Systematic research of the literature was carried out and compare with the database of our institution; the most representative cases were selected and organized in a diagnostic algorithm ( Table 1 ).
This algorithm is based on the classification proposed by Osborn and Preece in the article called: “Intracranial cyst: Radiologic – Pathologic correlation and imaging approach” (1) and in the ECR educational exhibit: “Differential diagnosis of intracranial cystic lesions” with the DOI: 10.1594/ecr2015/C-0215.
We focus in supratentorial and benign lesions although some tumoral lesions will be named in order to have a more general idea.
BRAIN LESIONS - SUPRATENTORIAL
1.
EXTRA - AXIAL
1.1.
BENIGN LESIONS
1.1.1.
Pineal Cyst
Definition: Pineal cyst has three layers: the outer layer (fibrous connective tissue),
a middle layer (pineal parenchyma with or without calcification) and an inner layer (glial tissue) (1).
Location: Pineal gland.
Age of presentation: young aged adults 20-30 years of age.
Female to male ratio 3:1 (2).
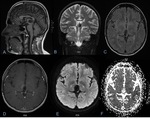
Imaging: Unilocular fluid-filled mass within the pineal gland (1) ( Fig. 1 ).
CT: With or without a rim or nodular calcium in the cyst wall on nonenhanced CT (1).
MR: T1: most of the cyst are slightly hyperintense to cerebrospinal fluid.
Most do not appear hypointense on FLAIR.
60% enhance with contrast material (1).
Differential Diagnosis: Pineocytoma,
arachnoid cyst,
epidermoid cyst.
1.1.2.
Dermoid Cyst
Definition: Congenital ectodermal (strictly) inclusion cyst.
The capsule consists of simple epithelium supported by collagen.
This cyst increases in size due to glandular secretion and epithelial desquamation (1).
Location: Midline sellar,
parasellar or frontonasal region (1).
Age of presentation: Typically,
dermoid cysts present in the first three decades of life (3).
Imaging: Cysts have the same imaging characteristics as fat because they contain liquid cholesterol (1) ( Fig. 2 ).
CT: Well-defined,
lobulated,
“pearly” mass of variable size (1).
MR: Hyperintense on T1-weighted images and do not enhance.
Heterogeneous signal intensity on T2-weighted images (1).
Differential Diagnosis: Lipoma,
craniopharyngioma,
teratoma,
epidermoid cyst (1).
1.1.3.
Rathke Cleft Cyst
Definition: congenital non-neoplastic cysts arising from remnants of the embryonic Rathke cleft (1,
4)
Location: Forty percent are completely intrasellar,
while 60% have some supra-sellar extension (1,
4)
Age of presentation: Although congenital,
they appear to enlarge during life,
as they are rare in childhood (5).
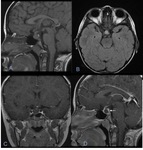
Imaging: Rathke cleft cysts are smoothly marginated cysts that vary in size from a few millimeters to 1–2 cm (1) ( Fig. 3 ).
CT: Nonenhancing noncalcified intra and/or suprasellar cyst with an intracystic nodule (1,
4).
MR: A half are hyperintense on T1 and a half are hypointense.
T2: 70% are hyperintense and 30% are iso or hypointense (4).
Differential Diagnosis: Craniopharyngioma,
cystic pituitary adenoma (1).
1.1.4.
Arachnoid Cyst
Definition: Benign,
congenital,
intraarachnoid space-occupying lesions that are filled with clear cerebrospinal fluid (1).
This cyst does not communicate with the ventricular system (6).
Location: Most arachnoid cysts are supratentorial.
Fifty to 60% are found in the middle cranial fossa,
anterior to the temporal lobes (1).
Age of presentation: Congenital.
Imaging: The cysts tend to be unilocular,
smoothly marginated expansile lesions that are molded by the surrounding structures ( Fig. 4 ).
CT: A sharply demarcated extra-axial cyst that can displace or deform adjacent brain.
No identifiable internal architecture and does not enhance (1).
MR: The cyst typically has the same signal intensity as CSF at all sequences (1).
Differential Diagnosis: Epidermoid cyst.
1.1.5.
Epidermoid Cyst
Definition: Congenital inclusion cysts
Location: The most common location for epidermoid cysts is the cerebellopontine angle cistern (40%–50%) (1).
Age of presentation: Congenital.
Imaging: CSF-like mass that insinuates within cisterns,
encasing adjacent nerves and vessels (1) ( Fig. 5 ).
CT: Well-defined hypoattenuated masses that resemble CSF and do not enhance.
Calcification is present in 10%–25% of cases (1).
MR: Isointense or slightly hyperintense to CSF on both T1- and T2-weighted MR images.
They do not suppress completely on FLAIR images and restrict on diffusion-weighted images (1).
Differential Diagnosis: Arachnoid cyst.
1.2.
INFECTIOUS LESIONS
1.2.1.
Neurocysticercosis
Definition: Parasitic infection.
Location: Most neurocysticercosis cysts are found in the subarachnoid spaces,
typically the basal cisterns and deep within the sulci (1).
However,
although they can present an extra-axial location,
they can also present an intra-axial location,
as we can see in the example ( Fig. 6 ).
Age of presentation: Time interval between the point of infection and the onset of symptoms ranging from 1 to 30 years.
Imaging: Vary with the stage of cyst development (1).
CT and MR: Early vesicular stage (smooth thin walled cyst) with a mural nodule (viable larval scolex).
Then colloidal-vesicular stage with pericystic edema and cyst wall enhancement.
The healing or granular nodular stage (calcified scolex) with surrounding edema and enhancement.
Residual cyst.
Finally,
quiescent or residual stage (small calcified nodules) (1).
Differential Diagnosis: Abscess,
tuberculosis,
neoplasm,
enlarged perivascular spaces (1).
1.3.
TUMORAL LESIONS
1.3.1.
Craniopharyngioma
Definition: Benign neoplasm (WHO I).
Arise in the sellar/suprasellar region.
There are two histological subtypes,
adantinomatous and papillary.
Craniopharyngiomas are believed to derive from Rathke cleft (7).
1.3.2.
Cystic Meningioma
Definition: The most common tumor of the meninges.
They are a non-glial neoplasm that originates from the meningocytes or arachnoid cap cells of the meninges and are located anywhere that meninges are found (8).
2.
INTRA - AXIAL
2.1. ANATOMICAL VARIANTS
2.1.1.
Cavum septi pellucidi
Definition: The septum pellucidum consists of two thin laminae of white matter surrounded by gray matter with a potential intervening space.
The leaves are separated in utero but fuse from back to front as the fetus approaches term or in the first few weeks after birth (9).
The cavum septi pellucidi persists when the two leaves fail to fuse (9).
The cavum septi pellucidi has the following boundaries: anteriorly,
the genu of the corpus callosum; superiorly,
the body of the corpus callosum; posteriorly,
the anterior limb and pillars of the fornix; inferiorly,the rostrum of the corpus callosum and the anterior commissure; laterally,
the layers of the septum pellucidum (10) ( Fig. 7 ).
Location: Corpus callosum.
Age of presentation: Congenital.
Imaging: On the sagittal images,
the cavum septi pellucidi is roughly triangular with the base at the corpus callosum.
Viewed in the coronal plane,
the cavity is also triangular with its base at the corpus callosum (10).
2.1.2.
Cavum vergae
Definition: The cavum vergae is a fluid-filled space between the two leaves of septum pellucidum located posterior to an arbitrary vertical plane formed by the columns of the fornix (9).
The cavum vergae has the following boundaries: anteriorly,
the anterior limb of the fornix,
superiorly,
the body of the corpus callosum,
posteriorly,
the splenium of the corpus callosum,
inferiorly the hippocampal commissure,
the fibers of which bridge space between the diverging posterior pillars of the fornix (10) ( Fig. 7 ).
Location: Corpus callosum.
Age of presentation: Congenital.
Imaging: This cavity is also triangular when viewed from lateral.
The cavum vergae flares out laterally on both sides with the curve of the fornix and pushes under the lateral ventricles at its extreme lateral extensions (10).
2.1.3.
Cavum veli interpositi
Definition: It is a potential space above the tela choroidea of the third ventricle and below the columns of the fornices (9).
The cavum veli interpositi is located in front of the quadrigeminal (superior) cistern above the roof of the third ventricle (10).
The cavum veli interpositi is separated from the cavum vergae by the crura of the fornices (9) ( Fig. 8 ).
Location: In front of the quadrigeminal cistern.
Age of presentation: Congenital.
2.2.
BENIGN LESIONS
2.2.1.
Enlarged Perivascular Spaces
Definition: Virchow- Robin spaces are pial-lined interstitial fluid-filled structures that accompany penetrating arteries and veins.
They do not communicate directly with the subarachnoid space.
Enlarged perivascular spaces are “leave me alone” lesions.
Microscopically it consists of a single or double layer of invaginated pia (1).
Location: They frequently appear in the inferior basal ganglia (1).
Age of presentation: Congenital.
Normal variant.
Imaging: Most appear as smoothly demarcated fluid-filled cysts,
typically less than 5 mm in diameter,
and often occur in clusters in the basal ganglia or midbrain (1) ( Fig. 9 ).
MR: They are isointense to CSF at all sequences,
including FLAIR.
They do not enhance,
cause focal mass effect,
or restrict on diffusion-weighted images (1).
Differential Diagnosis: Multiple lacunar infarcts,
cystic neoplasms,
and infectious cysts (1).
2.2.3.
Porencephalic Cyst
Definition: Porencephalic cysts are congenital or acquired cavities within the cerebral hemisphere that usually communicate directly with the ventricular system (1).
Location: They can be cortical or subcortical,
unilateral or bilateral.
The location often corresponds to territories supplied by the cerebral arteries (1).
Age of presentation: Congenital or acquired.
Imaging: Cystic space in the brain parenchyma that communicates with an enlarged adjacent ventricle (1) ( Fig. 10 ).
MR: The cysts have the same appearance as CSF at all MR sequences.
Adjacent white matter typically shows hyperintensity on T2-weighted and FLAIR images (1).
Differential Diagnosis: Arachnoid cyst,
schizencephaly,
ependymal cyst,
encephalomalacia,
and hydranencephaly (1).
2.2.4.
Cyst of the Corpus Callosum (splenium)
Definition: Different lesions can be present in the form of cyst in the corpus callosum.
Location: Corpus callosum.
Age of presentation: Different ages.
Imaging: Cystic appearance ( Fig. 11 ).
Differential Diagnosis: Enlarged perivascular space,
neurocysticercosis,
gliosis and others.
2.2.5.
Choroid Plexus Cyst
Definition: Choroid plexus cysts are non-neoplastic epithelial lined cysts of the choroid plexus (1) ( Fig. 12 ).
Location: Lateral ventricular atria.
Age of presentation: Found incidentally,
typically in neonates and older adults (1).
CT: These lesions are iso- to slightly hyperattenuated on nonenhanced CT scans compared with cerebrospinal fluid.
Peripheral calcification is common.
The cysts show enhancement that varies from none to striking (1).
MR: Signal intensity on MR images is variable.
Most are iso- or hyperintense on precontrast T1-weighted MR images compared with CSF and show rim or nodular contrast enhancement.
These lesions are usually hyperintense to CSF on T2- weighted images,
especially with long repetition/short echo time sequences.
The majority do not become completely hypointense (suppress) on fluid-attenuated inversion recovery (FLAIR) images and remain slightly or moderately hyperintense to cerebrospinal fluid (1).
Differential Diagnosis: Ependymal cyst,
villous hyperplasia of the choroid plexus (1).
2.2.6.
Ependymal Cyst
Definition: Ependymal cysts are rare,
benign,
ependymal-lined cysts of the lateral ventricle or juxtaventricular region.
Ependymal cysts are thought to arise from sequestration of developing neuroectoderm during embryogenesis (1).
Location: Temporoparietal region and frontal lobe (1).
Age of presentation: Most are incidental,
but symptomatic cysts may manifest with a headache,
seizure,
and/or obstructive hydrocephalus (1).
Imaging: The best diagnostic clue is a nonenhancing thin-walled cerebrospinal fluid-containing cyst of the lateral ventricle (1).
Differential Diagnosis: Choroid plexus cyst,
arachnoid cyst,
neurocysticercosis,
asymmetric ventricules (1).
2.2.7.
Colloid Cyst
Definition: Colloid cysts are a benign mucin-containing cyst.
Colloid cysts are derived from embryonic endoderm (not neuroectoderm) (1).
Location: More than 99% are found wedged in the foramen of Monro.
The cysts are typically attached to the anterosuperior portion of the third ventricular roof (1).
Age of presentation: Early middle age.
30-40 years of age.
Imaging: The cysts are smooth and spherical,
varying in size from 0.3 cm to more than 4 cm in diameter.
The best diagnostic clue to a colloid cyst is its location at the foramen of Monro (1) ( Fig. 13 ).
CT: Well-delineated hyperattenuated mass on nonenhanced CT (1).
MR: On T1-weighted MR images,
two- thirds of colloid cysts are hyperintense.
The majority are isointense to brain on T2-weighted images.
Some demonstrate peripheral rim enhancement (1).
Differential Diagnosis: CSF flow artifact (1).
2.2.8.
Neurocysticercosis
Mentioned previously.
See ( Fig. 6 )
2.2.9.
Abscess
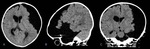
Definition: Cerebral abscesses result from pathogens growing within the brain parenchyma.
Initial parenchymal infection is known as cerebritis,
which may progress into a cerebral abscess (11) ( Fig. 14 )
Location: Brain parenchyma.
Age of presentation: All age groups of age affected.
Imaging: Early and late encapsulation.
Differential Diagnosis: Metastases,
high-grade glioma,
contusion,
radiation necrosis (11).
We present a summary table with cerebral cystic lesions and their most frequent location (1) and age of presentation ( Table 2 ).