Conditions that compromise the life of cancer patients have to do with the underlying pathology or complications of treatment.
Emergencies can be classified into metabolic,
hematological (of which not try) and structural,
that it may result from bleeding,
compression or obstruction of the tumor itself.
The image studies are crucial in the diagnosis and treatment.
Thoracic emergencies include: the airway obstruction,
esophagorespiratory fistula,
massive hemoptysis,
pulmonary embolism,
superior vena cava syndrome,
pericardial tamponade; and abdominal emergencies include: abdominal hemorrhage,
obstruction,
perforation,
ischemia,
intussusception and urinary obstruction.
Early diagnosis of these diseases helps to select the more appropriate treatment in each case that,
at times,
can be an interventional procedure (abdominal hemorrhage,
hemoptysis).
We have retrospectively reviewed the emerging pathology in oncologic patients who have been performed different imaging techniques in our hospital.
We will show the radiological findings of the most relevant thoracic and abdominal emergencies.
THORACIC EMERGENCIES
Pulmonary thromboembolism (PTE)
Neoplastic processes,
along with the state of hypercoagulation,
recent surgery,
pregnancy,
prolonged bed confinement and the use of oral contraceptives are risk factors for the development of PTE.
PTE is an entity that can be clinically asymptomatic or present non-specific symptoms (dyspnea,
tachypnea or pleuritic pain).
Multidetector computed tomography (MDCT) is the method of choice for the suspicion of a case of acute pulmonary thromboembolism,
as in addition to being a test with high sensitivity and specificity for the diagnosis of PTE,
it provides additional information and/or alternative diagnoses.
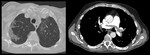
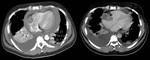
Signs of acute pulmonary thromboembolism in MDCT (Fig.
1):
- Complete repletion defect of a vessel,
with an increase in diameter.
- Partial repletion defect: can be central ("tram-track sign") or peripheral,
forming an acute angle with the wall of the vessel.
- Areas of ground-glass opacity: may be due to hemorrhage or temporary ischemia.
- Atelectasis: by alteration of the surfactant with secondary collapse.
- Infarcts: peripheral triangular condensations of pleural base without enhancement after contrast administration.
The prognosis and the treatment are related to the hemodynamic state of the patient.
The prognostic factors that will determine the severity of the PTE are a major obstruction of the pulmonary arteries greater than 60% and,
above all,
signs of pulmonary hypertension: increased pulmonary trunk caliber,
right ventricular dilatation and displacement of the interventricular septum into the left ventricle.
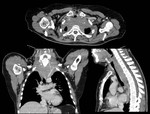
Superior vena cava syndrome (SVCS)
SVCS is due to a difficulty in venous drainage of the head and neck and upper extremities.
It has a very characteristic clinic that includes facial edema and development of swollen collateral veins on the front of the chest wall.
It occurs when the superior vena cava (SVC) is compressed,
invaded,
or thrombosed.
Most commonly,
there is a direct obstruction due to the compressive effect of tumor masses (95%),
whether of pulmonary origin,
thymic or mediastinal lymphadenopathies.
Contrasted CT is the method of choice for the etiologic diagnosis of this syndrome.
CT findings will include (Fig.
2):
- No filling of the SVC.
- Severe stenosis of the SVC.
- Presence of collateral circulation.
- Intraluminal repletion defect,
if there is associated thrombosis.
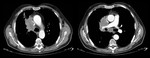
Airway obstruction
Neoplastic processes involving the tracheobronchial tree,
mediastinum,
or pulmonary hilum may compress or invade the airway (Fig.
3 and 4),
producing a respiratory commitment.
Lung carcinoma is the most frequent cause of airway obstruction,
being also produced by lymphoma,
mediastinal adenopathy,
bronchial carcinoid tumor,
endobronchial metastases,
and primary tracheal tumors.
Obstruction of the upper airway may cause acute respiratory failure,
while bronchial obstruction will produce less severe symptoms such as dyspnea,
fever,
and cough.
Esophagorespiratory fistula
Anomalous communication between the esophagus and the trachea,
bronchi,
or pulmonary parenchyma may be secondary to both benign and malignant processes.
The most common causes of neoplasms are esophageal adenocarcinoma,
lung carcinoma,
and lymphoma.
The clinic will consist of recurrent pulmonary infections,
aspiration pneumonitis,
and cough after fluid ingestion.
The findings on chest x-ray are nonspecific,
with recurrent pulmonary consolidations,
pulmonary abscesses,
and pleural effusion.
In case of suspected esophagorespiratory fistula a hypo-osmolar contrast CT should be performed,
which in addition to characterizing the place and extent of the fistula,
will provide information on the adjacent pulmonary parenchyma.
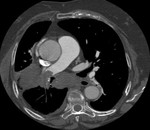
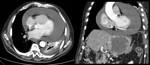
Pericardial tamponade
Pericardial tamponade constitutes a serious complication of the pericardial effusion in which a cardiac compression is produced and prevents the correct filling of the cavities.
The presence of a small amount of pericardial effusion is common in advanced cancers and is usually asymptomatic.
The pericardial effusion can be caused by both metastasis and direct tumor invasion.
The clinic is non-specific and will depend on the amount of fluid accumulated and the speed of onset.
The most frequent symptoms are dyspnea,
chest pain or syncope,
others that might be observed are jugular regurgitation,
paradoxical pulse,
and arterial hypotension.
Echocardiography is the technique of choice.
CT is used in cases where echocardiography is inconclusive,
being of help to determine the cause of effusion.
CT findings are (Fig.
5 and 6):
- Presence of moderate-severe amount of pericardial effusion.
- Deformity and compression of cardiac chambers.
- Angulation of the interventricular septum.
- Dilation of cava veins.
- Contrast reflux to the azygos system and to the lower vena cava.
- Periportal lymphedema.
The treatment of choice is pericardiocentesis,
and surgical drainage may be necessary if it is not resolved.
Massive hemoptysis
The coughing of blood > of 200-400 ml/day or that which,
regardless of the quantity,
implies a vital risk by commitment of the respiratory function or hypotension by the loss of blood,
is considered massive hemoptysis.
Massive hemoptysis has a high mortality rate.
Bronchogenic carcinoma is the most frequent malignant cause of massive hemoptysis,
which may also occur in bronchial carcinoids and in endobronchial metastases of colon,
breast and kidney cancer.
The factors that predispose are large tumors of an angioinvasive character,
with great neovascularization and that destroy the pulmonary parenchyma that supports the vessels.
The treatment of choice is embolization.
In hemodynamically stable patients the previous realization of other imaging tests for proper assessment and planning is useful.
The technique that provides more information is the thoracic CT angiography.
The place,
cause,
and vascular origin of the bleeding (from bronchial,
systemic,
non-bronchial,
or pulmonary arteries) should be identified.
Findings of thoracic CT angiography are:
- Signs of alveolar bleeding: confluent acinar nodules,
ground-glass opacity areas (Fig.
1),
condensations,
atelectasis.
- Presence of clots in the tracheobronchial tree.
- The visualization of an active bleeding is identified exceptionally,
being necessary to search for causes associated with hemorrhage (tumors,
vascular malformations,
aneurysms...).
ABDOMINAL EMERGENCIES
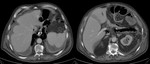
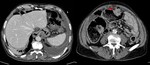
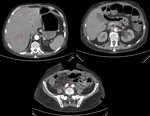
Abdominal hemorrhage
Severe abdominal hemorrhage in oncological patients is a rare,
but life-threatening complication.
Malignant tumors that most often occur with spontaneous abdominal hemorrhage are hepatocellular carcinoma,
renal carcinomas,
and melanomas.
Certain characteristics of the tumors make them more prone to an intratumoral bleeding and posterior rupture,
the main being tumor size,
the peripheral or subcapsular location and the increase of intratumoral vascularization.
In uncontrasted CT,
acute peritoneum manifests as high-density ascites (around 30-45 HU).
The coagulated blood shows a greater attenuation (45-70 HU),
which may indicate the origin of the bleeding.
After contrast administration,
it is possible to see extravasation within the neoplasm and in the peritumoral region,
indicating active bleeding (Fig.
7) and the need for immediate treatment,
either through embolization or surgery.
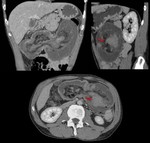
Intestinal obstruction
Adenocarcinoma is the most frequent tumoral cause of intestinal obstruction,
mainly of colon.
Other neoplasms that often produce obstruction include small bowel lymphoma,
gastrointestinal stromal tumor,
carcinoids,
and advanced gynecological neoplasms.
Obstruction in oncological patients can be caused by both wall-affecting tumors that cause decreased motility and linitis plastica,
as well as intraluminal growth of the tumor or extrinsic compression of peritoneal metastases.
In the abdominal x-ray,
we will typically identify dilated bowel loops with hydroaerial levels.
The realization of CT is useful to confirm the location,
severity,
and cause of the obstruction.
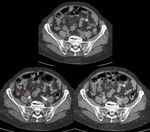
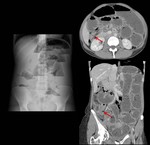
CT characteristic findings are (Fig.
8,
9 and 10):
- Dilation of bowel loops: small bowel loops greater than 2.5 cm or colon greater than 8 cm.
- Visualization of the zone of change of bowel caliber.
- Visualization of "breadcrumb pattern" in small bowel loops,
proximal to the change of caliber area.
- Identification of the cause of obstruction.
- Assess the severity of the obstruction and discard associated complications (incarceration,
ischemia,
and perforation).
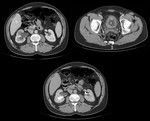
Intestinal perforation
Colorectal carcinomas and gastrointestinal lymphomas are neoplasms that often present spontaneous perforation.
The risk of perforation will be increased if an intestinal obstruction with strangulated bowel loops is also associated,
which will produce wall ischemia with weakening and ruptured walls.
The most important sign of perforation is the presence of extraluminal gas,
which is often identified in simple radiology.
CT can be used to identify the cause,
location,
and extent of the perforation.
The intestinal perforation findings that we can objectively in CT include (Fig.
11,
12 and 13) pneumoperitoneum,
leakage of intestinal content and oral contrast,
discontinuity of the wall,
the presence of gas and/or collections surrounding the tumor,
and less frequently,
contrast leakage to an adjacent bowel loop by formation of fistula.
Intestinal ischemia
Mesenteric ischemia is one of the most lethal abdominal emergencies.
In tumor patients,
intestinal ischemia may be secondary to severe distension due to mechanical obstruction or mechanical vascular occlusion.
Patients with tumors that affect the root of the mesentery may present ischemia secondary to compression and invasion of the mesenteric vessels.
The radiological findings we can find in mesenteric ischemia are (Fig.
14):
- Repletion defects in artery or mesenteric vein.
- Dilation of bowel loops,
often filled with fluid.
- Alterations in the enhancement pattern of the bowel wall: the increased enhancement of some segments is an early sign of ischemia and indicates viability; if on the other hand there is an absence of enhancement it is a sign of infarction and indicates that the bowel loop is not viable.
- Thickening of the bowel wall: it is more frequent in venous thrombosis and is related to reversible ischemia.
- Pneumatosis intestinalis and air in portomesenteric veins are late signs of transmural bowel wall necrosis.
- Other signs of bowel necrosis are pneumoperitoneum,
ascites,
and mesenteric edema.
Intestinal intussusception
Neoplastic etiologies are responsible for approximately 50% of all adult intussusceptions; among them,
intestinal lymphoma,
gastrointestinal tumor,
and metastatic disease to the bowel wall are the common malignant conditions.
Both primary and secondary bowel wall neoplasms involving the small intestines and colon can act as lead points and cause intussusceptions.
CT depiction of a telescoping or “bowel-within-bowel” appearance,
with or without incorporation of adjacent fat and vessels (Fig.
15),
confirms the diagnosis.
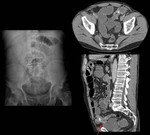
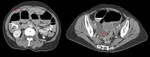
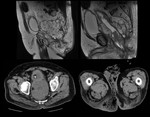
Urinary obstruction
Most urinary obstructions due to oncological causes occur from infiltration or compression of the ureteral pathway (bladder,
prostate,
or cervix neoplasia).
Obstruction of one or both ureters may also be due to extrinsic compression by a tumor or lymph nodes.
Another possible cause is fibrosis that originates after surgery or radiotherapy in the retroperitoneum.
It is mainly patients who come to the emergency room for decreased diuresis,
symptoms resulting from acute renal failure or those who have progressive deterioration of renal function tests.
Diagnosis is confirmed radiologically by ultrasound or CT showing the dilatation of the urinary excretory system (Fig.
16).