The most used imaging technique for the extension study and the follow-up of these patients is CT.
However,
for the detection of cerebral metastases or when the tomographic study is inconclusive,
MRI is the technique of choice due to its superior tissue characterization.
The ultrasound is limited to the assessment of the scar area and the study of locoregional lymphatic chains.
PET-CT is also useful in the monitoring of maetastatic melanoma because of its ability to assess the entire body in a single study,
however it has low specificity and low resolution when the lesions are small.
Ultrasound (US),
CT and MRI all have the ability to identify locoregional and distant metastases but their use in asymptomatic patients with early stage melanoma is not generally indicated.
However,
in patients with tumours with a thickness > 2 mm,
we routinely perform CT studies of the neck,
chest,
abdomen and pelvis,
and US studies of the scar area and regional lymph nodes.
Generally,
on CT without contrast enhancement,
melanomas appear isodense to hyperdense relative to muscle,
and they enhance due to their hypervascularity.
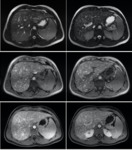
On MRI,
melanomas are classically hyperintense on T1-weighted images because of their melanin content.
However,
melanomas have a tendency to bleed in up to 50% of cases,
so the hemorrhage itself would also contribute to T1 signal shortening.
In fact,
T1 hyperintensity due to melanin is present in only 24-47% of lesions,
associated with those that have more than 10% of cells containing melanin.
On T2-weighted images,
melanomas are classically hypointense because of the paramagnetic effects of melanin.
Restricted diffusion is usually present due to tumor hypercellularity.
We will review the possible forms of presentation of metastatic melanoma according to its location,
based on the most representative cases in our center in the last 5 years.
Skin,
subcutaneous tissue and lymph nodes
Ultrasound shows greater utility in lesions located on skin,
subcutaneous tissue and lymph nodes,
both in the assessment of the area of the scar and in the diagnosis of satellite (within 2 cm of the primary tumor),
"in transit" (more than 2 cm from the primary lesion but not beyond the regional nodal basin) and locoregional lymph node metastases.
Lymph nodes metastases not accesible to ultrasound evaluation are usually imaged on CT,
and it has been necessary to establish size criteria and the pattern of enhancement to define the likelihood of involvement (fig.
3-6).
Affectation of the subcutaneous tissue usually occurs by direct extension although it may also be secondary to hematogenous spread.
They are usually seen as well-defined nodules of different sizes,
hypodense with peripheral enhancement after contrast administration (fig.
7-8).
In CT studies this lesions are often conspicuous because of the low density of normal fat around them.
Grayscale US shows hypoecoic nodules and prominent Doppler flow signal as a result of a disorganized neovascularization (fig.
9-10).
Thorax: pleura and lungs.
Melanoma has a high propensity to metastasize to the lung where it can present as a solitary nodule or,
more frequently,
as multiple,
rounded and well-defined nodules.
In fact,
respiratory failure caused by replacement of lung tissue by metastases is the most common cause of death from malignant melanoma.
Pleural metastases usually appears as soft tissue nodular thickening indistinguishable from other entities.
They can show a homogenous enhancement when they are small or heterogeneous enhancement due to areas of necrosis secondary to their rapid growth (fig.
11). They may also associate with pleural effusion,
usually unilateral.
CT has been shown to be the most accurate imaging modality for detection of both lung and pleural metastases.
PET-CT it is also useful in these cases.
Brain
Cerebral metastases usually occur in late stages of the disease and they are associated with the worst prognosis of all visceral sites with a median survival rate of 4 months.
They are often multiple metastases and commonly located at the grey matter-white matter junction of the supratentorial compartment.
On MRI images,
malignant melanoma may show melanotic (high signal intensity on T1-weighted images and low signal intensity on T2-weighted images) (fig.
12-13) and amelanotic patterns (hypointense or isointense to the cortex on T1-weighted images and hyperintense or isointense to the cortex on T2-weighted images) (fig.
14) depending on the percentage of melanin present in the lesion,
and its frequent bleeding (fig.
15-16).
T1-weighted imaging is useful for detecting melanotic pattern and hemorrhage since they may appear similar in T1 weigted images.
T2*-weighted sequences shows signal loss in bleeding because of metahemoglobin susceptibility effect, but in some studies is not as strongly correlated with melanin content,
despite its paramagnetic effect.
T1-weighted postgadolinium sequences are useful to detect solid areas with avid enhacement.
T2 and FLAIR sequences better show digitiform oedema.
However there is frequent deviation from these usual patterns such as small and rapidly growing metastases,
milliary metastases and subependymal metastases.
Abdomen: liver,
spleen,
gallbladder
The liver is the third most common site of metastases melanoma.
The appearence of liver metastases on US studies is hypoechoic and on CT studies is variable,
but the majority of them are hypodense when compared to the normal parenchyma.
They can be single or multiple,
variable in size and may be partly calcified.
They often present necrotic areas,
especially larger lesions and they are best detected on contrast-enhancement studies because of its hypervascularity.
Melanoma liver metastases may or may not contain enough melanin so they can appear hyper / hypointense on T1-weighted MRI images (fig.
17-21).
Generally,
the spleen is a rare site for metastatic disease but up to 30% of metastatic melanoma patients have splenic involvement in later stages of the disease. Splenic metastases also are variable in appearence on CT and MRI.
Lesions may be solid or cystic and variable in size (fig.
22).
Melanoma accounts for more than half of metastases to the gallbladder.
It is unknown why melanoma tends to metastasize to the gallbladder.
They are usually clinically occult and,
for this reason,
are rarely discovered in living patients.
US is the most useful modality for assesing the gallbladder for metastatic melanoma.
They begin as small,
flat nodules that progress to polypoid or pedunculate masses (fig.
23).
Because of their low density,
tumor masses do not exhibit acoustic shadowing.
On CT scans the gallbladder shows focal irregular wall thickening,
or enhancing intraluminal polypoid masses.
PET-CT can help correctly identify this metastases (fig.
24).
Mesentery and peritoneum
Mesenteric involvement can mimic lymphoma with single or multiple nodules infiltrating the mesentery or omentum.
Peritoneal nodules or carcinomatosis can be present (fig.
25).
They may present as different sizes,
lobulate,
confluent or infiltrative (fig.
26-29).
Genito-urinary system
The adrenal gland is the most frequently invaded endocrine organ.
Adrenal metastases may be bilateral (fig.
30) although typically are unilateral as in others metastatic disease.
Their appearence is not specific,
are variable in size (mean diameter of 4 cm),
round or lobulate,
with soft-tissue density and heterogeneously enhancement.
Most patients have other sites of metastatic disease sites as well.
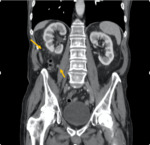
Melanoma can metastasize from the kidneys to the bladder,
causing sometimes hydronephrosis or haematuria.