Central nervous system tuberculosis has a broad imaging spectrum,
including meningitis,
intracranial tuberculous granuloma (tuberculoma),
abscess,
cerebritis and miliary tuberculosis.
Spinal tuberculosis includes spinal cord meningitis,
epidural or subdural abscess and tuberculoma.
Complications include hydrocephalus,
ventriculitis,
vasculitis and ischemic infarcts.
The major CNS TB imaging findings will be revised in this work.
BRAIN
Meningitis
Meningitis is the most common manifestation of CNS tuberculosis and is most common in children and adolescents.
Clinically,
it has an insidious course with a nonspecific clinical presentation with fatigue,
anorexia,
fever and headache in early stages,
especially in children.
In two to eight weeks,
the patient will develop meningeal irritation.
- CT:
- Can be normal
- Basal cisterns' obliteration by isodense or mildly hyperdense exudates
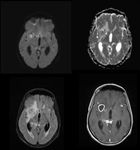
- MR (Fig.
1):
- T1 and T2: initially normal
- FLAIR: hyperintense CSF space,
especially in the sulci
- T1with gadolinium: focal/diffuse basal enhancing exudates
Tuberculoma
Tuberculoma (Fig.
1) is the most common parenchymal lesion in CNS tuberculosis,
which are more common in the supratentorial region and can be solitary or multiple.
- CT:
- isodense/ hyperdense/ mixed density
- ring-like enhancement pattern (if with central calcification it is known as target sign) or nodular
- MR:
- T2/ FLAIR: mixed,
but predominantly hypointensity lesion,
with a central high signal intensity (caseating necrosis) and oedema
- T1 C+: ring-like enhancement
Cerebritis,
abscess and miliary tuberculosis are less common parenchymal lesions.
Complications
Hydrocephalus (Fig.
3)
It is meningitis' most common complication due to impairment of cerebrospinal fluid resorption and flow.
Vasculitis and ischemic infarcts (Fig.4 and Fig.5)
Inflammation of the vessels transversing the subarachnoid space can cause occlusion and ischemic lesions,
most commonly within the internal capsule and basal ganglia,
resulting from vascular compression and occlusion of small perforating lenticulostriate and thalamoperforating arteries.
SPINE
TB is the most common cause of granulomatous spinal meningitis.
Frequently presents shortly after intracranial disease and occurs concomitantly with tuberculous myelitis.
Tuberculomas may form on the inner aspect of the dura and tend to involve the cord.
Therefore intramedullary tuberculoma,
dural disease and leptomeningeal tuberculosis may be difficult to distinguish.
Consequently,
the patient will have CSF loculation and subarachnoid space obliteration,
with loss of the outline of the spinal cord.
Complications include hydrocephalus,
syringomyelia and adhesive arachnoiditis (Fig.
4).