Keywords:
Performed at one institution, Diagnostic or prognostic study, Retrospective, Osteoporosis, Metabolic disorders, Demineralisation-Bone, Experimental investigations, Computer Applications-Detection, diagnosis, CAD, Digital radiography, Absorptiometry / Bone densitometry, Musculoskeletal bone, Computer applications, Artificial Intelligence, Information Technology
Authors:
A. Creeden; Coventry/UK
DOI:
10.26044/ecr2020/C-02138
Methods and materials
Full Research Ethics Committee approval was not required for this study. Local approvals were granted by the hospital Research and Development department under Governance Arrangements for Research Ethics Committees (GafREC) provisions (ref. GF0235).
A convenience sample of 150 individuals who had undergone both pelvic radiography and femoral neck DXA within a maximum interval of 6 months during 2016 was identified retrospectively. Patients were classified by DXA according to the World Health Organisation (WHO) definitions (figure 2). The sample was intentionally balanced to include equal proportions of individuals with each DXA classification, such that 50 were classified as osteoporotic, 50 as osteopenic and 50 as normal.
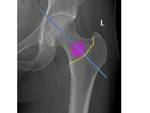
Textural analysis software (qMaZda, University of Lodz, Poland) was used to calculate 329 textural parameters relating to a 1cm2 region of interest (RoI) placed in the central axis of the femoral neck, such that the inferolateral corner of the RoI abuted the intertrochanteric line (figure 3). The textural results were collated into a Machine Learning (ML) training dataset. An independent test dataset comprising a further 150 individuals was created following an identical method using data from patients who underwent both radiography and DXA in 2017. The hospital site and equipment used were the same for both the training and test datasets. No individuals were included in both the training and test datasets.
Using the data in the training dataset, eight common ML algorithms available within the WEKA software application (University of Waikato, New Zealand) each generated a different model for the prediction of an individual’s femoral neck DXA classification (normal, osteopenic or osteoporotic) based solely on the individual's femoral neck textural parameters.
The accuracy of each model was evaluated on the training dataset using ten-fold cross-validation. The model which had the highest accuracy when tested using ten-fold cross-validation was then further assessed using the independent test dataset.

![Fig. 2: Definitions of normal, osteopenic and osteoporotic bone according to WHO criteria [6].](https://epos.myesr.org/posterimage/esr/ecr2020/152921/media/847418?maxheight=150&maxwidth=150)