From 2013 to 2018 we diagnosed 20 cases of necrotizing pneumonia (13 male and 7 female).
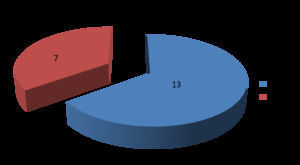
Fig. 1
The average age of these patients was 66 years old.
Only 5 of the total cases (25%) were immunosuppressed patients due to diabetes mellitus and neoplasia,
among others,
and 9 of the 20 cases (45%) were smokers.
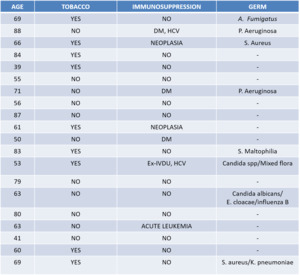
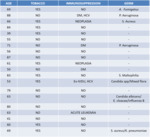
Table 1
In relation to bacterial etiology,
the most frequent was S.
aureus and P.
aeruginosa but is important to describe that the most common result in the culture was negative.
Fig. 2
The most common location of the disease was on the right lung and the most common lobe affected was the upper lobe.

Fig. 3
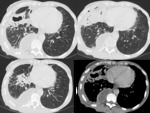
Below are the radiological findings in chest X-ray and in contrast-enhanced chest CT of some of the reviewed patients diagnosed of necrotizing pneumonia:
Case 1: An 83-year-old man with COPD who suffers an exacerbation secondary to respiratory infection with bad evolution:
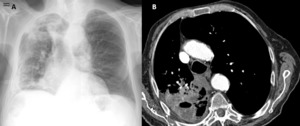
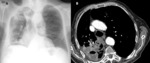
Fig. 4: A: Chest x-ray. B: Contrast-enhanced chest CT. Consolidation in the right upper lobe that presents air cavities in its thickness and conditions volume loss of the right lung with mediastinal deviation.
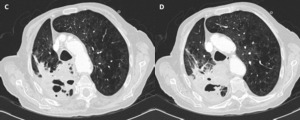
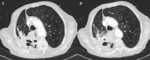
Fig. 5: C-D: Contrast-enhanced chest CT. Great centrilobular emphysema and consolidation in the right upper lobe with air cavities in its thickness that conditions loss of the right lung volume with mediastinal deviation.
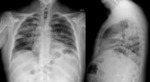
Case 2: A 53-year old woman ex-IVDU who suffers a respiratory infectious process with poor clinical evolution:
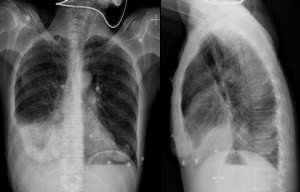
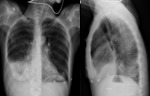
Fig. 6: PA and lateral chest x-ray: Right pleural effusion.
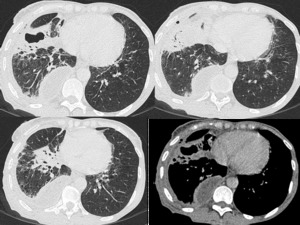
Fig. 7: Contrast-enhanced chest CT: Consolidation in the middle lobe with an air cavity and pleural effusión with the split pleura sign suggestive of empyema.
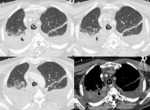
Case 3: A 55-years-old man with no medical history of interest suffers a respiratory infectious process with poor clinical evolution:
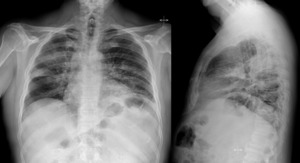
Fig. 8: PA and lateral chest x-ray: Consolidations in the right lung.
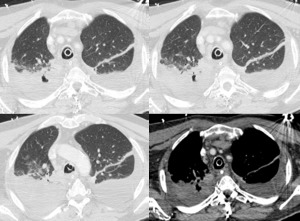
Fig. 9: Contrast-enhanced chest CT: Bilateral pleural effusion and consolidation in the upper right lobe with an air cavity inside.