Normal disc
Normal signal intensity of nucleus pulposus on MRI reflects its high content in water, which is up to 80% in normal discs: imaging appearance is homogeneously hyperintense on T2 weighted images (wI) and homogeneously hypointense compared to normal vertebral marrow on T1wI.
Regarding annulus fibrosus, the inner portion gradually blends with the nucleus pulposus, with similar signal intensity: homogeneously hyperintense on T2wI and homogeneously hypointense on T1wI. The outer portion of annulus fibrosus is composed by collagen type II fibers and appears hypointense on all MRI sequences, especially on T2wI.
Intranuclear cleft: a normal finding in adults around the age of 30, the internuclear cleft is caused by fibrous transformation of the gel-like nuclear matrix. It appears as a horizontal hypointense band on T2w sequences.
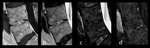
Decreased SI on T2wI
Regarding T2w images, the signal intensity (SI) of the nucleus pulposus has been shown to correlate directly with the proteoglycan concentration; this means that T2wI SI loss correlates directly with progressive degenerative changes in the disc.
Degeneration starts in the nucleus pulposus, with loss of water and elasticity, then spreads to the annulus in which type II collagen increases reducing disc hydration.
The first sign of degeneration consists in disc desiccation: both water content and intradiscal pressure decrease. As intradiscal pressure decreases, mechanical stress on the anulus fibrosus progressively increases, together with T2w changes.
As the degeneration evolve, the disc appears more and more hypointense on both T2 and T1wI and undergoes a reduction in height.
Morphologic classification based on T2wI appearance: to classify these changes, a grading of lumbar disc degeneration has been proposed by Pfirmann et al:
-
Grade I: homogeneous nucleus, hyper or hypointense to cerebrospinal fluid on T2wI, with clear distinction from the annulus. Normal height of the disc.
-
Grade II: inhomogeneous nucleus hyper or hysointense to cerebrospinal fluid on T2wI, may present horizontal hypointense bands. Clear distinction from the annulus. Normal height of the disc.
-
Grade III: inhomogeneous nucleus, hysointense or hypointense to cerebrospinal fluid on T2wI, with unclear distinction from the annulus. Normal to slightly decreased height.
-
Grade IV: inhomogeneous nucleus, hypointense to cerebrospinal fluid on T2wI, with no distinction from the annulus. Reduced height of the disc.
-
Grade V: inhomogeneous nucleus, markedly hypointense to cerebrospinal fluid on T2wI, with no distinction from the annulus. The disc is collapsed.
Level of alteration: degenerated discs are located more often around the thoracolumbar junction and in the lower levels of lumbar spine, where load stress is maximum.
Decreased SI on T1wI
As said before, intradiscal calcifications appear markedly hypointense on T1wI; calcified discs are found in degeneration, but may also develop as a result of trauma, discitis or associated with ankylosing spondylitis.
A linear signal void on T1wI inside a degenerated intervertebral disc may be indicative of vacuum phenomenon: nitrogen gas accumulates inside fissures in degenerated discs, appearing hypointense on all pulse sequences.
Pitfalls: always pay attention to the history of the Patient, for example in case of previous surgery that may mimic discal SI alterations (e.g.: titanium intradiscal cage is markedly hypointense on all pulse sequences).
Increased SI on T2wI
High SI on T2wI is associated with increase of water content inside the disc.
In case of spinal trauma, discal edema in acute stages presents as high SI on T2wI within the disc, paired with reduced SI on T1wI.
Moreover, discal edema is also found in discitis: the association with SI changes in vertebral marrow and paravertebral tissue helps the diagnosis of infection, together with clinical history and laboratory parameters.
Increased SI on T1wI
An increased SI on T1wI after spinal trauma may be caused by subacute intradiscal haemorrhage; as the haematoma chronicize, it may evolve in intradiscal calcification, turning hypointense on T1wI and T2wI images. In these cases, fat suppression helps differentiate between fat and hemorrhagic products of degradation.
Regarding degenerative spine, high SI on T1wI can rarely be found in mild or early stages calcifications, always associated with degenerative changes in the disc. As the calcification progresses, it turns hypointense both on T1wI and T2wI.
Adipose degeneration of intervertebral disc is another rare cause of hyperintense appearance on T1wI; this kind of fat degeneration shows hyperintensity on T2wI, hypointensity on fat suppressed sequences, and no enhancement after contrast media administration.
Pitfalls: diffuse infiltrative disorders of bone marrow may mimic SI alterations of the intervertebral discs, which appear relatively hyperintense on T1w images in comparison with pathological vertebral bodies.
Increased SI on CE T1wI
Contrast media administration, while not required for degenerative spine disease, is fundamental for the evaluation of neoplastic and infectious diseases.
An increased enhancement represents an increase in vascularization inside the disc, and can be caused by inflammatory response, tumoral neoangiogenesis and in rare cases by degenerative changes.
In case of neoplastic infiltration, the disc will be replaced by hypointense tissue on T1wI, more often spreading from adjacent vertebral bodies, with variable sign on T2wI.
Regarding discitis, important edema of adjacent structures is almost always present, with high SI on T2wI.
Lastly, enhancement may be present shortly after discal surgery and must be differentiated from post-operative discitis.
Pitfalls: enhancement may be found in degenerative discs, often with linear intradiscal appearance. Always pay attention to clinical history when evaluating discal enhancement.