NEUROBLASTOMA
Neuroblastoma (NB) is a malignant tumour of embryonic origins which arises from sympathetic cells which originate from neural crest.
Head-neck primitive location of the neoplasia is rare[2][3].
Tumour imaging features are the basis of all pre-treatment risk classification of NB affected patients.
In head-neck tumours,
ultrasound represent first level imaging technique,
particularly in paediatric patients [6].
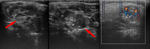
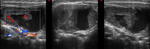
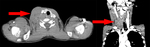
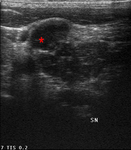
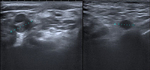
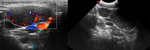
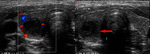
On ultrasound examination the tumour appears as a solid heterogeneous echogenic lesion with intralesional fine or coarse calcifications.
Fine calcifications result in a diffuse increased echogenicity of the lesion while coarse calcification appear as a focal echogenic spot usually without distal shadowing (Fig.
1) [7].
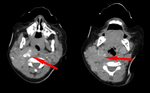
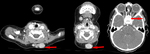
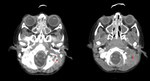
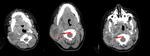
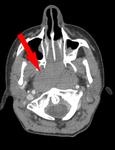
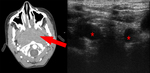
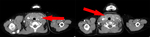
On CT scans the lesion appears like a lobulated mass with soft tissues density with poor enhancement after contrast media administration.
The presence of coarse and sometimes curvilinear calcifications is a typical imaging feature (Fig 2 – 3 – 4).
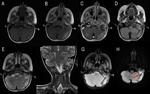
MR is superior to the CT in the evaluation of paravertebral extension,
leptomeningeal and cervical medullary involvement [8].
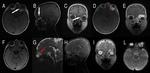
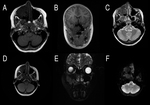
On MR acquisitions the lesions show heterogeneous signal,
hypointense on T1 weighted sequences and hyperintense on T2 weighted images.
Intratumoral necrosis can be demonstrated by the presence of cystic and hemorrhagic areas.
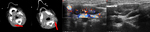
On diffusion weighted imaging (DWI),
the lesions appear hyperintense due to restricted perfusion caused by hyper-cellularity of the tumour mass (Fig.
5).
Bone marrow disease is usually seen as presence of lesions with hyperintense on T1 and hypontense on T2 appearance,
usually with diffuse aspect and rarely with a nodular pattern [7].
Scintigraphic studies with MIBG have a role in evaluating distant bone marrow involvement[9].
RHABDOMYOSARCOMA
Sarcomas are relatively rare pathologies but in paediatric population they represent the most common malignant neoplasia,
with a 8% prevalence in total [10].
The rhabdomyosarcoma (RMS) shows a dicotomic incidence distribution with two peaks; incidence is about 4,3 cases/1 million [11].
In most cases etiopathogenesis remains unknown[12].
There are three sub-types: embryonal RMS (botryoid or spindle cell variants),
alveolar RMS and pleomorphic.
Although RMS may arise in every body districts,
it involves more frequently the head-neck and genito-urinary district[13].
When the tumour involves the head-neck district,
in paediatric age,
we may observe a para-meningeal localization in 50% of cases,
a peri-orbital localization in 25% of cases and in 20% of cases it involves other sites [14].
A correct diagnosis can only be achieved with more advanced tomographic modalities such as CT and MR.
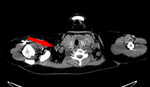
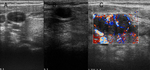
Ultrasonography usually demonstrates an expansive and infiltrating mass with an inhomogeneous iso- or hypo-echogenicity with intra-lesional haemorrhagic or colliquative areas,
hyper-echogenic spots such as calcifications are rarely seen; Doppler analysis might show anarchical angiogenesis within the lesion.
Differential diagnosis are fibrosarcoma,
histiocytoma,
angiosarcoma and neurofibrosarcoma (Fig.
6).
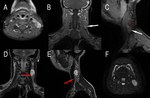
MR studies are useful to evaluate tumour extension and treatment response in pelvic,
para-spinal and extremities masses,
however CT scans show superior sensitivity in the evaluation of bone and lymph nodes involvement (Fig.
7) [15].
The tumour shows hyper-intense signal on T2 weighted sequences and appear iso-intense to the muscle in T1 weighted sequences; contrast media administrations determines high enhancement of the lesions (Fig.
8 – 9)[15].
Positive prognostic factors include absence of metastatic disease at the time of the diagnosis,
disease free resection margins,
mass dimension below 5 cm and patients younger than 10 years[16][17].
THYROID CARCINOMA
Thyroid carcinomas represent about 0,5-3% of all tumours in paediatric population[18][19].
Most relevant risk factors include family history of thyroid tumours or other thyropaties and familiarity for multiple endocrine neoplasia[20][22][23][24].
In paediatric population a higher probability of lymph nodes secondary involvement or distant metastasis has been demonstrated [25].
Clinical signs include sudden onset hyperthyroidism,
compression signs such dysphonia and dysphagia,
local lymph nodes enlargement[26].
Echotomographic examination can evaluate single or multi-nodular neoplasia,
nodules dimensions,
echogenic pattern and presence of microcalcifications as well as lymph nodes involvement and vascularization patterns of the lesions and lymph nodes [27].
Ultrasound features include lesion hypoechogenicity,
irregular margins,
presence of microcalcifications,
lymph nodes abnormalities,
such as round and pseudo-cystic aspects (Fig.
10 – 11)[28].
CT neck scan is useful to identify sub-centimetric lesions and evaluate lymph node involvement,
as well as nodular lesions characterization,
however it demonstrated poor reliability in the determination of the nature of the lesions [29].
Ultrasound-guided fine needle aspiration represent the gold-standard for the diagnosis of carcinoma[30].
This procedure can be executed on nodules greater than 1 cm[31].
In MEN-2 syndrome prophylactic thyroidectomy is recommended [32].
Serum thyreoglobulin level must be used as a marker of relapse [33].
To achieve a complete therapeutic success,
a long follow-up with ultrasound is recommended[24].
LYMPHOMA
Lymphomas belong to a heterogeneous group of neoplastic pathologies arising from lymphoid tissues; they represent about 10-15% of all neoplasia during paediatric age.
Hodgkin lymphoma (HL) reaches peak incidence during puberty,
while Non-Hodgkin Lymphomas (NHL) are more frequent in patients younger than 10 years old and in males [34].
Most frequent localizations in NHL are mediastinum or abdomen.
Tumour staging,
which differs between HL and LNH,
depends on different lymph nodes stations involved,
extra-lymph nodes extension and presence of signs or symptoms of systemic involvement.
LH staging in paediatric patients depends on Cotswold’s classification [35] while St.Jude classification is used for NHLs [36].
Morphologic criteria used to define suspect nodules are represented by nodules with axial diameter greater than 1,5 cm.
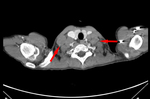
Although CT represents the most sensitive modality for deep and/or small lymph nodes detection (mediastinal or abdominal),
the administration of contrast media is not always useful to discriminate their malignant nature (Fig.
12 – 13 – 14 – 15 – 16)[37].
Echographic criteria for malignant lymph nodes characterization include volume enlargement,
round aspect,
vascular structure distortion,
presence of aberrant or eccentric vascular hila,
sub-capsular vessel distortions,
necrotic areas or lack of vascular signal,
sovra-clavear localization (Fig.
17 – 18 – 19 – 20 – 21 – 22 – 23)[38].
Cervical lesions during paediatric age fall into differential diagnosis with numerous inflammatory pathologies,
benign neoplastic lesions and lympho-granulomatous diseases.
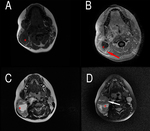
A complete MR examination should always include T1 sequences,
that due to their high anatomic detail are useful in the evaluation of loco-regional soft tissues and bone involvement,
except in sino-nasal or ethmoidal localizations where CT scans demonstrated higher accuracy[39].
Meningeal secondary involvement must be suspected when a meningeal thickening greater than 5 mm is seen or in the presence of focal nodularities[40].
Lymph nodes involvement features volumetric enlargement of lymphatic tissue,
with iso or hypo-intense appearance in T1 weighted sequences and hyper-intense in T2 or STIR acquisitions.
After contrast media administration,
the lesions show mild enhancement.
Staging and therapy response evaluation,
particularly in paediatric patients can be achieved through “whole body” PET-CT scans with 18-FDG[41].