Patients
Between April and July 2019, A total of 132 patients (88 males, 44 females) with an average age of 69 ± 10.5years (range, 34–85 years) who underwent both echocardiography and CT at the same day for evaluation of coronary artery were enrolled in the study(Table 1).
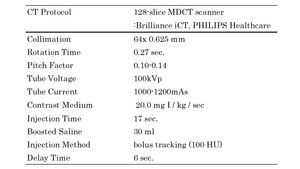
Table 1: The Table shows demographics of the study population.
CT protocol
Contrast-enhanced cardiac CT were performed with 128-slice MDCT scanner (Brilliance iCT, PHILIPS Healthcare).
The imaging parameters were as follows: collimation, 64 mm x 0.625 mm; Rotation time: 0.27 sec.; pitch factor,0.10 to 0.14; tube voltage,100kV; tube current, 1000 to 1200 mAs.
In the contrast injection method, scan was started after the CT value in the descending aorta reached 100 HU at the location of the trachea branch using the bolus tracking method. (delay time 6sec)
Contrast medium ,20.0 mg I / kg / sec; Injection time ,17 seconds; boosted with 30 ml of saline at the same speed as the injection rate (Table 2).
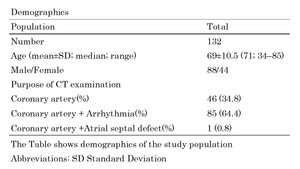
Table 2: The Table shows CT protocol.
The reconstruction parameters were as follows: reconstruction slice thickness,0.8 mm; reconstruction interval,0.8 mm; display FOV,160 to 180 mm; reconstruction function, XCB (cardiac standard function);reconstruction method,iDose4 (PHILIPS Healthcare); reconstruction steps,10% throughout the entire R–R interval; cine images, 0–90% ;phase-interpolated reconstruction, 30-phases using deformable voxel-to-voxel registration algorithm (PhyZiodynamics, Ziosoft Inc.,Tokyo,Japan) (Table3).
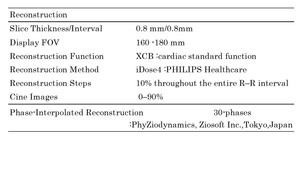
Table 3: The Table shows reconstruction parameters.
Image analysis and measurement
Both the tricuspid annular plane systolic excursion (TAPSE) and the right ventricular fractional area change (RVFAC) are used to estimate the right heart fraction.
Echocardiography
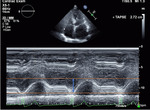
TAPSE is assessed in an apical four‐chamber view by placing the M‐mode on the lateral tricuspid annulus; maximum systolic excursion of the lateral annulus along its longitudinal plane toward the apex is recorded.[10-11]
The displacement of the basal segment from the reference point reflects longitudinal contraction of the RV.
This is the most commonly used parameter for RVF quantification (Fig.2).
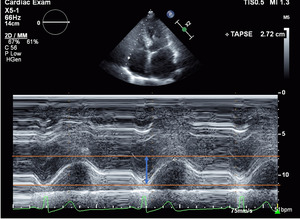
Fig. 2: How to measure TAPSE with echocardiography.
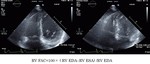
RVFAC is the percent change in RV area from diastole to systole.
It is performed by tracing the endocardial RV borders during diastole and systole.
A RV focused 4-chamber-view is essential to ensure that the entire endocardial border is visible in end-systole and end-diastole.
RVFAC was calculated by the following formula: RVFAC = [(end‐diastolic RV area – end‐systolic RV area)/end‐diastolic RV area] × 100.
RVFAC is best correlated with MRI‐derived RVEF(Fig.3).[12]
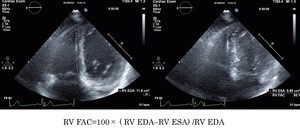
Fig. 3: How to measure RVFAC with echocardiography.
128-slice MDCT
Multiplanar reformats (MPR)was displayed in a four-chamber view from phase-interpolated reconstruction data.
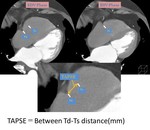
It was set to Td that the position of the tricuspid lateral annulus at the right ventricular end-diastolic.
And it was set to Ts that the position of the tricuspid lateral annulus at the right ventricular end-systolic.
Defined as TAPSE, the distance between Td and Ts on MPR was measured (Fig.4).
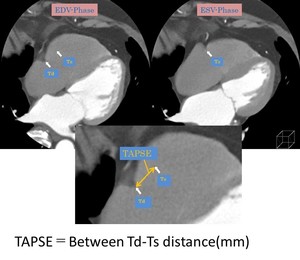
Fig. 4: How to measure TAPSE with CT.
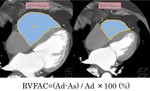
The right ventricular end-diastolic area (Ad) and end-systolic area (As) were measured on MPR in the four-chamber view.
Defined as RVFAC, it was calculated by the following formula: RVFAC=(Ad-As) / Ad x 100(Fig.5).
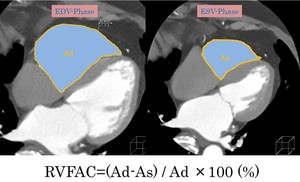
Fig. 5: How to measure RVFAC with CT.
Statistical analysis
TAPSE and RVFAC were measured on echocardiography by experienced sonographer.
TAPSE and RVFAC were measured on CT by independent five radiographers, and the median values were compared to echocardiography-derived values.
Pearson’s correlation coefficient(r) was calculated to determine whether there was a correlation between the TAPSE and FAC calculated by CT and echocardiography.
A paired t-test was used to evaluate the statistical significance of the differences in TAPSE and FAC as determined using CT and echocardiography.
A P-value of less than 0.01 was considered significant.
The agreement between CT and echocardiography was evaluated using Bland-Altman analysis.
A P-value of less than 0.01 was considered significant.
Besides, inter-observer correlation on CT was evaluated using intraclass correlation coefficients (ICC) and Cronbach's alpha (α).