Hiatal hernia
Hiatal hernia (HH) is characterized by protrusion of stomach or abdominal viscera, into the thoracic cavity through the esophageal hiatus [1]. It is mainly caused by weakening of the phrenoesophageal ligament and widening of the esophageal hiatus in case of increased intraabdominal pressure [2].
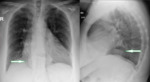
Often asymptomatic, HH are an incidental finding on chest radiograph, which reveals a retrocardiac mass containing air-fluid level (Fig.1) [2].
Current classification of HH comprises of four subtypes, based on the position of the gastroesophageal junction in relationship to the esophageal hiatus, exquisitely described on MDCT with MPR, as follows:
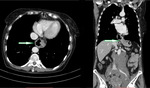
- Type I HH, or “sliding hernia”, is the most common type of HH (95%), being characterized by intrathoracic migration of the gastroesophageal junction, while the gastric fundus remains below the diaphragm (Fig.2).
Types II – IV HH are referred to as “paraesophageal hernias”, being differentiated from type I by laxity of the gastrosplenic and gastrocolic ligaments and intrathoracic migration of the stomach.
- The least common, type II HH results from herniation of the gastric fundus into the thorax through a localized defect in the phrenoesophageal membrane, while the gastroesophageal junction remains below the diaphragm.
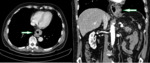
- Compound HH, or type III hernia, represents a combination of types I and II hernias, characterized by cephalic migration of both gastroesophageal junction and gastric fundus into the thoracic cavity (Fig. 3). It accounts for more than 90% of paraesophageal hernias and can be associated with gastric malrotation.
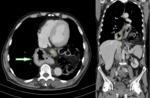
- Type IV HH is caused by a large defect of the phrenoesophageal ligament, leading to intrathoracic herniation of stomach and other abdominal viscera, such as the colon, small bowel or spleen (Fig. 4) [1,2].
Possible complications, which may appear in case of intrathoracic gastric herniation, include incarceration, strangulation and volvulus. Contrast-enhanced MDCT allows for fast diagnosis of gastric volvulus and possible complications, indentifying gastric wall thickening, pneumatosis, perigastric fluid collections and decreased gastric wall enhancement, in case of strangulation. Oral contrast is avoided in case of obstruction and when administered, water is preferred for optimal evaluation of the gastric wall enhancement [1,3].
- Gastric volvulus represents a rare condition, mostly associated with paraesophageal HH, characterized by intrathoracic or intraabdominal malrotation of the stomach. It can be classified as either organoaxial or mesenteroaxial, depending on the axis of rotation. The most common type is organoaxial volvulus, characterized by pathological rotation of the stomach along its longitudinal axis or cardiopyloric line. In mesenteroaxial volvulus, the rotation occurs along the mesenteric short axis of the stomach, the gastric antrum being displaced superiorly to the gastroesophageal junction. Predominantly in elderly population, gastric volvulus presents with symptomatology ranging from chronic asymptomatic (Fig. 4) to acute, with the classical triad of Borchardt (acute epigastric pain, unproductive retching, inability to pass the nasogastric tube) (Fig. 5). Complete gastric rotation >180°, seen more often in organoaxial volvulus, is considered predisposing to strangulation and obstruction, whereas mesenteroaxial volvulus is usually partial [1,3].
Differential diagnosis include epiphrenic or traction diverticulum and esophageal-respiratory fistula (Fig 6), which on chest radiograph may present as retrocardiac soft tissue mass with or without air-fluid level [1].
- Epiphrenic diverticulum is a pulsion diverticulum characterized by herniation of mucosa and submucosa through the muscular layers of the distal esophagus, almost invariably associated with an underlying esophageal motility disorder, such as achalasia [4]. It is best described using a barium esophagogram, while MDCT accurately describes location, dimensions and content of the esophageal pouch (Fig 6).
- Esophageal-respiratory fistula represents a communication between the esophagus and the respiratory system, secondary to esophageal malignancy, infections or corrosive ingestion. Left untreated, it complicates with lung abscess. MDCT using intravenous and oral contrast accurately describes esophageal morphology, the fistulous tract and the lung abscess (Fig 7) [5].
Bochdalek hernia
Bochdalek hernia is considered the most common congenital diaphragmatic hernia, caused by incomplete fusion of the pleuroperitoneal membranes, which leads to a defect in the postero-lateral part of the diaphragm. It usually occurs on the left side, due to the presence of liver, which protects from thoracic herniation on the right side. Most cases of Bochdalek hernia in adults are asymptomatic, being usually an incidental finding [6].
MDCT is able to visualize the postero-lateral disrupted diaphragmatic continuity and herniated content, often omental or retroperitoneal fat in Bochdalek hernia (Fig 8).
Diagnostic pitfalls may occur in case of breathing artifacts, which can mimic posterior diaphragmatic discontinuity and Bochdalek hernia (Fig 9).
Morgagni hernia
Relatively rare, Morgagni hernia is characterised by a small congenital defect in the anteromedial part of the diaphragm (sternocostal triangle) [1]. Right-sided diaphragm is predominantly affected since the left sternocostal triangle is protected by the pericardium. Morgagni hernias are not usually diagnosed until adulthood, when are incidentally discovered [7].
On chest radiograph, Morgagni hernia is characterized by soft tissue opacity in the cardiophrenic angle, with superimposed intestinal gas in case of bowel loops herniation. Differential diagnosis includes pericardial cyst, eventration, prominent fat pad or Chilaiditi sign [1].
MDCT allows the highest accuracy in visualizing the defect of the sternocostal triangle, frequently containing omentum and colon (Fig 10). Moreover, it is the best imaging modality to evaluate complications like closed loop obstruction, strangulation or ischemia, being able to differentiate Morgagni hernia from other pathologies.
- Pericardial cysts are congenital entities that form due to failure of fusion of one of the mesenchymal lacuna that form the pericardial sac, showing a thin-walled, fluid mass, that lacks contrast enhancement on CT (Fig 11). MRI accurately describes typical patterns of pericardial cysts, showing hyperintense signal on gradient-echo sequence and hypointense signal on T1-weighted images (Fig 12) [8].
- Diaphragmatic eventration is characterized by incomplete muscular development and fibro-elastic changes of part of the diaphragm, which is displaced into the thorax. Chest radiograph identifies a focal diaphragmatic elevation, while MDCT is able to precisely differentiate the focal narrowing of the diaphragm from a true muscular defect (Fig. 13) [9].
- Chilaiditi sign presents with asymptomatic interposition of the colon between the liver and the right hemidiaphragm, without disruption of the diaphragmatic continuity (Fig 14) [10].