INTRODUCTION
Brain tumor is a complex disease,
often with serious repercutions, especially when occurring in the posterior cranial fossa. Regarding by its location,
the posterior fossa tumors are considered critical,
as they can cause from hydrocephalus and ataxia to cranial nerve palsy, herniation and death.
Posterior fossa tumors are more common in children than in adults.
Between 54% and 70% of all childhood brain tumors originate in the posterior fossa while 15-20% of brain tumors in adults occur in the posterior fossa.
Magnectic Ressonance Imaging (MRI) can be used to acquire a big amount of information on posterior fossa tumors,
informations that go far beyond anatomy and include both metabolic as well as physiologic information by diffusion, perfusion,
MR spectroscopic,
and other more recently developed imaging techniques.
Have basic mastery of these informations that MRI gives helps the radiologists to adress a more accurate differential diagnosis.

Fig. 23
PILOCYTIC ASTROCYTOMA
- Cerebellar astrocytomas are the most frequent posterior fossa tumors in children and account for approximately 30ŌĆō35% of the cases.
- Usually occur in the latter half of the first decade,
mean age of 7 years old and rarely found in children less than 1 year of age.
- Approximately half are purely midline tumors,
but a lateral or hemispheric location is also seen.
- Cerebellar astrocytomas are usually sporadic,
but association with neurofibromatosis type 1 (usually seen with optic nerve or brainstem involvement),
Turcot syndrome,
PHACE(S) syndrome,
and Ollier's disease has been reported.

Fig. 5

Fig. 4
- Increased ICP
- Cerebellar deficits
- Papilladema (84%)
- Ataxia
- Hydrocephalus (85%)
- Median duration of symptoms before diagnosis is 5ŌĆÉ9 months
MEDULLOBLASTOMA
- A primitive neuroectodermal tumor (PNET),
first described in 1925
- Medulloblastoma is the most frequent malignant brain tumor of childhood,
is an invasive embryonal tumor with an inherent tendency to metastasize via the subarachnoidal space
- It accounts for approximately 20ŌĆō25% of all pediatric brain tumors and 40% of all posterior fossa tumors
- Median age 5ŌĆÉ7 years old,
they are rare in adults,
accounting for 1 to 3 % of all adult primary brain tumours
- Because of the fast growth,
clinical symptoms mostly develop rapidly and are typically related to intracranial hypertension and cerebellar ataxia
- Approximately 75ŌĆō90% occur in the midline,
mostly arising in the inferior vermis
- Hemispheric locations account for 10ŌĆō15% of the cases and are associated with an older age and desmoplastic histology
- Most commonly involve defect in chromosome 17
- Can be seen with GorlinŌĆÖs syndrome and TurcotŌĆÖs syndrome

Fig. 15

Fig. 12

Fig. 14

Fig. 13
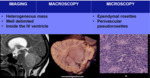
EPENDYMOMA
- Ependymomas are the fourth most common posterior fossa tumors in children and constitute approximately 8ŌĆō15% of the neoplasms
- Mean age at diagnosis is 4ŌĆÉ6 years,
1/3 of which are diagnosed before age 3
- Arise from the ependymal cells that line the ventricle of the brain and spinal cord,
most commonly located infratentorial
- Deletion of chromosome 22q
- NF2 patients commonly have spinal ependymomas not intracranial
- Can be seen with LiŌĆÉFraumeni syndrome (p53) and Turcot syndrome (APC gene)
- Location: floor of the 4th ventricle (60%),
lateral aspect of the 4th ventricle (30%) and roof of the 4th ventricle (10%)
- Typically,
a long history characterizes the clinical findings,
including signs of increased cerebral pressure,
ataxia,
and lower cranial nerve palsies

Fig. 7

Fig. 6
BRAINSTEM GLIOMA
- Gliomas of the posterior fossa/brainstem account for 5ŌĆō11% of all intracranial tumors in children and for 15ŌĆō30% of infratentorial tumors
- Peak presentation at 7ŌĆÉ9 years

Fig. 9

Fig. 8
- Clinical findings (classic triad seen in 1/3 of cases):
ŌĆō Cranial nerve palsies
ŌĆō Ataxia
ŌĆō Long tract signs
- Diffuse intrinsic brainstem Glioma:
Most commonly located in the Pons
Account for 80% of brainstem tumors
They typically involve more than 50ŌĆō75% of the cross sectional area of the brainstem on initial diagnosis and are generally poorly defined
- Focal Tumors:
Occupy less than 50% of brainstem subregion
Often clearly distinguishable from surrounding brainstem
Midbrain tumors carry the best prognosis
Dorsal exophytic tumors ~20% of brainstem tumors and typically fills the 4th ventricle
SCHWANNOMA
- Can be unilateral or bilateral
ŌĆō If there are bilateral acoustic schwannomas this is diagnostic for NF2
ŌĆō Unilateral acoustic schwannoma and a first degree relative with NF2 is
diagnostic of NF2
- Can be sporadic or associated with NF2,
sporadic variety is very rare in pediatric population
- NF2 associated schwannomas present with auditory complaints only 30% of the time,
grow faster and have increased invasion of the nerve
- It represents 60-90% of all CPA tumors,
sensorineural hearing loss is the most common presentation,
frequently accompanied by tinnitus and dysequilibrium

Fig. 22

Fig. 21
MENINGIOMA
- Meningiomas can occur at any age,
but are rare in children representing only 0.4ŌĆō4% of all pediatric brain tumors
- Pediatric meningiomas are usually seen as part of a NF2 syndrome,
or may occur as complication of prior radiation therapy
- NF2 can be found in approximately 40% of all children presenting with meningiomas and should be considered in any child with a meningioma
- They typically present with nonspecific symptoms,
depending on their location and compression of adjacent neuronal structures

Fig. 17

Fig. 16
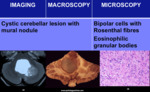
HEMANGIOBLASTOMA
- Most common primary intra-axial tumor of the posterior fossa in adults (WHO grade 1)
- Location: posterior fossa (90-95%): cerebellar hemispheres (80%),
vermis (15%)
- Capillary hemangioblastoma is the most frequent manifestation of Von Hippel-Lindau (VHL) syndrome
- There tumors can be solid tumor (25-30%),
cystic with a mural nodule on one of the walls (55-65%),
mixed (4%) or cystic (6%)

Fig. 11

Fig. 10
METASTASES
- Metastasis is the most common intra-axial neoplasm of posterior fossa in adults
- About 20 % of all intracranial metastases occur in the posterior fossa and the most common primary sites are lung,
breast,
malignant melanoma,
gastrointestinal and genitourinary tumors
- In children,
intracranial metastases from systemic malignancies most commonly result from neuroblastoma,
Ewings's sarcoma,
osteogenic sarcoma,
rhabdomyosarcoma,
and Wilm's tumor
- Multiple lesions are the hallmark,
however in the posterior fossa there is a high incidence of solitary lesions (25-50%)
- Typically,
metastases enhance strongly and are surrounded by significant amounts of vasogenic edema

Fig. 20
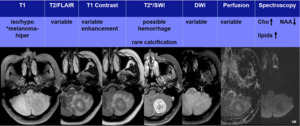
Fig. 18

Fig. 19