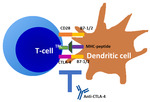
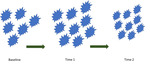
Mechanism of action of ICIs
Genetic alterations in cancer antigens can create new antigens,
recognized by the host immune system as “non-self”.
The antitumor response involves a complex interaction between immune cells,
tumor cells and the environment. However,
cancer cells can escape immune recognition and destruction in a variety of ways.
(3)
ICIs are monoclonal antibodies that promote immune system mediated tumor destruction by inhibiting the signaling pathways that suppress anti-tumor T-cell activity,
targeting molecules on the surface of T-cells.
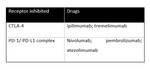
(2) ICIs that are currently in use target receptors as CTLA-4 (cytotoxic lymphocytes associated antigen 4) and the axis of PD-1 (programed death-1) receptor and its ligands,
namely PD-L1.
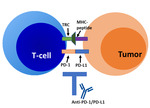
(3) Fig. 1 Fig. 2
Immune checkpoint blockade can lead to induction of hyperactivated T-cell-mediated response against normal tissue,
breaking tolerance to "self." (3)
Tumor response patterns with ICIs
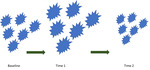
ICIs can generate a tumor response patterns not found with conventional chemotherapy,
namely pseudoprogression (initial increase in tumor burden preceding tumor regression).
(3) Fig. 3 Fig. 4
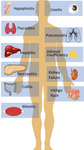
Immune-related adverse events
ICIs can cause a unique spectrum of toxicities,
which are known as immune-related adverse events (IrAE),
which can occur early,
even after the first treatment.
(3,
2) Fig. 5
Although IrAE can involve any organ system,
clinical experience has revealed a clear role for imaging in the evaluation of a few adverse events.
In addition to making a diagnosis,
radiologist plays a role in the management of IrAE by monitoring change on serial images.
(1)
Anti-CTLA-4 and anti-PD-1/PD-L1 drugs,
although similar,
have different IrAE incidences (anti-CLA-4 54% and anti-PD-1/PD-L1 14-26%).
(1)
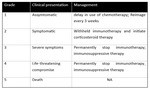
IrAE can be managed with strategies including delaying a scheduled dose,
administering corticosteroids and discontinuing therapy,
depending on severity.
Early diagnosis and close follow-up can contribute to a safe management of the patients.
(2) Table 2 Fig. 6
It is not known which patients are more susceptible to IrAE,
however a positive correlation between development of side effects and a favorable response to treatment exists.
(2)
Our work will focus on the most common IrAE with thoracic,
abdominal and pelvic manifestations. Table 3
1) Pneumonitis
More common with PD-1/PD-L1 inhibitors than anti-CTLA-4.
According to literature,
the median time of onset range from 9 days to 19months and the incidence varies between 3-6%.
(3,
4,
5)
Importantly,
pneumonitis can recur after appropriate treatment.
(3) It is a life-threatening condition that requires attention.
(6)
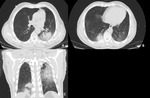
Image findings:
It is advisable to perform thoracic imaging at baseline and every 6-9weeks after treatment is started.
(3)
CT findings include ground glass opacities,
consolidations,
reticular opacities,
consolidations and traction bronchiectasis.
Decrease lung volume and small pleural effusions might be seen.
(5) Fig. 7
Four CT patterns have been reported: (3,
5,
6)
· Cryptogenic organizing pneumonia (65%)
· Non-specific interstitial pneumonia (15%)
· Hypersensivity pneumonitis (10%)
· Acute interstitial pneumonia/acute respiratory distress syndrome (10%)
Differential diagnosis:
Include edema,
infections,
hemorrhage or progression of the disease.
Immune mediated pneumonitis is a diagnosis of exclusion,
therefore other disease processes need to be ruled out.
(3) New ground glass opacities in a patient with lung cancer treated with PD-1/PD-L1 inhibitor should prompt radiologist to consider immune mediated pneumonitis.
(3)
2) Colitis
It is an important complication,
and the most commonly reported.
(4) In fact,
the highest mortality associated with IrAE occurred as a result of severe colitis,
with worst outcomes resulting from prolonged time between appropriated diagnosis and treatment.
(2) It is more common with CTLA-4 inhibitors (8-38% with ipilimumab) and typically occurs 6-7 weeks after therapy initiation.
(1,
6)
Image findings:
Three patterns have been described: (1,
5,
6)
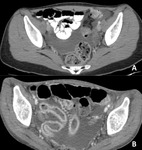
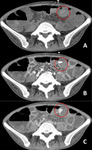
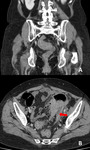
· Diffuse colitis (most common) Fig. 8 Fig. 9
· Segmental colitis (superimposed to diverticulitis) Fig. 10
· Isolated rectosigmoidal colitis
Characteristic CT findings are non-specific and include: mesenteric hyperemia (comb sing),
bowel wall thickening,
increased mucosal enhancement,
a fluid filled small or large bowel and fat stranding and free fluid.
Rarely colitis can lead to perforation (1,
6,
8)
Differential diagnosis:
Infectious and inflammatory conditions (e.g.
diverticulitis,
ischemic colitis)
3) Auto-immune hepatitis
It is rare (fewer than 5% of IrAE with ipilimumab).
(4,
8) The median time of onset is 3-9 weeks with ipilimumab.
(2)
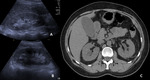
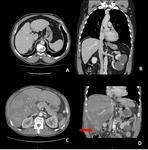
Imaging findings:
Include hepatomegaly,
periportal/gallbladder edema,
lymphadenopathy or hypoattenuation of the liver parenchyma at CT compared with baseline.
These imaging findings are not specific for auto-immune hepatitis,
but in the setting of cancer immunotherapy this diagnosis should be recognized as a possibility.
(2,
6,
7) Fig. 11
Differential diagnosis:
Other inflammatory and infectious conditions (e.g.
acute viral hepatitis).
(2)
4) Endocrinopathies
Median time of onset varies between 7-20 weeks with ipilimumab.
(2)
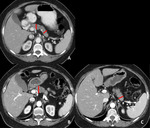
a)Pancreatitis
Immune mediated pancreatitis is rare,
with an incidence below 1%.
(6)
Imaging findings include organomegaly,
reduced density of the pancreas and increased density of peripancreatic fat or fluid.
In more severe cases necrosis and abscess formation may occur. Fig. 12
b)Thyroiditis
Immunotherapy-induced thyroiditis is rare and can occur in the first 5 months up to 3 years.
(4) Thyroid disfunction is predominantly a clinical diagnosis,
but radiologists may sometimes identify incidental abnormalities within the thyroid gland,
as ultrasound abnormalities (heterogeneous,
hypoechoic echotextures,
enlarged thyroid),
heterogeneous enhancement or increased FDG uptake on PET-CT.
(4,
7)
5) Other reactions
a)Sarcoid-like reaction
It is a rare side effect: there are few reported cases.
Involvement of lungs,
skin,
CNS and kidneys has been described.
(4) At imaging it manifests as new bilateral symmetric mediastinal and hilar lymphadenopathies,
multiple micronodules or ground glass opacities or enlarged spleen.
Needs to be differentiated from progressive disease and malignant lymphadenopathies.
(6,
7) It might regress spontaneously without treatment.
(7)