncommon.
Approximately 50% of patients with GIST have a disseminated disease at diagnosis (the most common is hepatic dissemination and to the peritoneum).
Another characteristic finding on this type of tumors is that the involvement of the lymph nodes is extremely rare.
The behavior in the MRI study will depend on the component of hemorrhage and necrosis.
LYMPHOMA
They are solid tumors of the lymphoid tissue.
We distinguish two groups: Hodgkin's disease and non-Hodgkin lymphomas,
the latter being the most frequent hematological disease.
The form of presentation is diverse and non-specific,
so it will practically always enter into the differential diagnosis.
Generally,
we should think of lymphoma in the presence of:
-Adenopathies: in multiple locations,
which can converge forming conglomerates.
-Soft tissue masses of expansive aspect,
not much infiltrative,
with homogeneous enhancement after the administration of contrast.
It involves vascular structures without diminishing their caliber.
INJURIES FROM OTHER LOCATIONS
There are tumors that depend on other abdominal organs that much less frequently can present as large lesions,
such as those of hepatic,
pancreatic or renal origin.