OVERVIEW
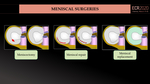
In this work, we review clinical indications, expected post-surgical findings on MRI and potential complications regarding three major surgical options related to meniscal tears: meniscectomy, meniscal repair, and meniscal replacement. (Fig.23). Some meniscal replacement options are still under development, so the information collected in this text will be limited.
INTRODUCTION
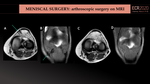
One of the most important starting points for evaluating a postoperative meniscus is knowing what type of surgery has been performed and reviewing previous radiological tests. The clues to prior arthroscopic surgery on MR imaging include linear areas of low signal in all sequences in Hoffa´s fat pad, focal thickening of the patellar tendon, and foci of magnetic susceptibility artifact along the instrumentation tracts. (Fig.24).
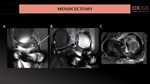
MENISCECTOMY.
Meniscectomy consists of removing the torn meniscus fragment (partial meniscectomy) or the entire meniscus (total meniscectomy, less common). (Fig.41). We describe mainly partial meniscectomy characteristics.
The objective is to remove unstable edges of the meniscus and to leave a meniscal remnant as large as possible, maintaining the peripheral meniscus ring and the meniscocapsular junction.
Clinical indications of partial meniscectomy are summarized in Figure 25.
Normal findings on MRI after surgery:
- May vary from a normal meniscus shape and size (after minimal meniscectomy) to a diminished meniscal volume with or without truncation of the free edge. (Fig.26).
- The presence of a globular or linear signal intensity change on DP and T1-weighted images that may extend to the meniscal surface is a common sign that may persist for years (it may represent a healing process, myxomatous changes or a persistent residual cleft with synovial fluid). (Fig.28)
Postoperative complications:
- Post-surgical tear:
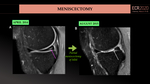
- If the meniscectomy is <25%, the same MRI signs of preoperative meniscus evaluation are used. (Fig.27).
- If the meniscectomy is >25%, the demonstration of fluid signal intensity on T2- weighted images in MRI extending through the meniscus remnant or the presence of contrast on fat-Suppressed T1-weighted images of MR(CT)-arthrography are needed. (Fig.6). Additional criteria to improve the diagnosis: when tear being greater than a third of the length / a third of the height of the meniscus.
- Other signs: Displacement of the meniscal fragment, abnormal signal intensity distant from the location of the surgery.
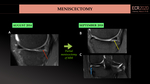
- Accelerated osteoarthritis: is closely associated with the amount of meniscal tissue removed. (Fig.28).
- Osteonecrosis (uncommon).
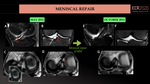
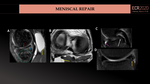
MENISCAL REPAIR
Meniscus repair consists of internal fixation and suturing of the tear using several techniques. (Fig.29,42,43).
Only about 10% of meniscal tears are susceptible to being repaired due to the limited vascular supply of the meniscus. Clinical indications are summarized in Fig.30.
Normal findings on MRI after surgery:
The repaired menisci may show high signal intensity on T1 and DP-weighted images (similar findings as partial meniscectomy) (Fig. 33A, B, D) or normal low signal (Fig.31). Sutures are difficult to delineate.
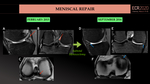
Postoperative complications:
- Recurrent tear (leads to meniscectomy vs new repair): (Fig.32).
- Same radiological signs as post-partial meniscectomy >25% on T2-weighted images, being the MR-arthrography superior as a diagnostic imaging technique.
- Diastasis of the edges of the meniscal repair on T2-weighted images >1 mm.
- Device fracture/migration of all-inside earlier rigid devices: produces mechanical symptoms and pain.
- Arthrofibrosis, stiffness, hemarthrosis, effusion: the patient has pain with a decreased range of motion. Effusion can be aspirated.
- Perimeniscal synovial cyst formation: causes pain and focal swelling. May indicate failure of repair. (Fig.33A,B).
MENISCAL REPLACEMENT
Replacement using meniscal allograft transplant (MAT) or meniscal scaffolds seems to be the most adequate solution to improve persistent pain and limited knee mobility after a meniscectomy, delaying the onset of osteoarthritis.
Meniscus allograft transplantation has been performed over the past 25 years but problems related to graft availability, size matching, and cost-effectiveness limit their widespread use. Therefore, meniscal substitutes have been developed as an alternative to MAT. Currently, three of these implants are clinically available. (Fig.34).
Despite its promising results, only a few numbers of reports have been published on the findings of in-vivo artificial meniscus implants on MRI and their long-term outcomes, so more randomized controlled trials are necessary to support the clinical performance of these devices.
We describe more in detail MAT and collagen meniscal implants because these two techniques are the ones performed in our institution. Clinical indications are summarized in Fig.35.
—>MENISCAL ALLOGRAFT TRANSPLANT (MAT)
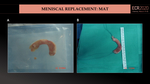
MAT involves the replacement of the meniscus using a cadaveric allograft. (Fig.36,44).
Various surgical techniques are used for allograft transplantation based on fixation of the allograft to the tibia using bone vs soft-tissue fixation. Multiple meniscocapsular sutures are required to fix the allograft meniscus to the joint capsule and the remnant meniscus.
Normal findings on MRI after surgery:
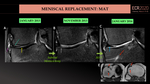
- Allograft meniscus shows high signal intensity present 6-12 months after transplantation, especially the anterior horn, due to normal healing process (cells repopulation, poor organization of collagen fibers). Wavy-appearing meniscus as a result of a tight suture may be seen. A slight meniscal extrusion is a quite common finding. (Fig.37,38).
- Sutures are seen as linear hyper intensities traversing the meniscus obliquely or vertically on a single slice. Suture-knot-related susceptibility artifacts are also encountered frequently.
Postoperative complications:
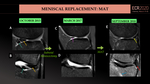
- Dislocation of the allograft as a result of incomplete healing and meniscocapsular detachment. It can vary from moderate to more significant displacement of the graft (MAT failure). (Fig.39).
- Graft shrinkage: due to inappropriate healing/poor revascularization of the allograft.
- Postoperative infection.
- Meniscus tearing: same characteristics as post meniscectomy and post meniscus repair re-tears.
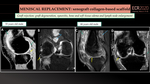
—>COLLAGEN MENISCUS IMPLANT (CMI)
The Collagen Meniscal Implant (CMI) is a xenograft collagen-based scaffold manufactured from highly purified type 1 bovine collagen. The porous, collagen-glycosaminoglycan matrix of the CMI serves as a temporary template to support the migration of the host's cells to the meniscal deficiency, restoring meniscal volume and function.
The scaffold is arthroscopically implanted after performing a partial meniscectomy, and it is sutured to the native peripheral meniscal rim after the revitalization of the margins. (Fig. 45,46).
Normal findings after surgery and complications:
Literature related to expected and abnormal radiologic findings after CMI replacement is limited, so clinical correlation and a thorough inspection of any other knee joint pathology in symptomatic patients is essential.
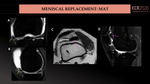
According to a recent study, postoperative findings on asymptomatic patients may be: heterogeneous high signal intensity and irregular margins of the early postoperative CMI (tends to decrease over time), variation of size over time (hypertrophic 1 year after surgery, being less evident in later years) meniscal extrusion (more frequent in the early term after surgery), and femoral chondral defects (more common in the long-term after surgery).
*In our institution, a clinical trial using xenograft collagen-based scaffold manufactured from purified type 1 porcine collagen was performed. Unfortunately, graft rejection (a complication not previously reported after collagen-based scaffold replacement) was diagnosed in 7 patients. (Fig.40).