Certain orbital fractures occur with sufficient regularity to allow a classification into types. This classification has practical value, is that a particular mechanism tends to produce a type of fracture.
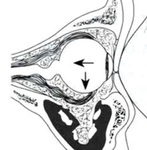
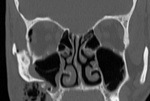
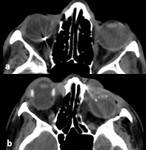
Orbital blowout fractures occur when one of the orbital walls is fractured but the orbital rim remains intact. It is caused by a direct blow to the central orbit from an object larger than the orbital rim. There is an increase of pressure and fractures occur through the weakest portions (lamina papyracea and orbital floor) thus preventing the globe and optic nerve from further injuries. Fig. 3
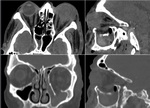
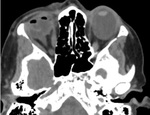
CT with coronal reconstrutions can provide informations regarding components burst into sinus cavities and entrapment of rectus muscles. Fig. 4
Trap door fractures are most common in children, du to the elastic nature of their bones.
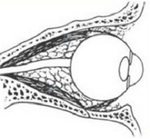
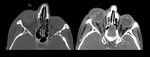
Resulting from an acute transient increase in orbital pressure, A linear orbital wall fracture is created. A flap of bone is outwardly displaced, then immediately returns to its original position. Fig. 5
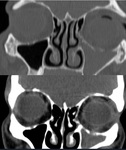
Soft tissue may be ensnared leading to reduced duction of the eye. Urgent release of entrapped tissue is vital to prevent permanent tissue ischemia and definitive diplopia. Fig. 6
External wall and orbital apex fractures
Resulting from direct lateral injury, External wall may be an extension of a zygomaticomaxillary fractures. Radiologic description should include the location of bone fragments and eventual optic nerve impingement. Fig. 7
Orbital apex fractures may be associated with compression of the intracanalicular segment of optic nerve with subsequent loss of vision. Which may indicate a surgical emergency
Orbital blow-in fractures occur when a detached bone fragments moves towards the orbits effectively reducing the volume of the orbit and causing exophthalmos. This type of fractures are usually impure but can be seen as an isolated orbital roof fracture especially in the pediatric population.
It can be associated with pneumocephalus, intracranial hematoma, cerebrospinal fluid leaks, necessitating early neurosurgical consultation.
Intraorbital lesions and complications:
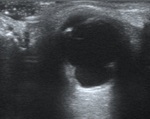
Anterior chamber (AC) injuries such as corneal laceration can be indirectly diagnosticated in case of a decreased anteroposterior diameter of the AC.
Bleeding into AC (hyphema) can be visualized by CT as increased attenuation in the anterior chamber.
Injury to the lens is most commonly caused by blunt trauma to the orbit, causing subluxation of the lens either anteriorly or posteriorly.
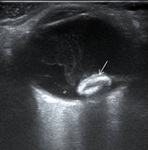
US and CT can aid in the diagnosis through visualizing lens displacement as well as other injuries associated with trauma. Fig. 8 Fig. 9 In diagnosing bilateral subluxation of the lens, non-traumatic etiologies, such as systemic collagenopathies must be ruled out.
Rupture of the globe is a surgical emergency because of the risk of endophthalmitis and monocular blindness. It commonly occurs at the insertion of the intraocular muscles where the sclera is thinnest.
CT is the imaging of choice for the diagnosis with 75% efficiency A number of CT findings may be suggestive such as change in the globe contour with loss of volume (“flat-tire”sign), scleral discontinuity, pneumobulb, and presence of foreign bodies. Fig. 10
This is important to recognize because it is a generally transient and reversible.
Several causes of altered globe contour from congenital (eg, coloboma) Fig. 11 or acquired (eg, staphyloma) nontraumatic deformitie exist, and therefore must be ruled out.
Diagnosis of injury to the globe may be complicated in the presence of previous gas bubble, silicon sponge, or scleral band treatment for retinal detachment, which mimic air or foreign bodies. Fig. 12
Foreign bodies detection are the key element in the radiologic examination of orbital trauma.
Diagnostic accuracy of CT depends on the size, the location and the type of the foreign bodies. Fig. 12
MRI may be useful in doubtful cases, only after the presence of a metallic foreign body is ruled out definitively The higher contrast resolution and the use of fat suppression sequences facilitate the detection of foreign bodies and inflammatory response. Neverless detecting organic foreign bodies remains challenging.
Metallic foreign bodies are generally well tolerated and should be managed conservatively with close monitoring. Indications for surgical removal include neurologic compromise, mechanical restriction of ocular movements, development of acute or chronic infection,or chronic suppurative reaction such as with copper foreignbodies.
Extraocular muscles can be entrapped, avulsed, or lacerated from the trauma. Medial and inferior recti muscles are most commonly involved.
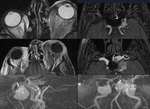
MRI appears superior in detecting lacerated muscle. Fig. 13
Traumatic optic nerve injuries may be direc twhich is rare or indirect, this latter is suspect in the case of rapid decreased visual acuity not corresponding to a fracture diagnosis, suggesting a compression or tearing to the vascular supply of the nerve.
CT may detect compressive hematoma or an impingement of the nerve which indicate urgent surgical exploration. Fig. 13
MRI may detect increased signal intensity on DWI and T2-weighted sequences as a manifestation of direct injury or ischemic lesions Fig. 13
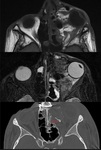
Carotid cavernous fistula is suggested clinically in the presence of post-traumatic diplopia, proptosis, associated with chemosis, hyperemia, and pulsatile exophthalmos typically apparing weeks later after the initial trauma.
CT demonstrates edema and ocular proptosis and dilation of the superior ophthalmic vein. Fig. 14
Because this finding has been reported as normal physiologic variant or in the presence of varix, cavernous sinus thrombosis, and Graves’ disease , diagnosis of cavernous sinus fistula must be confirmed with a CT angiography or conventional angiography.