We reviewed MRI studies of cases with clinical suspect of spondylodiscitis of the last two years.
Protocol used include MRI sequences (T1,
T2 ,
STIR and T1 after Gadolinium).
To complement this,
are reviewed previous studies CT,
specifically those containing vertebral collapse,
and medical histories are analyzed if unexpected evolution,
histopathological diagnosis exclude the presence of infection in disk or vertebral biopsy or other non-typical findings of spondylodiscitis.
MRI is the imaging technique preferred by their high sensitivity and specificity to diagnosis of spondylodiscitis.
CT values posterior elements,
vertebral canal and perivertebral tissues.
Besides osteolysis,
sclerosis eroded plates,
erosions,
geodes,
bone sequestration ,
residual calcifications.
Gas within paraspinal soft tissues abscesses are more evident,
on the contrary,
it does not clearly assess the extent of abscesses in the epidural space or foraminal.
It serves as a guide for percutaneous biopsy and for the drainage of abscesses.
Most frequent findings in MRI of spondylodicitis are the pattern of edema of the bone marrow on both sides of vertebral body surface (earliest sign),
disk and vertebral enhancement after gadolinium administration,
endplate erosion ( the more specific sign) and may extend subligamentous,
into the epidural space and the paravertebral soft tissues.
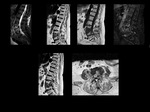
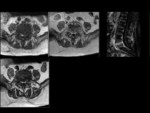
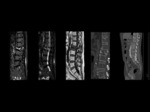
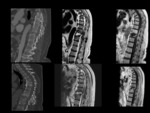
Typical alterations of acute spondylodiscitis in earlier stages involve bone marrow on vertebral endplate and of the adjacent vertebral bodies with edema-inflammation and fluid collections as hypointense on T1,
hyperintense on T2,
enhancement post contrast sequences with fat saturation of vertebral endplates ,
peripheral enhancement around fluid collection and cortical bone erosions as loss of low signal cortex at endplates.
Loss of heigh of disk space with edema-inflamation and fluid collection as low signal on T1,
high signal on T2,
enhancement post contrast sequences with fat saturation.
Perivertebral soft tissues: subligamentous,
epidural and paravertebral with edema-inflammation as high signal on T2,
enhancement post contrast sequences with fat saturation.
Enhancement around low-density centre indicates abscess formation.
Fig 1.
In chronic forms or in delayed diagnosis,
high signal in T2 and STIR,
and Gd enhancement of the bone marrow,
epidural tissue and paravertebral,
as an expression of inflammation,
are decreasing.
In the end,
the bone marrow is replaced by fat (hyperintense in T1 and isointense in T2),
fibrosis or sclerosis (hypointensity in T1 and T2).
Sclerosis of irregular endplate can be observed.
Destruction of the vertebral body may have progressed to a collapse.
This feature,
vertebral collapse,
and epidural and paravertebral soft tissue inflammation could be shared with vertebral osteonecrosis,
similar radiological findings between both entities that we detect in our experience.
And besides clinical presentation may be also similar.
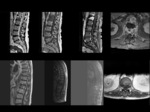
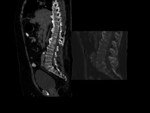
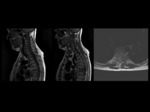
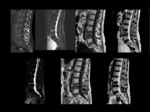
Epidural and paravertebral soft tissue inflamation secondary to osteonecrosis vertebral as consequence of extension of liquid from the subchondral necrotic cavity in the upper margin of the vertebral body ( avascular zone develops below the superior endplate). Fig 2,
Fig 3,
Fig 4,
Fig 5,
Fig 6.
Intravertebral vacuum and intravertebral fluid are described in benign vertebral osteonecrosis on MR images.
Both of them are typical radiological findings of vertebral osteonecrosis,
helping to the differential diagnosis is presented with other causes of vertebral collapse such as infection or neoplasia.
Fluid sign is seen in 12-50% of osteoporotic collapse and 5-6% of pathological collapse,
rarely occurs in metastatic fractures.
The presence of the intravertebral fluid sign is a strong predictive factor for the benign cause of a fracture.
(13).
It would be useful in the differential diagnosis between osteoporotic and neoplastic vertebral compression fracture.
In this way,
this finding,
together with other characteristics that we quote below,
makes it possible to distinguish between osteoporotic or benign collapse and malignant origin.
Osteoporotic collaps following known or unknown trauma.
Fluid and edema replacing the fatty marrow in acute osteoporotic collapse appears hypointense in T1,
iso to hyperintense in T2 and hyperintense in STIR. Common morphology of fluid sign is linear signal subjacent to the anterior part of superior end plate.
Involvement of intervertebral may rarely be seen in cases of osteoporotic or traumatic collapse.Normal posterior concave contour and intact pedicles. Bone fragmentation with dorsal angulation or retropulsion of bone fragments of bone fragment is common feature of benign collapse.
Paraspinal mass is seen rarely.
Malignat collapse however secondary deposits in vertebral bodies are usually well defined and rounded lesions.
Anterior or posterior margins of vertebral bodies show bulged contours.
Pedicle involvement is common in metastasis.
Paraspinal or epidural soft tissue masses.
Involvement of intervertebral disk is rare.
No bone fragmentation. (4,
16,
18) Fig 7,
Fig 8.
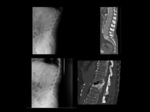
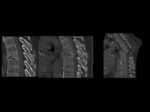
Vertebral osteonecrosis is usually suspected when the intervertebral vacuum cleft sign is present.
It is more easily seen on CT as air attenuation in the central area or adjacent to the upper endplate of a collapsed vertebral body,
whereas all MR imaging sequences will show a signal intensity void.
(10,
11)
Intravertebral vacuum cleft was described in osteoporotic vertebral compression fractures is due to nonunion within the fracture cleft.
Formerly,
this has been attributed to ischemic osteonecrosis of bone,
also known as Kümmell disease.
Ischemia produces bone necrosis causing an intraosseous cavity; the low pressure in this cavity favors the accumulation of gas,
mainly nitrogen.
Besides a similar phenomenon to vacuum phenomena are most commonly seen in patients with intervertebral osteochondrosis,
where dehydration of the disk and enlarging clefts within the nucleus pulposus lead to the accumulation of gas from the surrounding tissues,
appearing as a radiolucent area in the discal space in radiographs and CT scans.
Time-dependent accumulation of fluid within the intravertebral clefts has been described,
with the amount of fluid depending on the duration of supine positioning.
Intradiskal gas may migrate into fractured vertebral bodies, however,
suggest that the intradiskal air may come from intravertebral gas.
(11).
Discal space or soft tissue extension of the gas from intervertebral gas demand the differential diagnosis with infection.
Intravertebral vacuum cleft sign is probably not pathognomonic of Kummell’s disease,
but may be highly suggestive of it (17).
The fluid sign has been described in cases of vertebral osteonecrosis,
mainly on MR imaging.
It is a collection of intravertebral fluid was adjacent to the fractured endplates and exhibited a circumscribed area of fluidlike hypointensity on T1-weighted images and hyperintensity on T2-weighted images.
Histologic analysis will show reactive marrow fibrosis with high turnover rate,
which indicates osteonecrosis,
edema,
and fibrosis at the site of the fluid sign.
In acute vertebral compression fractures ,
the fluid sign,
is featured that show bone marrow edema.
The fluid sign was significantly associated with osteoporotic fractures and was significantly associated with fracture severity.
There was a tendency toward older fractures exhibiting the fluid sign,
but this relationship was not significant.
Studies (1) demostrated MRI fluid could be reliable for predicting osteonecrosis vertebral in vertebral fracture caused by minor trauma.
Therefore,
patients,
who sustained vertebral fractures caused by low-energy trauma and presented with surgical indications and MRI fluid signs,
should be highly suspected to have vertebral osteonecrosis vertebral,
especially within the initial 5 months after injury.
Osteonecrotic vertebral collapse usually has an increased signal on T1-weighted images and decreased signal on T2-weighted images.
Chronic osteoporotic fractures usually are not associated with MRI signal changes.
In addition,
a linear area of hyperintensity with surrounding hypointensity can be seen on MRI in cases of Kummell’s disease and spontaneous vertebral osteonecrosis.
Collapses were more frequent in patients with only intravertebral gas than in those with only intravertebral fluid.
(11).
Intravertebral fluid may represent a subsequent phase of vertebral osteonecrosis that precedes the development of intravertebral air.
The stage of vertebral osteonecrosis is late when intravertebral air appears and indicates a tendency for vertebral collapse in adjacent levels for those without this air.
(11).
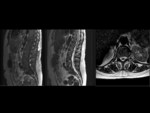
Fig 9,
Fig 10,
Fig 11.
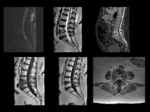
Extensive lysis in the vertebral body that may be important with great loss of height,
the fluid occupying much of the vertebral body and may extend into the disk or adjacent soft tissues forcing the differential diagnosis with infectious or neoplastic processes,
even to be performed biopsy of the collection.
The well defined delimitation of bone resorption in the cavity,
the absence of solid component and inflammatory tissue surrounding the collection are typical data that should be considered for diagnosis.
Evolution of the loss of height of the vertebral body,
little involvement of the intervertebral disk and vacuum effect as typical findings of osteonecrosis vertebral. Fig 2,
Fig 3,
Fig 4,
Fig 5,
Fig 6.
Absence of progressive neurological deficit or signs of infection,
knowledge of these features can expedite reduce potentially unnecessary procedures and help to provide treatment as vertebral cement augmentation,
with the expectation of immediate and good to excellent resolution of pain.
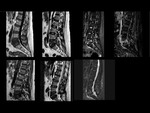
Vertebral compression fractures with torpid evolution in patients with risk factors and delayed treatment may evolve into spondylodiscitis.
Fig 12 ,
Fig 13.