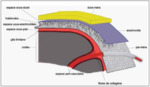
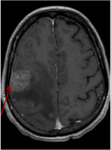
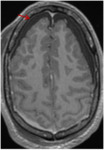
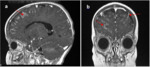
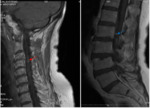
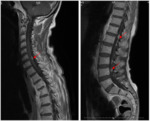
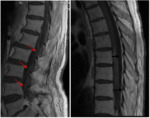
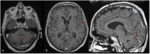
- Normal meningeal appearance on MRI
-The dura mater may be recognized as a short,
discontinuous,
thin,
hyperintense,
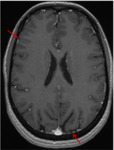
curvilinear structure on contrast-enhanced T1-weighted MRI ( Fig. 2 ).
-The pia mater and the arachnoid mater do not enhance in normal subjects.
-Many factors may affect this appearance such as magnetic power of the machine,
the T1 sequences used (spin echo,
gradient echo,
inversion recovery,
magnetization transfer),
the MRI contrast agent dose and the time between injection and the beginning of the sequence.
- Abnormal meningeal thickening
Meningeal thickening is most notably observed on contrast-enhanced T1-weighted MRI.In order to increase the sensitivity of MR imaging for detection of leptomeningeal disease,
some authors have suggested using a double and even a triple dose of gadolinium contrast material.
Other sequences can be performed after contrast administration besides conventional T1 images:
*Post-contrast fast FLAIR images have been reported to be even more sensitive to leptomeningeal enhancement than post-contrast T1 sequences.
*Fat suppression sequences (T1 or FLAIR) when osseous or soft tissues are involved.
-Distribution patterns for meningeal enhancement:
1. Dura-arachnoid pattern
Curvilinear enhancement is seen overlying the brain and into the immediate inner table of the cranial convexity.
2. Pia-subarachnoid space pattern
The enhancement closely follows the brain surface into sulci,
or outlines the basal cisterns.The enhancement around the brain stem is always classified as the pia-subarachnoid pattern,
since the outer arachnoid layer is separated away from the pia mater by the basal cisterns
3. Dual patterns
The dura-arachnoid and the pia-subarachnoid space patterns can coexist.
- Abnormal meningeal enhancement etiologies
1. Dura arachnoid enhancement
The arachnoid-dural enhancement results from an inflammatory or tumoral thickening and appears as a linear structure within the internal table of the cranial convexity,
but also affects the false brain and tent cerebellum.
Regular and diffuse contrast enhancement is rather related to an inflammatory cause or to an intracranial hypotension (spontaneous or post-lumbar puncture),
whereas irregular or localized contrast enhancement is usually related to a tumoral cause.
a. Diffuse dura arachnoid enhancement
We can distinguish three types of diffuse dura enhancement:
-A diffuse thickening that symmetrically affects the dura mater of the vault,
base,
belly of the brain and cerebellar tent,
first evokes a spontaneous chronic or iatrogenic intracranial hypotension (post-PL,
ventricular derivation)
-A diffuse thickening of the dura mater of the convexity and possibly the base with respect of the dura mater of the false brain and the cerebellum tent evokes a diffuse tumor infiltration,
most often related to a metastatic cause.
-A diffuse dural thickening predominating in the dura mater of the posterior fossa and the cerebellar tent,
with the presence of calcifications (hypointense areas on MRI sequences),
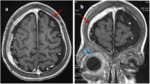
evokes first idiopathic pachymeningitis.Sinusitis and otomastoiditis may be also complicated by pachymeningitis ( Fig. 3 ).
b. Focal dura-arachnoid enhancement
Focaldural enhancement can often be observed in local tumoral or in inflammatory lesions.
Meningioma is by far the most frequent dural based tumor.
It typically presents as an extra-axial well-circumscribed mass with a broad-based duralattachment,
appearing isointense on T1 and T2-weighted images,
and showing intense,
homogeneous post-contrast enhancement.
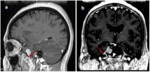
It may demonstrate “dural tail” sign which is present in approximately 60% of meningiomas.
This sign presents as a linear dural enhancement adjacent to the lesion ( Fig. 4 ).
The dural tail sign is however not specific for meningioma and can be observed in association with many vascularized masses,
either dural based or closely related to the dura.
Other lesions such as metastasis( Fig. 5),meningeal sarcoidosis,
meningeal lymphoma,
hemangiopericytoma,
plasmacytoma,
inflammatory pseudotumors in patients with systemic pathology including rheumatoid arthritis,
tuberculoma,
primary meningeal sarcoma,
gliosarcoma,
may have a similar meningeal enhancement appearance on MRI.
Meningeal tuberculosis may be unilateral and involve only one cerebral or cerebellar convexity.
Sarcoid or lymphomatous lesions simulating meningioma may decrease in size with steroids.
Focal dural thickening is routinely observed following craniotomy.Enhancement of dura-arachnoid pattern along the capsule of the hygroma or hematoma can be also seen ( Fig. 6 ).
2. Pia-subarachnoid enhancement:
The differential diagnosis for focal and diffuse pia-subarachnoid enhancement is similar.
Meningococcal meningitis is only associated with abnormal leptomeningeal enhancement when diagnosis is delayed.
However,
marked meningeal enhancement is associated with pneumococcal and tuberculous meningitis especially in the suprasellar cistern and sylvian fissures.
Viral encephalitis and meningo-encephalitis may be associated with focal or diffuse leptomeningeal enhancement.( Fig. 7 )
Leptomeningeal neurosarcoidosis is characterized by a similar pattern of enhancement.
Enhancing nodular intra-axial lesions may involve the brain and cord( Fig. 8 ),
probably from extension of the leptomeningeal process along the perivascular spaces.
Enhancing dural lesions may also be present.
Rapid regression of lesions with steroid treatment is a key instrument for diagnosis.
Leptomeningeal metastases may involve the brain and cord( Fig. 9 ,
Fig. 10 ).
Some key elements are suggestive of metastatic disease:predominent enhancement in dependent regions (pericerebellar cisterns,
lumbar dural sac),
and nodular enhancement of cranial nervesalong the spinal cord and cauda equina.
Leptomeningeal metastases may originate from CSF spread of aggressive or immature primary brain or cord tumors (high grade glioma,
medulloblastoma,
germinoma,
pinealoblastoma,
PNET) or from non-CNS tumors (breast,
lung and prostate tumors,
lymphoproliferative disorders especially lymphoma…).
The presence of symmetrical and bilateral enhancement of all spinal nerve roots and cranial nerves without associated focal tumor suggests a diagnosis of infectious or inflammatory meningoradiculitis (neuroborreliosis,
Guillain-Barré).
Correlation between MRI findings,
clinical setting,
CSF analysis and past medical history is mandatory for appropriate differential diagnosis.
3. Combined dura and pia-subarachnoid enhancement
Both types of meningeal enhancement may coexist,
typically focal in location and in association with a vascularized extra-axial tumor including metastasis( Fig. 11 ),
lymphoma,
focal tuberculous meningitis and sarcoidosis.