We describe the imaging features of the anatomic variants (aberrant or accessory biliary ducts,
aberrant cystic duct insertion,
anomalous junction of the common bile duct with the pancreatic duct,
variations of the pancreatic ducts),
of developmental anomalies of the pancreas (pancreatic agenesis and hypoplasia,
ectopic pancreas,
pancreas divisum and annular pancreas) and the congenital diseases of the pancreatobiliary system (choledochal cysts,
congenital pancreatic cysts or von Hippel–Lindau disease).
Some of these entities can be clinically significant and the advances in the imaging techniques have contributed to the increased recognition.
IMAGING TECHNIQUES
The advances in Multidetector CT (MDCT) have improved image quality greatly and have contributed to the increased recognition of these entities.
Magnetic Resonance Cholangiopancreatography (MRCP) is the modality of choice for non-invasive evaluation of suspected anomalies of the pancreatobiliary tract.
It may depict the course and drainage pattern of the ducts and easily diagnose developmental anomalies of the pancreas.
Is especially appropriate for the assessment of congenital pancreatic anomalies since it depicts ductal anatomy rapidly and noninvasively without risk of acute pancreatitis.
MRCP also allows imaging of patients in which endoscopic retrograde pancreatography (ERCP) is unsuccessful and reveals portions of the pancreatic duct upstream from an obstructing lesion.
ANATOMIC VARIANTS
BILIARY SYSTEM
The right posterior duct has many anomalous insertions sites:
- Direct drainage of the RPD into the LHD before its confluence with the RAD is the most common anatomic variant of the biliary system.
- The RPD drain into the right aspect of the RAD.
- The “triple confluence” characterized by simultaneous emptying of the RPD,
RAD,
and LHD into the CHD to form a trifurcation.
These variants it is important in potential patients as donors for right hepatic lobe transplantation.
- The direct drainage of the RPD into the CHD,
also known as an “aberrant hepatic duct”,
is a less frequent variant.
Also,
can be accessory hepatic ducts (2%) with a course along the left or right ductal system.
Are three common variants in the cystic duct:
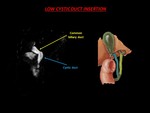
- A low CD insertion,
with fusion in the distal third of the extrahepatic bile duct (EBD).
- A medial CD insertion with drain into the left side of the CHD.
- A parallel course of the CD and the CHD for at least 20 mm.
PANCREAS
The MPD most commonly has a bifid configuration formed by the Wirsung and Santorini ducts.
Less common configurations are:
- A rudimentary duct of Santorini.
- A dominant duct of Santorini.
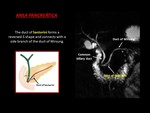
- Ansa pancreatica,
with a sigmoid curve of SD as it courses to the duct of Wirsung.
PANCREAS AND BILIARY SYSTEM
The pancreaticobiliary junction can be anomalous,
with a fusion of the Wirsung duct and CBD outside the duodenal wall,
formatting a long common channel,
which may allow reflux of pancreatic secretions into the biliary system,
helping in the formation of a choledochal cyst.
Also,
the reflux of bile into the pancreatic duct can cause pancreatitis.
DEVELOPMENTAL ANOMALIES OF THE PANCREAS
PANCREATIC AGENESIS AND HYPOPLASIA
The complete agenesis of the pancreas is very rare and is incompatible with life.
This absence of the gland has a relation with the mutation of a protein (IPF1).
The hypoplasia or partial agenesis is visualized as a short,
rounded pancreatic head adjacent to the duodenum with absence of the pancreatic neck,
body,
and tail.
The SD,
and the minor duodenal papilla can be absent too.
It may be a solitary finding or in association with other syndromes and many patients also have diabetes mellitus.
When agenesis of the dorsal pancreas is suspected,
it is indispensable to rule out pancreatic carcinoma with atrophy of the gland.
ECTOPIC PANCREAS
Occurs in 0.6%–13% of the population.
The ectopic tissue is in the submucosa in the 50% of cases and can be found more frequently in the stomach,
duodenum,
jejunum,
or ileum.
Rarely,
located in the colon,
esophagus,
liver,
gallbladder,
bile ducts,
etc.
The patients with this condition usually are asymptomatic,
however,
if the ectopic pancreatic tissue is functional,
it is subject to the same inflammatory and neoplastic disorders that involve the normal pancreas.
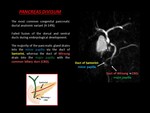
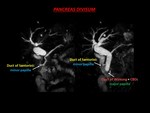
PANCREAS DIVISUM
Is the most common congenital anomaly of the pancreatic ductal system (4%–14% of the population).
Results when the ventral and dorsal pancreatic ducts fail to fuse.
The ventral duct or Wirsung drains only the ventral pancreatic anlage,
and most of the gland drains into the minor papilla through the dorsal duct or Santorini).
Focal dilatation of the distal portion of the SD (santorinicele),
it can be associated with pancreas divisum and relative obstruction at the minor papilla.
The clinical relevance of pancreas divisum remains controversial.
Most patients with pancreas divisum are asymptomatic but is more frequently seen in patients with chronic abdominal pain and idiopathic pancreatitis than in the general population.
MDCT only depict pancreas divisum when the pancreatic duct is visualized.
MRCP it is highly sensitive and specific for this condition,
showing the lack of communication between dorsal and ventral ducts,
independent drainage sites,
and a dominant dorsal pancreatic duct.
The WD is typically short and very narrow and the SD is typically larger.
The definitive diagnosis is made with ERCP.
ANNULAR PANCREAS
Is a rare congenital anomaly with an incomplete rotation of the ventral anlage,
which leads to a segment of the pancreas encircling the second part of the duodenum.
Has a prevalence of one in 20,000 persons and can occur as an isolated finding or with other congenital abnormalities.
In half of the cases,
will manifest in the neonate with gastrointestinal obstruction or bile duct obstruction,
possibly associated with pancreatitis.
In adults,
it may manifest with symptoms of “peptic ulcer disease,” duodenal obstruction,
or pancreatitis.
There are two types of annular pancreas:
- The extramural type,
where the ventral pancreatic duct encircles the duodenum to join the MPD.
- The intramural type,
in which the pancreatic tissue is intermingled with muscle fibers in the duodenal wall,
and small ducts drain directly into the duodenum.
On MDCT and MRCP,
the imaging findings reveal pancreatic tissue and an annular duct encircling the descending duodenum.
CONGENITAL DISEASES
BILIARY SYSTEM
Choledochal cysts are rare anomalies characterized by biliary tree dilatation.
Most of them are diagnosed in childhood with the triad of abdominal pain,
a right upper quadrant mass,
and jaundice,
but up to 20% manifest in adults.
This pathology has a female predilection.
The clinical manifestations are cholangitis due to bile stasis,
recurrent right upper quadrant pain,
fever,
and,
more rarely,
jaundice.
The choledochal cysts include the disorders characterized by dilatation of all or part of the extrahepatic (EBD) or intrahepatic biliary ducts (IBD).
There are 5 subtypes:
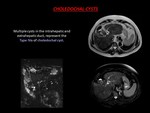
- Type I (Choledochal cyst): accounts for 80% to 90% of all bile duct cysts and are characterized by fusiform dilation of the EBD.
Can be subdivided into type Ia,
which involve the entire EBD; type Ib,
which involve only a focal segment of the EBD; and type Ic,
which involve only the CBD.
- Type II (Diverticulum): accounts for 3% of all bile duct cysts and represent a true diverticulum of the EBD.
- Type III (Choledochocele): accounts for 5% of all bile duct cysts,
represent ectasia of an intramural CBD segment and it is also known as choledochocele.
Typically,
manifest as focal dilatation of the intraduodenal segment of the distal CBD.
- Type IV (Multiple communicating intra and extrahepatic duct cysts): represent the second most common type of bile duct cysts (10%).
Are multiple and can have intrahepatic and extrahepatic components.
Can be subdivided into type IVa,
which involves both the EBD and the IBD; and type IVb,
which involve only the EBD with multiple saccular dilatations.
- Type V (Caroli’s disease): is a rare cystic dilatation of the IBDs.
It is an autosomal recessive disorder.
If the large IBDs are affected,
the result is Caroli’s disease.
If all levels of the intrahepatic biliary tree are involved,
the result is congenital hepatic fibrosis and Caroli disease,
which has been termed Caroli´s syndrome.
The imaging findings include intrahepatic saccular or fusiform dilated cystic structures that communicate with the biliary tree.
Intraluminal biliary calculi may be present.
The differential diagnosis is biliary hamartomas,
recurrent pyogenic cholangitis,
primary sclerosing cholangitis,
autosomal dominant polycystic liver disease,
and microabscess.
Other conditions who include choledochal cysts are,
cholangiocarcinoma,
and renal cystic diseases such as medullary sponge kidney and tubular ectasia.
PANCREAS
Congenital pancreatic cysts are exceedingly rare,
have a female predilection and manifest as an asymptomatic palpable mass.
May also produce epigastric pain,
jaundice,
and vomiting because of the compression of surrounding structures.
These cysts are most commonly located in the tail and body of the pancreas and can be single or multiple.
Multiple congenital cysts are associated with other anomalies,
such as von Hippel–Lindau disease and hepatorenal polycystic disease.
The von Hippel–Lindau disease is an autosomal dominant disorder characterized by retinal angiomas and central nervous system hemangioblastomas.
Pancreatic cysts are relatively common and can present from a single cyst to the cystic replacement of the gland.
Peripheral calcifications may also be present.