Keywords:
Head and neck, Ear / Nose / Throat, CT, MR, PET, Staging, Audit and standards, Technical aspects, Cancer, Education and training, Metastases
Authors:
A. Foran1, H. Barrett1, S. Looby2; 1Dublin/IE, 2Dublin /IE
DOI:
10.26044/ecr2019/C-3806
Results
We performed a review of this latest edition with the view of highlighting the pertinent changes whilst providing examples from our own practice.
The changes include:
- Depth of invasion (DOI)
- Oropharynx being divided into 3 separate chapters; nasopharynx,
HPV positive oropharyngeal squamous cell carcinoma (SCC),
hypopharynx and HPV negative oropharyngeal SCC.
- Extranodal extension
- Neck nodal SCC metastatsis with unknown primary
- Including DOI in the staging of OPSCC will better discriminate the higher risk small cancers as demonstrated by deeply invasive tumours from those with less invasive cancers that have an excellent prognosis.
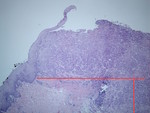
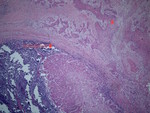
To measure DOI establish the horizon that is at the level of the basement membrane relative to the closest intact squamous mucosa.
The greatest invasion is measured by dropping a "plumb line" from the horizon.
This change is purely a pathological diagnosis (Fig 1) rather than a radiological measurement.
- A major change brought about in this 8th edition is the divison of the pharynx chapter into 3 separate chapter to reflect the very different biological and etiological difference between nasopharyngeal carcinoma,
HPV +ve oropharyngeal cancer,
and HPV -ve associated oropharyngeal cancer and hypopharyngeal cancer.
These divisions better reflect the variety of diseases arising in the pharynx.
As outlined above in the the new AJCC guidelines HPV+ orophayrngeal SCC will be staged separately.
This change reflects the markedly better prognosis of these tumours compared to HPV negative tumours.
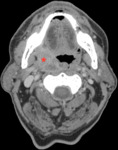
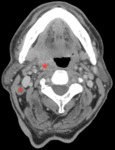
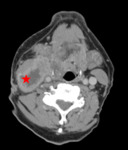
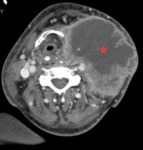
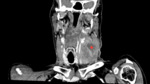
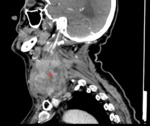
Fig 2 and Fig 3 demonstrate HPV positive oropharyngeal SCC.
There are no pathognomonic radiological features to distinguish HPV positive from HPV negative SCC.
But radiological features that help to distinguish HPV positive tumours include their small size,
well defined borders,
lack of invasion of surrounding structures,
a cystic appearance to lymph node metastases and also increased frequency of distant metastates to atypical sites.
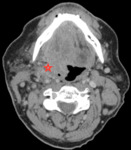
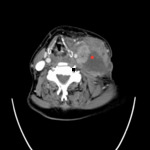
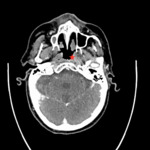
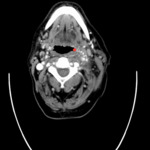
In contrast features that are more likely to predict HPV negative tumours (Fig.
4 and Fig.
5) are large size,
ill defined borders which invade surrounding structures and necrotic appearing lymph node metastases.
- Extranodal extension (ENE) (Fig 6) was another change in the updated edition,
being added as a prognostic variable for regional lymph node metastases.
Ultimately it is a pathological finding,
and the most significant pathological finding for prognosis in a positive lymph node.
As part of the updated guidelines it will now be an important aspect of staging non-HPV +,
non-EBV + cancers of the head and neck. Radiological findings that are supportive of a diagnosis of ENE include increased size,
necrosis,
ill-defined borders and invasion of adjacent structures.
But ultimately it remains a pathological diagnosis (Fig 7).
- Another change included the addition of SCC metastasis with unknown primary,
T0 is only valid for head and neck squamous cancer sites in the cases in which the patient is HPV positive (T0 oropharynx) or EBV positive (T0 nasopharynx).
It is usually the case that such primaries are located in the the fossa of Rossenmuller (Fig 11) or the oropalatine tonsils (Fig 12) for nasopharyngeal and oropharyngeal primaries respectively but these can often be radiologically occult.