EPIPLOIC APPENDAGITIS IMAGING FINDINGS:
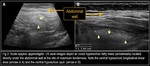
US Imaging Findings (Fig. 2):
Ovoid mass consisting of non-compressible hyperechoic fatty tissue located in the peritoneal cavity directly under the abdominal wall, at the site of maximum tenderness, adjacent to the colon, and with no central blood flow depicted on color Doppler US images.
The absence of a Doppler signal (lack of blood flow due to the torsion of an epiploic appendage) is a useful finding to differentiate epiploic appendagitis from acute diverticulitis.
Sagittal US scanning during inspiration and expiration shows that the mass is often fixed to the colon and often also to the parietal peritoneum.
A central hypoechoic spot (“central dot sign”) or a longitudinal linear area might be seen and it corresponds to engorged/thrombosed central vessels or central areas of hemorrhage/edema/fibrosis.
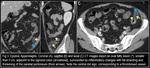
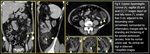
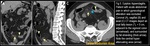
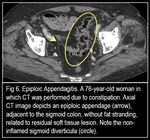
CT Imaging Findings (Fig. 3, Fig. 4, Fig. 5, Fig. 6, Fig. 7):
Oval lesion < 5 cm in diameter (typical diameter range 1.5–3.5 cm) that has attenuation equivalent to that of fat, abuts the anterior colonic wall and is surrounded by inflammatory changes. Thickening of the parietal peritoneum, secondary to the spread of inflammation, also may be observed (Fig. 3, Fig. 4).
The wall of the colon may be thickened but is most often normal in thickness. Intestinal obstruction and abscess formation are rare.
A central, hyperattenuating, ill-defined round area (“central dot sign”) or longitudinal linear area may also be seen (Fig. 3). Although the presence of a central dot or linear area is useful for diagnosis, their absence does not exclude the diagnosis of acute epiploic appendagitis (Fig. 4).
Although the clinical symptoms resolve within 2 weeks in most patients, the CT findings last longer.
At follow-up CT performed within 6 months of the initial manifestation of clinical symptoms, the findings on images may range from no change to decreased size of the lesion or lesions in the mesocolon, to residual soft-tissue attenuation (Fig. 6). 6 months after an episode of acute epiploic appendagitis, however, the CT features generally resolve.
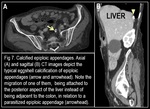
Calcification may be eggshell in shape and may become detached and appear as a peritoneal loose body in the abdominal cavity. The calcified tissue may reattach itself to a surface, such as the lower aspect of the spleen or liver, in which case it is called a “parasitized epiploic appendage” (Fig. 7). The smooth surface and calcified consistency of the epiploic appendage help to distinguish it from a metastatic lesion.
MR Imaging Findings:
T1WI and T2WI show a focal lesion with the signal intensity of fat.
Contrast-enhanced T1WI shows an enhancing rim around the oval fatty lesion.
The involved epiploic appendage is hyperintense on unenhanced T1WI but is slightly less intense than normal peritoneal fat. Epiploic appendages show a marked loss of signal on fat-suppressed T2WI, confirming the fatty nature of the lesion.
In epiploic appendagitis, the thin peripheral rim and the perilesional inflammatory changes appear hypointense on T1WI, hyperintense on T2WI, and show marked enhancement on contrast-enhanced fat-suppressed T1WI, whereas the central draining vein usually has low signal on both T1WI and T2WI.
MIMICS:
1) OMENTAL INFARCTION:
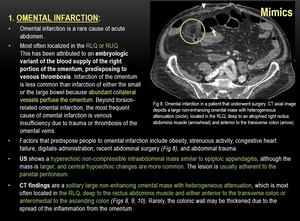
Fig. 8
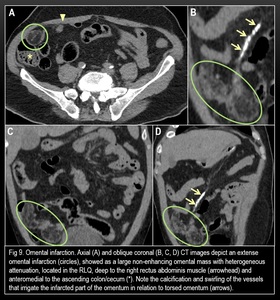
Fig. 9
Fig. 10
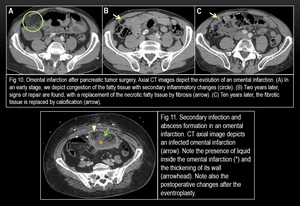
Fig. 11
2) SCLEROSING MESENTERITIS:

Fig. 12

Fig. 13
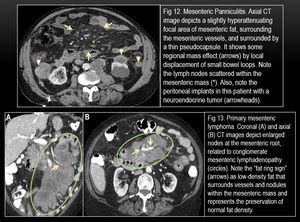
Fig. 14
3) NEOPLASMS:

Fig. 15
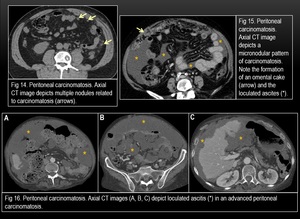
Fig. 16
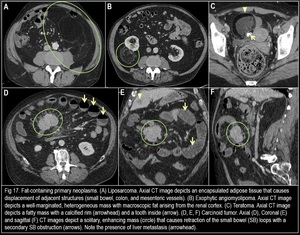
Fig. 17
4) TUBERCULOUS PERITONITIS:
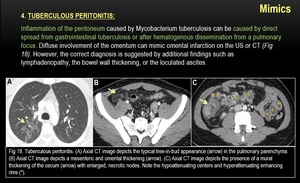
Fig. 18
5) TRAUMA:
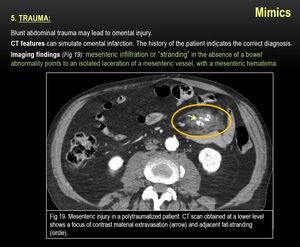
Fig. 19
6) URACHAL CYST:
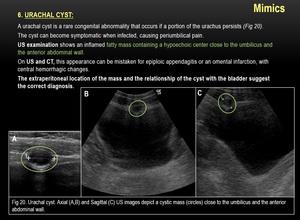
Fig. 20
7) ACUTE COLONIC DIVERTICULITIS:

Fig. 21
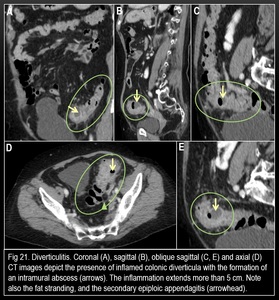
Fig. 22
8) ACUTE APPENDICITIS:
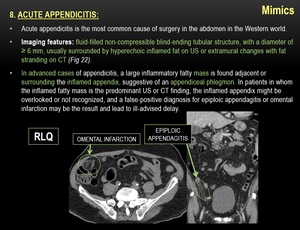
Fig. 23
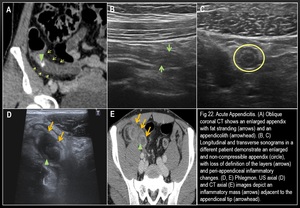
Fig. 24
9) ACUTE CHOLECYSTITIS:
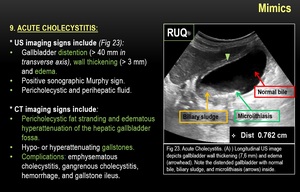
Fig. 25