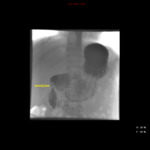
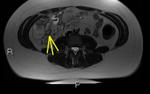
Paediatric Small Bowel MRI: An approach
There is more than one way to perform small bowel MRI.
Even with different scanners from the same manufacturer, sequences that are apparently identical produce images that look different. This poster describes experience with Seimens scanners across 3 Scottish health boards. All are 1.5T magnets. The majority of studies described were performed at the Royal Hospital for Sick Children in Edinburgh using a 1.5T wide bore scanner system (Seimens Espree).
When thinking about your protocol consider:
- Time: Time is money in a scanner. The less sequences the more efficient
- Patient demographics: Children will grant a limited time for scanning. Be quick and specific.
- Patient acceptability: Large volumes of oral distending agents are difficult to swallow if you have a diseased gut (or not)
- Reporting time: More sequences means longer reporting time. Only do the sequences that help you make the diagnosis accurately
Our basic small bowel MRI protocol would include:
- Coronal and axial T2 (we use HASTE sequences): for morphology
- Coronal and axial diffusion weighted images(DWI) (b0, 800 and 1300): for inflammation
- We do not administer IV contrast or spasmolytics
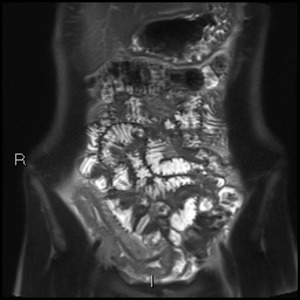
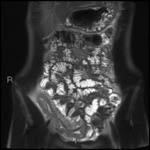
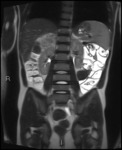
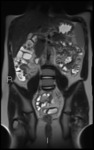
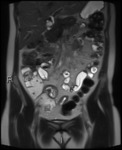
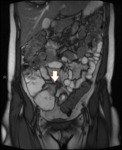
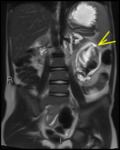
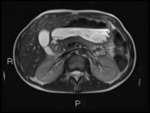
Fig. 1: Coronal T2 HASTE showing thickened, T2 hyperintense ileum with deep ulceration and surrounding mesenteric oedema
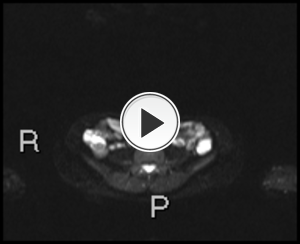
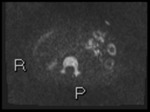
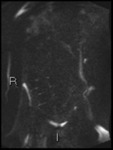
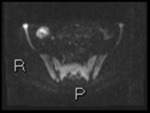
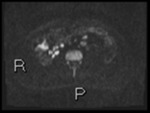
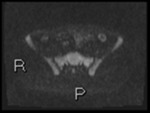
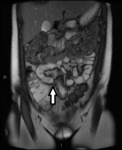
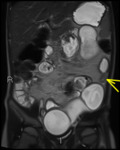
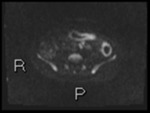
Fig. 2: Axial diffusion weighted Imaging (DWI) b0, 800 and 1300
Intraluminal fluid signal is suppressed at higher b-values.
Disease becomes conspicuous at b 800 and 1300
Nodes in the right iliac fossa show high signal and are easy to confuse with terminal ileal disease
References: Borders General Hospital, Melrose, UK
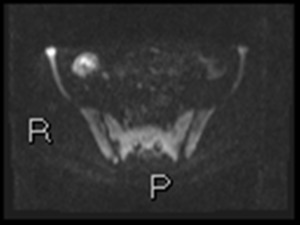
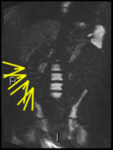
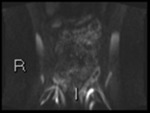
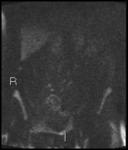
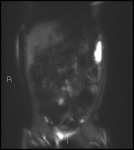
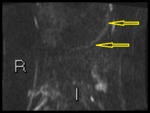
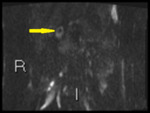
Fig. 3: b1300 DWI shows high signal in terminal ileum
Absolute ADC measurement of bowel is not very reproducible.
We use subjective comparative intensity ("how bright does it look") to decide if inflammation is present
Additonal sequences that are often used include:
- True FISP: uses chemical shift artefact for wall conspicuity
- T2 fat saturated images: Used for wall oedema. Superceded by DWI in our practice
- Cine images: useful for finding strictures. Some evidence that they assess overall motility which is a good indicator of disease response. We use a cine True FISP
- Post contrast imaging: We no longer use this as diffusion weighted imaging is as sensitive and specific.
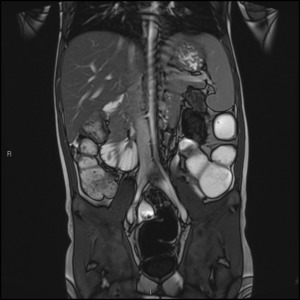
Fig. 5: Coronal True FISP image showing chemical shift artefact
References: Victoria Hospital, Kirkcaldy, UK
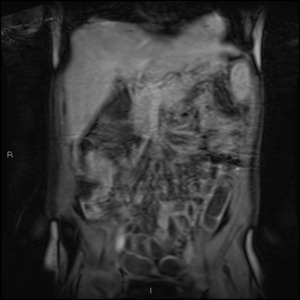
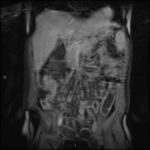
Fig. 6: Coronal T1 FS VIBE post contrast.
Both normal and abnormal bowel enhance.
Differentiating between normal and abnormal can be difficult
How long does a study take?
In our hospitals as standard small bowel MRI would take less than 25 minutes.
Oral distending agent (Lactulose) is taken 1 hour prior to scanning.
No buscopan or gadolinium is administered.
The same protocols are now used for adult as well as paediatric patients routinely.
Oral distending agents:
Following Giles et al (9) we use of 50ml of lactulose, diluted to 100ml with water and made more palatable by mixing with lemon flavouring as our distending agent. Prior to this we had used up to 2L of oral distending agents.
Massive distension is not a pre-reqisite for a diagnostic small bowel MRI and can be counter productive because of associated nausea. Enough distension to separate walls of small bowel is adequate.
Common MRI findings in paediatric IBD
Mucosal inflammation:
Classically IDB is a transmural inflammatory process. While this becomes true, it is not uncommon for paediatric patients to demonstrate mucosal disease only at presentation
If the radiologist relies on morphological imaging (HASTE/ True FISP) much mucosal disease may be missed
If you use DWI as part of your protocol you will recognise more mucosal disease
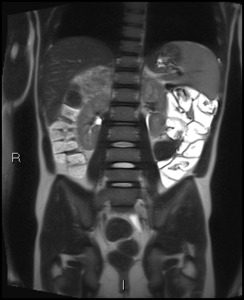
Fig. 7: Coronal T2 HASTE image.
Patient presenting with rectal bleeding.
Adequate distension of small bowel with oral distending agent in large bowel.
No abnormality seen
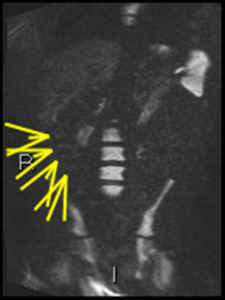
Fig. 8: b1300 coronal DWI shows colonic haustral high signal. This was initially reported by the corresponding author although the significance was not clear. Endoscopist confirmed apthous ulceration corresponding to areas of MRI abnormality
References: Borders general hospital, Melrose, UK
Another example of colonic haustral diffusion abnormality (b1300)
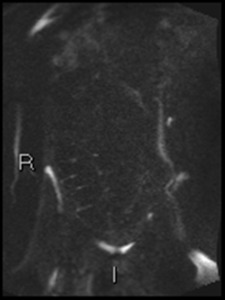
Fig. 9: Coronal DWI b1300 showing haustral diffusion abnormality.
Endoscopy shows apthous ulceration.
Ulceration
Ulceration can be difficult to see on MRI because of the limited spatial resolution. As shown above fine ulceration can be seen with diffusion weighted imaging. Deep ulceration can sometimes be seen in thickened bowel.

Fig. 1: Coronal T2 HASTE showing thickened, T2 hyperintense ileum with deep ulceration and surrounding mesenteric oedema
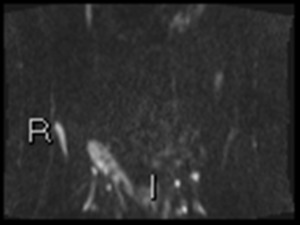
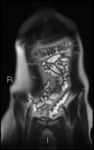
Fig. 11: Coronal DWI shows extensive ileal high signal.
The short bore of the MRI scanner used results in wrap at the pelvis explaining distortion of images
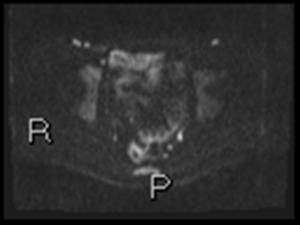
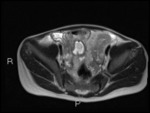
Fig. 10: Axial DWI b1300 shows rectal inflammation, ileal inflammation and mesorectal lymph nodes
Often, rectal mucosal disease is only seen on axial DWI.
Transmural Disease and fistulas
Transmural inflammation is a hallmark of IBD and while some paediatric patients present with mucosal only disease, transmural disease is more common
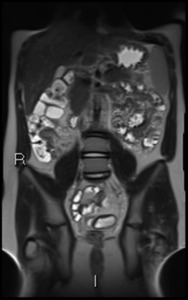
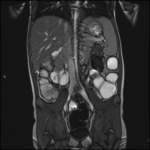
Fig. 12: Coronal HASTE shows thickened terminal ileum
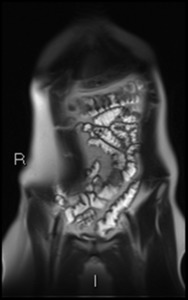
Fig. 13: Coronal HASTE shows extensive large bowel wall thickening
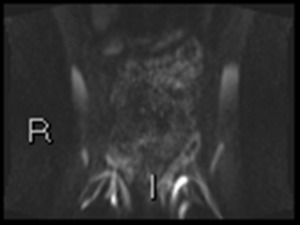
Fig. 14: b1300 DWI confirms inflammation in ileum and left colon
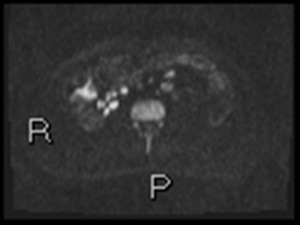
Fig. 15: Axial DWI b1300 shows ileal inflammation.
Nodal high signal is noted. Unlike inflamed bowel looks these are solid rather than circles of peripheral high signal with central low signal.
l
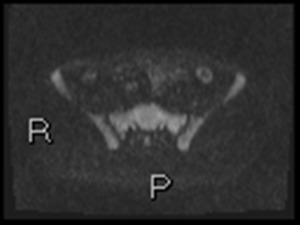
Fig. 16: Axial b1300 DWI shows circle of hyperintensity in left iliac fossa. This is inflamed left colon
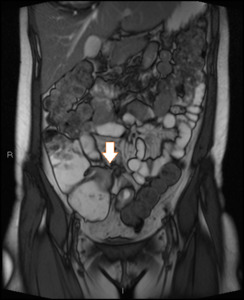
Fig. 20: Coronal True FISP image shows abnormal configuration of terminal and distal ileal loops.
Abnormal connection between bowel wall typical of entero-enteral fistula
No fluid in fistula track
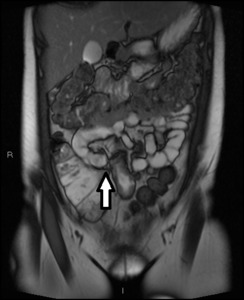
Fig. 21: Coronal True FISP image shows abnormal configuration of terminal and distal ileal loops
Abnormal connection between bowel wall typical of entero-enteral fistula (arrowhead)
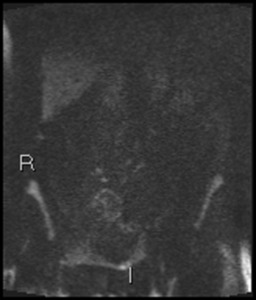
Fig. 22: Coronal b1300 DWI images show minor diffusion abnormality at site of fistula
Stricturing
Inflammatory stricturing can present early in paediatric IBD. This often settles with medical treatment.
Chronic, fibrotic stricturing is less commonly seen in paediatric patients suggesting there is a significant lag time in development of chronic stricutes.
The case below illustrates both types of stricturing with presumed fibrotic stricturing developing within 6 months of commencement of therapy.
9 years of age with a 1 year history of abdominal pain adn iron deficiency anaemia.
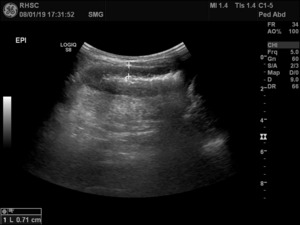
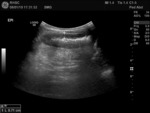
Fig. 23: Thickened left flank bowel loop with surrounding echogenic fat.
Initially this was interpreted as thickened colon
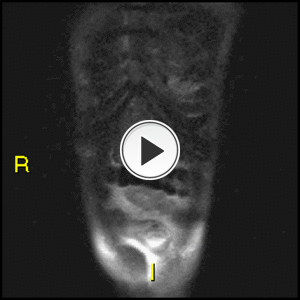
Fig. 24: Coronal HASTE. Multiple inflammatory strictures
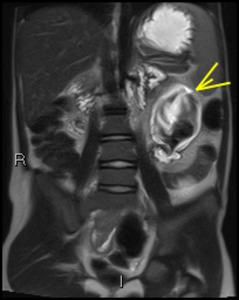
Fig. 25: Dilated jejunal loop
Low signal seen in the distended bowel loop is caused by turbulent flow associated with stricturing
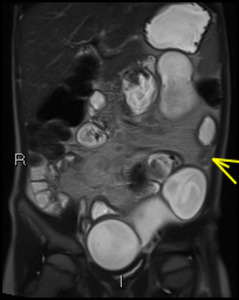
Fig. 26: Arrowhead denotes a fleshy stricutre with multiple dilated bowel loops giving a "Chain of lakes" appearance in this child with multiple strictures
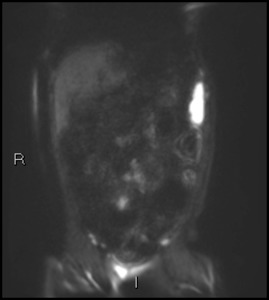
Fig. 27: Coronal DWI b1300 shows multiple areas of high signal consistent with inflammation and inflammatory strictures
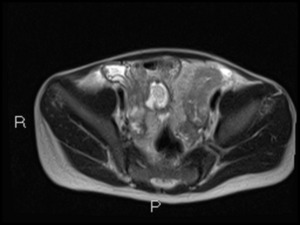
Fig. 28: Axial HASTE images showing bowel wall thickening and oedema in distal jejunum
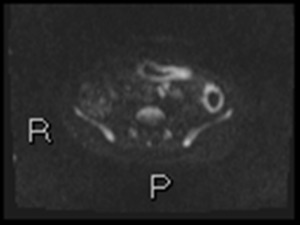
Fig. 29: b1300 axial DWI correlates the wall inflammation
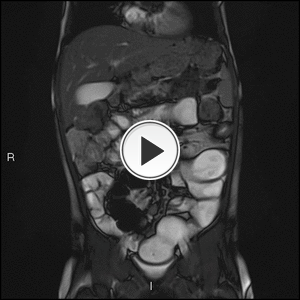
Fig. 30: Coronal cine True FISP images after 3 months of treatment.
Persisting stricutres. Best seen on these images in left upper and left lower quadrant.
These images give good appreciation of distension and motility
References: Victoria hospital, Kirkcaldy, UK
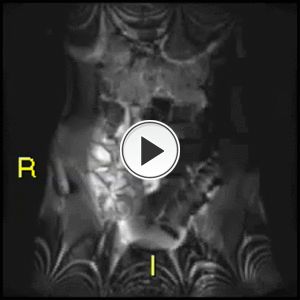
Fig. 31: Normal cine True FISP for comparison
Pathologically, strictures are often both inflammatory and fibrotic. Inflammatory strictures change with treatment to shorter, more fibrotic strictures with less wall thickening and diffusion high signal.
The disease in this child is jejunal and ileal with jejunal predominating early on.
Good jejunal distention can be hard to achieve. Our experience is that this does not matter. 4% of cases have jejunal disease (it is uncommon) and when it is present the jejunal disease is obvious manifest as wall thickening, dilatation, diffusion high signal and mesenteric oedema.
Gastric and duodenal disease
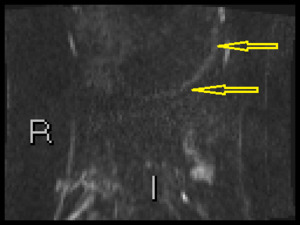
Fig. 32: b1300 DWI shows gastric inflammation in a 13 year old boy
Gastric disease is common in Crohn's and can be identified on SBMRI most commonly seen as diffusion high signal. Wall thickening is uncommonyl seen.
Why is gastric disease relevant as the patient may have had endoscopy? It is helpful as an internal control for diffusion signal elsewhere in bowel i.e. if histology and endoscopy show inflammation of the stomach and you see diffusion high signal in the stomach you know that the level of brightness you are seeing represents inflammation.
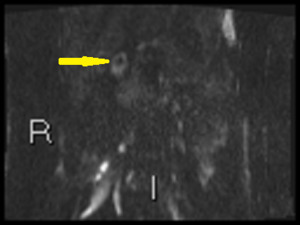
Fig. 33: The same 13 year old boy has high signal in proximal duodenum on b1300 coronal DWI
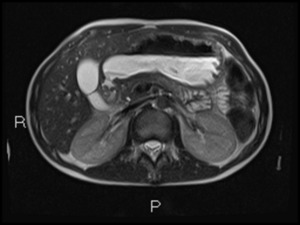
Fig. 34: Axial T2 HASTE shows duodenal dilatation
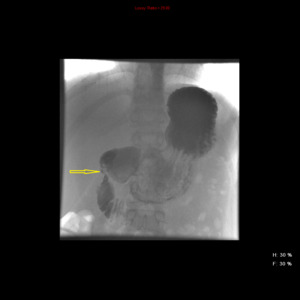
Fig. 35: Contrast meal confirms D1 stricture
Biopsy confirmed Crohn's. Patient initially improved with intensive medical therapy but relapsed within 6 months and was treated with laparoscopic gastroduodenostomy
Isolated gastroduodenal Crohn's is rare. This case is one of two published cases of stricturing duodenal Crohn's disease (the other is also from our institution) (11)
Mimics and pitfalls
Small bowel MRI can show inflammation but this is a not a pathological diagnosis. While many cases with inflammation represent IBD there are other potential causes. Worldwide, infection and infestation of the bowel with worms are common and potential pitfalls
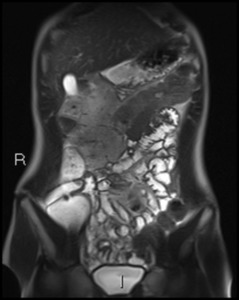
Fig. 36: Coronal T2 HASTE shows terminal ileal thickening
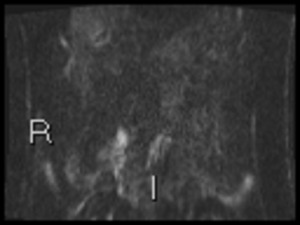
Fig. 37: Coronal DWI b1300 shows terminal ileal inflammation.
Endoscopy shows worms in the terminal ileum. No evidence of Crohn disease
Lymphoid intestinal hyperplasia is a recognised cause of wall thickening and inflammation in the distal small bowel (12)
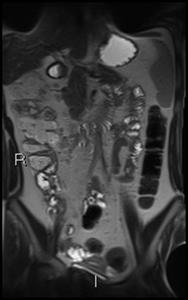
Fig. 38: Coronal T2 HASTE shows minor thickening of terminal ileum
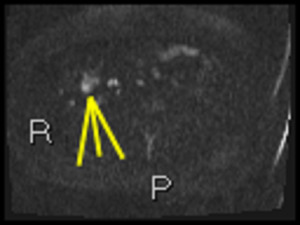
Fig. 39: Axial b1300 DWI shows linear high signal in TI with small adjacent nodes
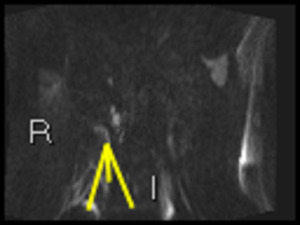
Fig. 40: Coronal b1300 DWI shows linear high signal in TI with small adjacent nodes
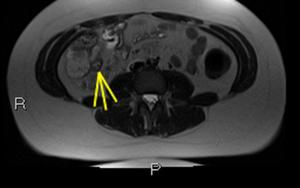
Fig. 41: Axial T2 HASTE images show terminal ileal wall thickening