1. Anatomy
Patella is the biggest sesamoid bone in the human body and a part of the knee joint.1,2 It is triangular, with basis oriented cranialy, and apex oriented caudaly.1,2 Patella has two sides: rugged ventral side, and smooth dorsal side. 1 On the dorsal side vertical stripe divides the smooth part of patella into two great articular zones, medial and lateral patellar facet.1 Superior third of the patellar ventral side is the site of insertion for quadriceps muscle tendon while the inferior third is the starting point of the patellar ligament.1 Fibers of the rectus femoris and lateral vastus muscle tendon coalesce distaly from the insertion to the patella and form the lateral patellar retinaculum.1,2 On the other side tendon fibers of the medial vastus form medial patellar retinaculum. 1,2,3
2. Etiology
Excessive lateral pressure syndrome (ELPS) has several potential causative factors which all have in common abnormal tension in the lateral retinaculum and chronic lateral patellar tilt.
Firstly it is proposed that pre-existing patelar tilt without symptoms is aggravated after some kind of injury, which adds additional factors to the disequilibrium and only then patient presents with clinical symptoms, firstly pain.4 Also, the lateral retinacular shortening can occur secondary to chronic lateralization or tilt of the patella as adaptive process due to the persistent lateral malalignment.4
Abnormal lateral thetering forces caused by fixation treatment of the fracture, local trauma or capsulitis can also lead to the abnormal tension.4
On the other hand, any type of weaking of medial stabilizers by rupture of the medial retinaculum or atrophy of the vastus medialis will disrupt balance and shift tension power to the lateral side with subsequent patelar tilt. 4
In some cases it is suggested that the cause can be congenital due to the abnormal fascial bands with shortened lateral retinaculum and excesive tension. 4
3. Clinical findings
The most common complaint in patient is the generalized anterior knee pain.4,5 The pain often presents during or after weight bearing activities such as climbing, hiking, running or squating.4,5 It is partially due to amplified tension in already excessively thightent lateral retinaculum and partially because of increased physical interaction between lateral patellar facet and the lateral femoral condyle. 4.5 Crepitus and joint effusion in patellofemoral joint can also occur with time.4,5
Clinical tests that are used to evaluate existance of thigtness of the lateral retinaculum are the patellar tilt test and the extent of the passive medial displacement of the patella. 4,5 When passive translation of patella medially is lesser than 15 mm it is indication of incrased lateral retinaculum thightness. 5 Patellar tilt test is performed by trying to elevate lateral patellar facet more than a 15ᵒ from the starting position, if that is not possible the test is positive and indicative for increased lateral retinaculum thigtness. 4
Test that points to possibility of chondromalacia is Clarke's test of the patellar grind. It is performed in supine position by compression of the superior rim of patella while the patitent contracts the quadriceps muscle which produces pain in the anterior part of the knee. 6
4. Radiological findings and mesaurments
Diagnosis of ELPS is combined effort of clinical examination and radiological findings. Radiogical modalities that are used are plain X ray, MSCT scans and MRI.
Different X ray techniques are used for visualisation of the pattelofemoral joint in assesment of the ELPS . Some of those techniques are prone technique, Knuttson technique, Merchant or Laurin technique and in all of them knee needs to be in 20ᵒ-45ᵒ flexion. 7
On axial radiographs we observe two parameters:
1) the lateral patellofemoral angle
2) indirect radiographic sings of excessive lateral tilt
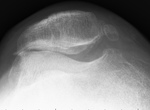
Lateral patellofemoral angle is an angle measured between line that connects most prominent parts of the femoral condyls and line that joins the limits of the lateral patellar facet. 7 When that angle opens to medially it is a direct sign of the excessive lateral tilt. 7
Indirect signs of excessive lateral tilt can be signs of the excessive lateral pressure or excessive lateral ligamentous tension.4 They appear in high grade of chondromalacia with subsequent bone changes. Thickening of subhondral plate, increased densitiy of the lateral facet cancellous bone and medial facet osteoporosis are sings of excessive pressure, while signs of excessive ligamentous tension are fibrosis and calcification of the lateral retinaculum, lateral osteophytes and lateral facet hyperplasia. 4
MSCT and MRI are methods of choice for visualization of the soft tissue, however the MRI is the superior method and is the golden standard for assessment of chondromalacia.
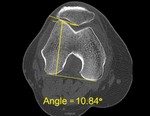
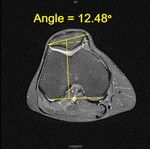
MSCT scans are used for assesment of the patellar tilt by measuring patellar tilt angle and evaluation of soft tissue involved in etiology of ELPS.4 Patellar tilt angle is the angle between the line that connects posterior condyles of femur and the line through specific parts of patella. 4 Different authors take different parts of patella for reference spots which produces the patellar line in angle. The first group describes a patellar tilt angle as angle between line that connects posterior femoral condyles and the line that joins the limits of the lateral patellar facet.4 Their results describe lateral patellar tilt when patellar tilt angle is lesser than 7ᵒ in extension or 12ᵒ-14ᵒ in 20ᵒ flexion. 4 The second group describes patellar tilt angle as the angle between the line that connects posterior femoral condyles and the line that connects medial and lateral border of patella. Their results describe lateral patellar tilt when patellar tilt angle is greater than 10ᵒ in 10ᵒ knee flexion.8
Soft tissue changes, seen on the CT scans and predominantly on MRI, that are associated with ELPS are chondromalacia in patellofemoral joint, soft tissue edema and thickenig of the lateral retinaculum. 4,5
5. Medical treatment options
Treatment can be conservative or surgical.
Conservative medical treatment is used predominatly as a first method of choice in less degeneratively changed femoropatellar joint .5 The goal is to strengthen medial part of the quadriceps muscle and muscles involved in external rotation of the hip while trying to mobilize thight lateral retinaculum and lateral part of the quadriceps muscle.4 It can be achived by focused excersise or wearing orthrosis.4
If those noninvasive treatments do not produce adequat clinical outcome surgical treatment is the next step. In both initial and chronical stages of ELPS surgical release of thight lateral retinaculum can be performed. It is the most common surgical procedure associated with initial lateral patellar arthritis, which in most patients leads to pain relife and reduces the load on the patellar facets.4 In patients with more pronunced patellar arthrosis and chondromalacia in the same act the anteromedial tibial tubercul transfer can be done. 4
Pitfall with releasing lateral retinaculum is excessive cut which can lead to medial dynamic subluxation. On the other hand, if some strings of tighten retinaculum are not released pain persists and can be even more aggrivated which requires another surgical treatment.