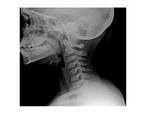
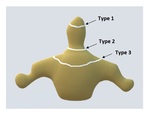
Development and normal anatomy of the cervical spine:
Chondrification of the vertebral bodies occurs around the fifth or sixth gestational weeks.
Primary ossification centers are present in all the vertebral bodies by the fourth month.
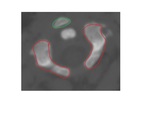
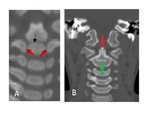
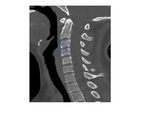
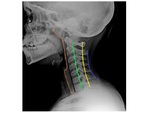
The C1 vertebra has a unique anatomy Fig. 1,
three primary ossification centers; one for the anterior arch,
and two for the posterior neural arches separated by synchondroses Fig. 2 .
At birth,
the neural arches are ossified but the anterior arch is not.
The anterior arch undergoes ossification by three months of age in 33% of children and by the age of one year in 81% of children.
Fusion of the posterior neural arches occur by 3 to 4 years of age,
and fusion of the synchondroses between the body and the posterior elements occur by 7 years of age.
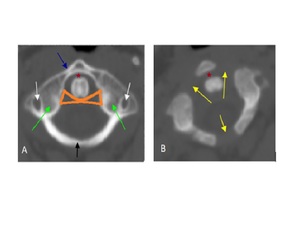
Fig. 1: Normal C1 anatomy (A) the complete ring of atlas consists of anterior arch (blue arrow) and posterior arch (black arrow), foramen transerversarium (white arrow), superior articular facets (green arrow), atlanto- axial articulation (red asterisk) and the diagramatic illustration of the transverse ligament (orange diagram), (B) showing opened neurocentral synchondrosis (yellow arrows).
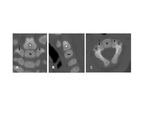
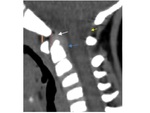
The axis has four primary ossification centers; with two ossification centers forming the dens Fig. 3 .
The C2 body fuses to the odontoid between 3 and 6 years of age.
The posterior arches fuse at their midline by 2 to 3 years and fuse with the body by 3 to 6 years.
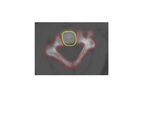
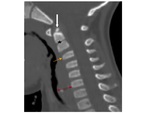
The secondary ossification center at the tip of the odontoid Fig. 4 appears between 6 and 8 years of age and fuses with the dens around 12 years of age.
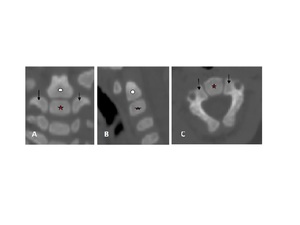
Fig. 3: CT cervical spine (A) coronal, (B) sagittal reformat and (C)axial view showing the primary ossification centers of the axis; one for the vertebral body (red Asterisk), one for each neural arch (arrow), and one for the dens (white circle).
- The sub-axial cervical spine:
The development of the sub-axial cervical spine has a common pattern between C3 through C7 comprising a single ossification center for the vertebral body and an ossification center for each neural arch Fig. 5 .
The arches fuse in the midline by the second to third year and fuse to the body between the third and the sixth year.
Five secondary ossification centers develop at the anterior transverse processes,
spinous process apices,
and superior and inferior epiphyseal rings Fig. 6 .
The anterior transverse process fuses with the vertebrae at six years of age.
The latter three centers fuse by the age of twenty-five 2.
Cervical spine stabilizing Ligaments:
Primary stabilizing ligaments:
Secondary stabilizing ligaments:
Imaging protocol:
The Appropriateness Criteria of the American College of Radiology (ACR) indicate radiography as the imaging method of choice for children less than 16 years of age.
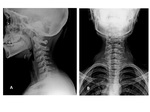
In children older than 5 years of age three views cervical X-rays should be done (anteroposterior,
lateral,
and open-mouth odontoid views) while in children younger than 5 years,
anteroposterior and lateral views radiographs are only needed Fig. 9 .
Flexion/extension views may be useful for further evaluation of prevertebral soft-tissue swelling or congenital abnormalities.
CT scans are needed in case of suspicion of cervical spine injury in radiographs,
or inability to obtain adequate X-ray and in patients with Glasgow score less than 8.
MRI is recommended to assess cord/soft tissue status.
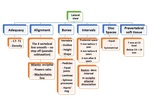
Approach to the cervical radiograph:
Lateral radiograph
It is the most important for evaluation of the potential cervical injuries. Fig. 10 .
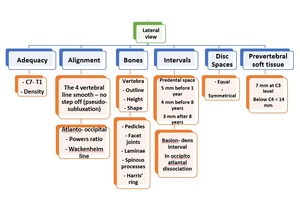
Fig. 10: Checklist for reporting lateral cervical x- ray.
-Vertebral lines: they should be aligned and parallel.
The anterior,
and posterior vertebral lines follow respectively the anterior and posterior aspects of the vertebral bodies.
The spinolaminar vertebral line follow the anterior aspects of the spinous processes.
The posterior cervical line is the upper end of the spinolaminar line Fig. 11 .
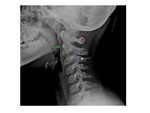
-Harris’ ring: ring-like structure resulting from projection of the lateral masses of C2 on its body.
it should remain unbroken Fig. 12 .
-Lines,
measurements and spaces Fig. 13 Fig. 14
- The atlantodental interval
- The basion axial interval
- The basion dens interval: normally < 12 mm.
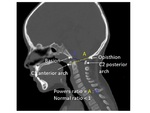
- The Wackenheim line: Fig. 15.
- The Powers ratio Fig. 16 .
- C1–C2 intraspinous distance (mm) < 12.
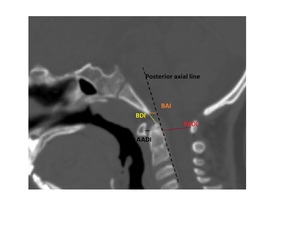
Fig. 13: CT cervical spine, midsagittal of normal patient illustrates, the basion-dens interval (BDI), anterior atlanto-dental interval (AADI), posterior atlanto-dental interval (PADI) and basion- atlanto interval (BAI) which is measured in-between the basion to the posterior axial line which is a line tangential to the posterior surface of C2.
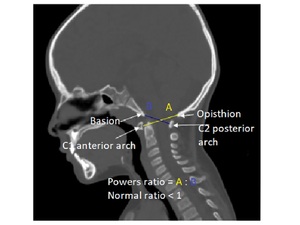
Fig. 16: How to calculate Powers ratio.
- Prevertebral soft tissues: prevertebral space of less than 7 mm at the C3 level is considered normal in children.
Below C4,
this space should not exceed 14 mm.
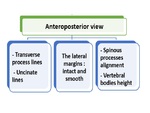
Antero- posterior radiograph:
This view is used to verify that the transverse process lines and uncinate lines are parallel and equidistant,
the spinous processes align and lie in the midline Fig. 17 .
Open-mouth radiograph (odontoid view):
This view is used to verify that the lateral masses of C1 do not overhang the articular masses of C2,
and are equidistant from the dens Fig. 18.
Radiographic variants and pitfalls of the pediatric cervical spine:
- Prevertebral soft-tissue pseudo-widening:
In children,
prevertebral shadow pseudo- widening on plain radiographs can result from expiration or crying.
For better assessment repeat x-rays during inspiration but if this is couldn’t be done,
CT is indicated Fig. 25 .
- Increased atlantodental interval (ADI):
The normal ADI in adults is less than 3 mm.
This distance can be normally up to 5 mm in the pediatric age group.
Increase in ADI > 5 mm means disruption of the transverse and accessory ligaments.
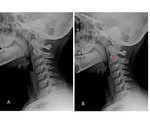
- Overriding of the anterior arch of C1 on the dens during extension:
Normal in 20% of children younger than 8 years old and it can be mistaken for atlantoaxial instability.
- C1 lateral mass displacement:
Up to four years of age C1 lateral mass displacement up to 6 mm is common and may be present till the age of 7 years
- Pseudosubluxation:
Pseudosubluxation of C2 on C3 is present in up to 24% of normal pediatric static cervical spine radiographs.
It can be noted in children up to 14 years.
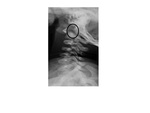
Swischuk proposed a method to differentiate pseudosubluxation of C2 on C3 from true instability.
A line is drawn from the anterior cortex of the posterior arch of C1 to the anterior cortex of the posterior arch of C3.
This line typically passes through or lie up to 1 mm anterior to the cortex of C2 posterior arch,
If the cortex is within 2 mm or more posterior to Swischuk line,
this indicates a true dislocation Fig. 19 .
Up to 14% of children have pseudosubluxation of C3 on C4 on lateral X-rays.
Full reduction of displacement on extension suggests pseudosubluxation rather than true instability.
- Variants of the atlas (C1):
- Occipitalization: congenital fusion of the atlas to the base of the occiput,
either partial or complete forms Fig. 20.
- Failure of ossification or fusion: whether at the anterior or posterior arches and it could take several forms Fig. 21; complete absence or hypoplasis,
failure of synchondrosis fusion and unilateral Fig. 22 or bilateral clefts .
- Arcuate foramen (posterior ponticle): is a bony bridge caused by ossification of the atlanto-occipital membrane,
associated with increased incidence of vertebral artery dissection.
- Accessory ossicle of the anterior arch.
- Variants of the axis (C2):
- Odontoid aplasia Fig. 26 / hypoplasia.
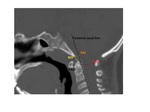
- Persistent ossiculum terminale and os odontoideum Fig. 24 .
- Dens bicornis.
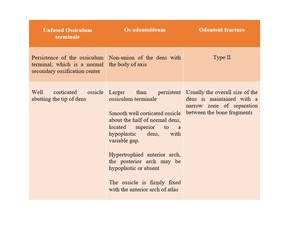
Fig. 24: Differential diagnosis for ossific density cranial to the dens.
- Persistence of subdental synchondrosis of C2
The synchondrosis can be differentiated from dens fracture by being well corticated and by its position below the level of the superior facets of C2.
- Ring apophyses:
They appear as thin wedge-like structures along the anterior inferior and superior borders of the developing vertebral bodies on a lateral radiograph Fig. 6 , usually seen at multi-levels,
begin to ossify at the age of 10 years and tend to fuse at age 17.
Complete fusion with the vertebral body occurs between 18 and 25 years of age.
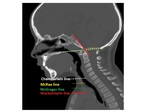
- Basilar invagination:
Abnormality at the craniovertebral junction,
the diagnosis depends on carniometric measurements: Fig. 14
- Chamberlain line
- McGregor line
- McRae line
- Non-symmetric closure of neurocentral synchondrosis:
Synchondrosis can be mistaken for fracture lines especially in case of non- symmetric closure,
yet they can be differentiated by their known locations and appearance as a smooth,
regular,
radiolucent line with a sclerotic border crossing the vertebral bodies.
- Vertebral body variants:
- Shape: In newborns,
cervical vertebral bodies have an ovoid appearance with increasing age,
the vertebral bodies assume a more rectangular shape.
A wedge appearance of the anterior aspect is a common intermediate stage,
and mild C3 wedging can persist until 12 years of age Fig. 25.
- Block vertebra.
- Hemivertebra.
- Loss of cervical lordosis: is a normal finding until the age of 16 years old.
Patterns of cervical spine injuries:
Young children less than 8 years of age tend to have upper cervical injuries (C3 or higher) whereas older children,
are prone to lower cervical injuries.
Instabilities:
- Atlanto-occipital and atlanto-axial dissociation injuries:
Dissociation injuries are either subluxations or dislocations; resulting from injury to the tectorial and alar ligaments.
Coronal and sagittal CT images can demonstrate unilateral or bilateral joint widening at O-C1 and/or C1–2.
At C2,
widening of the retropharyngeal space beyond 7 mm is a subtle sign of high cervical injury.
Power’s ratio >1,
basion-dens interval > 10 mm and basion-axis interval (BAI) and occipital condyle-C1 interval > 5mm,
atlanto- dental interval >5 mm and Wachenheim not intersecting the odontoid process.
- Atlantoaxial rotatory fixation (AARF):
This injury is an alteration of the normal rotational relationship between the atlas and axis.Type I AARF is rotary fixation with intact transverse ligament.
Types II and III injuries are rotatory fixation with anterior displacement of the atlas by 3-5 mm and > 5 mm,
respectively.
Type IV is posterior rotatory displacement of the atlas on C2.
AP radiography show asymmetry of the distance between the dens and lateral masses of atlas.
Functional CT examination in which patients turn their head to the maximum contralateral rotation show demonstrated fixed position of atlas with respect to axis and loss of normal rotation at the AA joint in case of atlantoaxial rotary fixation.
- Subaxial ligamentous injuries:
Mild forms may show no abnormality on CT or plain films.
More severe injuries may be associated with widening of facet joints,
widening or collapse of the disc space,
and separation of the spinous process.
White and Panjabi have suggested that more than 11° of angulation and/or 3.5 mm of subluxation between adjacent vertebrae implies significant ligamentous injury.
Fractures:
- Atlas fracture:
Burst fracture of C1 (Jefferson fracture) is caused by axial loading.
Isolated fracture of a synchondrosis may occur.
- Odontoid process fracture Fig. 27 :
It is the most common cervical spine fracture in children,
with the subdental and neurocentral synchondrosis being the most susceptible to injury,
typically in odontoid process fracture,
the dens is tilted posteriorly on lateral plain radiograph.
- Hagman’s fracture:
Bilateral pars fractures,
and anterolithesis of C2 on C3 vertebra,
most commonly confused with pseudosubluxation at C2-3 level,
displacement more than 2mm is pathognomonic of a true spondylolisthesis and swischuk’s line is useful to differentiate between them.
- Sub-axial cervical spine fractures:
The most common injury patterns include compression fractures,
burst fractures,
and facet fracture/dislocations.
-SCIWORA (Spinal Cord Injury Without Radiographic Abnormality):
MRI is the best for assessment of the spinal cord.
Acute spinal injury can be in the form of edema,
hematoma and cord transection.
Spinal cord edema appears as hyperintense T2 signal intensity and is best visible on STIR images.