Management of gastrointestinal bleeding is primarily endoscopic according to the predominance of peptic ulcer disease with a great success rate (85 to 90%). In case of failure of a first endoscopy,
a second must be attempted,
with as much as possible the “marking” of the bleeding site by clips.
After two unsuccessful endoscopic treatment attempts,
are positioned interventional radiology with embolization and surgery,
guided by abdominal angio-CT,
with similar results. Embolization should be preferred to surgery especially in risky patients,
because of co-morbidities and coagulopathy.
OVERVIEW
EPIDEMIOLOGY
1.
Annual incidence: 65000 cases per year.
1% in people over 80’s
2.
Upper gastrointestinal bleedings
Incidence: 100 to 150/100 000
2000 deaths including 97% related to comorbidity (advanced age,
cirrhosis,
cancer ...).
PROGNOSIS
Spontaneously favorable evolution in 80% of cases
Mortality rate: 5-10% BUT this rate in patients who continue to bleed increases to 40%
In practice,
2 clinical situations guide the management
1.
Upper gastro-intestinal bleeding other than cirrhosis
2.
Hemorrhage in a cirrhotic patients (not traited in our work).
Clinical orientation
1.
History of peptic oeso-gastroduodenal pathology,
NSAIDs,
Aspirin.
2.
Detecting underlying chronic liver disease +++.
ANATOMIC FEATURES
The majority of digestive hemorrhages are from arterial origin.
There is a large anastomotic network that allows embolization procedures with low ischemic risk when embolization is very close to the pathological site.
The collaterals are also a source of bleeding recurrence.
The recall of arterial anatomy is an essential prerequisite for CT angiography analysis and for interventional procedures.
Vascularization of the stomach and the duodenum comes mainly from the celiak trunk.

Fig. 1
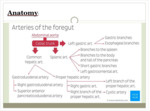
THE STOMACH
Arterial blood supply through the 3 branches of the celiac trunk : arch anastomoses.
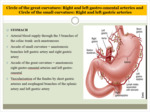
The circle of the great curvature is realized by by the right and left gastro-omental arteries and circle of the small curvature: Right and left gastric arteries).
- Arcade of small curvature = anastomosis branches of the left gastric artery and right gastric artery.
- Arcade of the great curvature = anastomosis of the right gastro-omental arteries and left gastro-omental.
- Vascularization of the fundus is realized by short gastric arteries and esophageal branches of the splenic artery and left gastric artery.

Fig. 2
THE DUODENUM
Peri-pancreatic arches are realized by the anterior,
posterior,
superior and inferior between gastroduodenal artery and superior mesenteric artery.
- Arterial blood supply of the common bulb with that of the pylorus (right gastric and right gastro-omental arteries).
- Vascularization of the rest of the duodenum indissociable from that of the head of the pancreas and the termination of the main bile duct.
- The duodeno-pancreatic arteries form two anastomotic arches,
anterior and posterior,
between the celiac system (via the middle and gastroduodenal hepatic arteries) and the superior mesenteric artery.
- The duodeno-pancreatic veins are satellites of the arteries and drain into the portal vein.

Fig. 3