Learning objectives
-Recognize vertebral osteonecrosis as a possible complication of vertebral compression fracture in osteoporotic bone,
mainly,
or late post-traumatic diagnosis (Kummell's disease).
- Identify radiological findings of spondylodiscitis.
Given that,
despite clinical suspicion,
if expected radiological findings are not objectified or there are discrepancies with other diagnostic tests; vertebral osteonecrosis should be included as a possible diagnosis,
especially if there is vertebral collapse.
Background
Spondylodiscitis can mimic many other pathologies,
such as degenerative intervertebral disease ,
inflammatory spondyloarthropathies,
neoplasms and compression fractures.
These noninfectious conditions may simulate a spondylodiscitis by showing similar features.
It is helpful to be aware of these diseases and their MR imaging features.
If endplate destruction,
increased disk signal intensity on T2WI,
enhancement after contrast,
or paravertebral or epidural abscess is present,
infectious spondylitis,
rather than Modic type 1 degeneration,
should be suspected.
(3)
To distinguish tumor involvement: posterior elements and non-contiguous vertebral bodies may...
Findings and procedure details
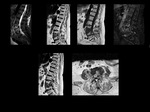
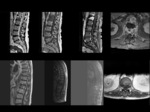
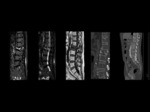
We reviewed MRI studies of cases with clinical suspect of spondylodiscitis of the last two years.
Protocol used include MRI sequences (T1,
T2 ,
STIR and T1 after Gadolinium).
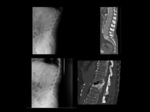
To complement this,
are reviewed previous studies CT,
specifically those containing vertebral collapse,
and medical histories are analyzed if unexpected evolution,
histopathological diagnosis exclude the presence of infection in disk or vertebral biopsy or other non-typical findings of spondylodiscitis.
MRI is the imaging technique preferred by their high sensitivity and specificity to diagnosis of spondylodiscitis.
CT...
Conclusion
-Vertebral osteonecrosis is an entity that must be included in the differential diagnosis of spondylodiscitis when all the radiological criteria are not met,
especially in patients with collapse vertebral.
-It is very important to correlate with antecedents,
previous imaging studies,
clinical evolution and other diagnostic tests (laboratory,
anatomopathological): radiological follow-up may be the key.
References
1.
Dupuy DE,
Palmer WE,
Rosenthal DI: Vertebral fluid collection associated with vertebral collapse.
AJR Am J Roentgenol 167:1535-1538,1996
2.Baur A,
Stabler A,
Arbogast S,
et al Acute osteoporotic and neoplastic vertebral compression fractures: fluid sign at MR imaging.
Radiology 2002; 225:730–735.
3.
Sung HH,
Ja-Young C,
et al.
MR Imaging Assessment of the Spine: Infection or an Imitation?.
RadioGraphics 2009; 29:599–612.
4. Yuh WT,
Zachar CK,
et al.
Vertebral compression fractures: Distinction between benign and malignant causes with MR imaging.
Radiology 172:215-218,
1989.
5.Tins...