Radiologic features
The patterns of COP can be divided into two main groups: typical and atypical [23].
The main HRCT findings in OP include: consolidation,
ground-glass opacification,
peri-lobular opacity,
reversed halo opacity,
nodule or mass,
parenchymal bands,
bronchial wall thickening,
bronchial dilatation,
mediastinal lymphadenopathy and pleural effusion [24].
Typical COP consist of multiple alveolar opacities; atypical pattern includes: nodular pattern (solitary or multiple nodules or masses),
infiltrative opacities (infiltrative COP),
atoll sign,
broncho-centric lesions,
linear and band-like opacities,
crazy paving pattern and progressive fibrosis [14,21,23,25].
(Table 1)
Typical pattern
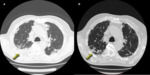
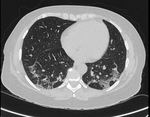
Classical form of COP is characterized by multifocal parenchymal consolidation,
often bilateral and asymmetrical.
These findings are usually described as patchy or with periferical/ peribronchial predominance in lower lobes.
They tends to migrate,
disappearing spontaneously and appearing in different sites.
(Fig.1)
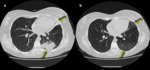
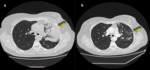
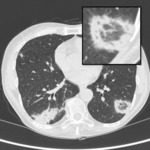
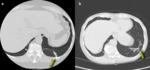
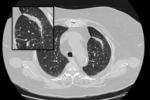
These consolidations may be associated with ground-glass opacities; usually,
these lesions may reproduce an air bronchogram sign in the context [25].
(Fig.
2,3)
On onset,
this pattern can be encountered in 75% of patients.
Multifocal parenchymal consolidations may be a sign of other pathological conditions that must be considered: bronchioloalveolar carcinoma,
primary pulmonary lymphoma,
eosinophilic pneumonia,
multifocal pneumonia,
alveolar hemorrhage,
multiple pulmonary infarcts,
alveolar sarcoidosis,
or ANCA-associated vasculitis [23].
If they have a fluctuating presentation,
the differential diagnosis can be reduced to four etiologies: OP,
eosinophilic pneumonia,
alveolar haemorrhage and vasculitis [21].
Atypical pattern
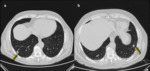
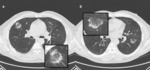
Nodular form.
Nodules can be solid,
part-solid or ground glass,
with no specific distribution (sprinkled or peribronchovascular).
(Fig.4)
Nodules could have speculated borders,
so the first suspect is for a malignant nature of the lesion.
If excavated (rare but possible),
the nodule can mime tuberculosis or septic embolism [23].
Atoll sign
Atoll sign (or reverse halo sign) was for a long time considered to be pathognomonic of OP; actually there are other conditions associated with this radiological feature which must be excluded (vasculitis,
sarcoidosis,
paracoccidiodomycosi,
pneumocystosi,
tbc,
lipoid pneumonia and complication of radio frequency treatments).
It is an area of ground glass opacity surrounded by a ring or a crescent-shaped consolidation [23,26].
(Fig.5,6)
Crazy paving pattern
Crazy paving pattern is represented by areas of ground glass opacities adjacent to focal area of consolidation and septal thickening.
It’s an uncommon presentation of COP [27,28].
Crazy paving pattern is a sign of different lung pathologies such as infection,
IIPs,
ARDS and sarcoidosis [29].
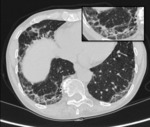
Progressive fibrosis pattern
Op can produce sub-pleural reticulations and architectural distortion in about a 15% of cases,
miming the appearance of NSIP; this presentation seems to be associated to a poor outcome [23].
(Fig.7)
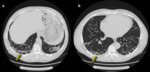
Infiltrative pattern
Infiltrative COP may be associated with interstitial alterations and superimposed small alveolar opacities and in some cases overlaps with IPF and NSIP.
The infiltrative pattern is characterized by curved or arcade-like bands of parenchymal consolidation with blurred borders and thickening of the interlobular septa with reticular pattern [25]; it’s a perilobular pattern and often associated with other opacities,
especially consolidations [16,23].
(Fig.8,9)
The presence of air bronchogram sign helps to differentiate this pattern from atelectasis and fibrotic bands; other conditions that must be excluded are postprimary tuberculosis,
lymphomatoid granulomatosis,
lymphangitis carcinomatosis,
Fungal infections,
Sarcoidosis,
pulmonary infarction and interstitial edema [30].
Linear and band-like opacities
They are thick radial bands of consolidation containing an air bronchogram (dd with atelectasis) or sub-pleural curvilinear bands parallel to the pleura.
These signs are very evocative of OP [23].
Frequently implicated diseases associated with linear abnormalities are pulmonary edema,
lymphangitic carcinomatosis,
atelectasis and asbestosis [30].
(Fig.10,11)
Extra-lung radiological findings
Mediastinal lymphadenopathy
Mediastinal nodes with a short-axis diameters >1 cm are observed in 20-30% of patients.
The most frequently involved mediastinal node stations are pulmonary hilum (s10),
lower paratrachea (s4) and subcarina (s7) [31].
Pleural effusion
Small amounts of pleural effusion are seen in 10-35% of patients,
usually bilateral [31].