Tuberculosis is caused by mycobacterial species in the Mycobacterium tuberculosis complex. It is transmitted via airborne droplet nuclei. A large number of patients infected with TB present with pulmonary complaints as the lungs are the most common site for the development of tuberculosis. Extra-pulmonary TB can occur either as a part of the pulmonary infection or as a late generalized manifestation of the spread of bacilli (Fig 1). Manifestations of tuberculosis can range from what looks like a simple infection to severe multisystem involvements with life threatening complications.
A) Pulmonary Tuberculosis
The lungs are the most common site of primary infection by TB and are a major source of spread of disease to other organs/ systems (2).
Pulmonary tuberculosis is classified as primary and post primary TB.
1. Primary TB: Primary TB is seen in patients who have not been prior sensitized to M tuberculosis. It is seen in the form of four main findings:
a) Parenchymal disease
- Areas of peripheral consolidation (Ghon's focus).
- Ghon's focus and enlarged/calcified lymph nodes (Ranke Complex).
- Apical calcified nodules (Simon foci).
b) Lymphadenopathy
- Ipsilateral hilar and contiguous mediastinal lymph nodes (Fig 10).
c) Miliary disease
- Occurs as a result of widespread hematogenous dissemination.
- Seen in the elderly, infants and in immunocompromised patients.
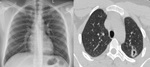
- Evenly distributed, small miliary (1–3 mm) nodules in bilateral lung fields (Fig 12).
d) Pleural effusion
- Usually unilateral and ipsilateral to site of infection (Fig 7 and Fig 8).
2. Post primary TB: Post primary TB follows primary TB after a latent interval and is either due to reinfection or reactivation of TB. As distinct from primary infection, in which healing is the rule, reactivation TB tends to progress (3). Following are the features of post primary TB:
a) Parenchymal disease:
- Cavities with thick, irregular walls (Fig 4)
- Parenchymal opacities
- Tuberculoma and satellite nodules
- Fibrosis and volume loss with healing
b) Airway involvement:
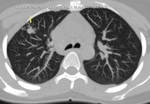
- Endobronchial spread - tree in bud sign (Fig 5 and Fig 6)
- Circumferential wall thickening and luminal narrowing of the airways
- Bronchiectasis
c) Pleural involvement
- Pleural thickening and calcification (Fig 7 and Fig 8)
- Tuberculous empyema
- Bronchopleural fistula
Some of the salient radiological features to differentiate active from inactive pulmonary tuberculosis are as follows (4):
Active Tuberculosis
|
Infiltrate/consolidation
|
|
Cavitary lesion
|
|
Nodule with poorly defined margins
|
|
Pleural effusion
|
|
Lymphadenopathy
|
|
Miliary TB
|
Inactive tuberculosis
|
Discrete fibrotic scar/ linear opacity
|
|
Discrete nodule without calcification
|
|
Fibrotic scar with volume loss or retraction
|
|
Discrete nodule with volume loss or retraction
|
|
Findings suggestive of prior TB
|
|
Cavities with intracavitary bodies
|
Complications of pulmonary tuberculosis:
- bronchiectasis
- mycetoma/ aspergilloma
- empyema thoracis
- fibrothorax (Fig 15)
- bronchopleural fistula
- arterial pseudoaneurysms: bronchial artery pseudoaneurysm, pulmonary artery pseudoaneurysm /Rasmussen aneurysm (Fig 13)
B) Extra pulmonary tuberculosis
1. CNS tuberculosis: Tuberculosis of CNS can result from either hematogenous spread from distant systemic infection or from direct extension from local infection. Manifestations include:
a) Extra-axial: The most common extra axial manifestation of CNS TB is tubercular meningitis (5), which is of two types:
i. Leptomeningitis (common)
- Thick basal exudates (Fig 16)
- Obstructive hydrocephalus
ii. Pachymeningitis (rare)
b) Intra-axial
- Intracranial tuberculomas: ring enhancing lesions with surrounding vasogenic edema (Fig 17)
- Focal tuberculous cerebritis
- Intracranial tuberculous abscess
- Tubercular rhombencephalitis
- Tuberculous encephalopathy
2. Head and neck TB
- Most common manifestation: bilateral painless cervical lymphadenopathy (Fig 11).
- Necrotic, conglomerated lymph nodes with/ without development of abscess or sinus tract formation.
3. Musculoskeletal TB
The major method of spread is hematogenous. TB spreads to vertebral body via Batson's venous plexus. It commonly manifests as:
a) Tuberculous spondylitis/ Pott’s spine
- Most frequent location for musculoskeletal TB.
- Lower thoracic and upper lumbar levels are the most common sites (Fig 18 and 19).
- Anterior wedging, reduction in vertebral height and intervertebral disc space (Fig 19).
- Paravertebral abscess (Pott's abscess) including psoas abscess (Fig 19 and 20).
- Gibbus formation.
b) TB osteomyelitis:
- Osteopenia and lytic lesions
- Sclerosis or periosteal reaction
- Sequestrum, involucrum and sinus tract formations
c) Tuberculous arthritis:
- Typically monoarthritis (Fig 22)
- Phemister’s triad (peri-articular osteoporosis, peripherally located osseous erosions, gradually decreasing joint space)
- Fibrous ankylosis
4. Abdominal TB: Abdominal TB is transmitted via swallowing of infected sputum, hematogenous spread from lungs, direct spread from infected adjacent foci or lymphatic spread from infected mesenteric lymph nodes. It manifests as:
a) GI tract involvement: The lesions are of three types: ulcerative, hypertrophic or stricturous (6). Ileocecal region is the most common site (Fig 23), manifested as bowel wall thickening with / without strictures, pulled up caecum and adjacent necrotic lymph nodes.
b) Abdominal lymphadenopathy:
- most common manifestation of abdominal tuberculosis.
- mesenteric, peripancreatic and periportal lymph node groups commonly involved with multiple necrotic lymph nodes with/ without calcification.
c) Tuberculous peritonitis:
- Wet type peritonitis: most common type, presenting as free or loculated ascites (Fig 25).
- Fibrotic type: omental and mesenteric masses, matting of bowel loops, omental caking (Fig 24).
- Dry type: fibrous adhesions and caseous nodules.
d) Solid organ involvement:
- Liver and spleen are the most commonly involved organs (7).
- Hepatosplenomegaly.
5. Genitourinary TB: Genitourinary TB always occurs secondary to hematogenous dissemination from lungs, bones or GIT. It manifests as the following (8):
a) Renal TB:
- Early: papillary necrosis.
- Progressive: multifocal thickening and enhancement (Fig 26, Fig 27).
- End stage: parenchymal thinning, dystrophic calcification.
b) TB ureter: wall thickening, strictures with beaded appearances, pipe stem ureter.
c) TB urinary bladder: irregular wall, decreased capacity, bladder calcification, thimble bladder.
d) Prostatic TB: enlargement of gland, hypoechoic areas, irregular contour.
e) TB of male genitalia: orchitis, epididymitis (Fig 30), wall thickening or irregularity of seminal vesicles/ vas differens.
f) TB of female genitalia: PID, infertility, tubo-ovarian abscesses, uterine synechiae, beaded fallopian tubes.
Complications of extrapulmonary tuberculosis
Extrapulmonary tuberculosis can lead to a number of complications depending upon the site of involvement. Common complications associated with extrapulmonary tuberculosis are abscess formation, sinus tracts/ fistula formation (Fig 29), non-healing chronic ulcers, intestinal and ureteric strictures, infertiity and PID. High index of suspicion with prompt and proper imaging evaluation of tuberculosis can help us prevent a number of these complications.