Diverticulitis is less frequently described in the jejunum than in the colon, probably because of larger diverticula size, better intra luminal flow, and relatively more sterile intestinal contents.
DEFINITION :
Acquired small bowel diverticulum corresponds to an herniation of the intestinal mucosa and submucosa with no muscular layer in the diverticular wall unlike congenital Meckel's diverticulum
Jejunal diverticulitis results from the combination of two factors:
- * the stasis of the intestinal contents in the diverticulum
- * the mucosal edema obstructing the collar favouring intradiverticular microbial growth.
CLINICAL MANIFESTATION :
The clinical presentation of jejunal diverticula can be variable and the diagnosis may be delayed until a complication has emerged
Νο sign or symptom is pathognomonic of small intestine diverticular disease
Jejunal diverticulitis can easily be confused with acute appendicitis, acute cholecystitis, colonic diverticulitis, perforated ulcer
Jejunal diverticula complications are frequent in patients with multiple diverticula .Important ones are :
- diverticulitis
- perforation
- obstruction
- bleeding of patients
Imaging findings:
1/ Ultrasound :
It’s difficult to diagnose jejunal diverticulitis by ultrasound because it’s frequently hindered by intestinal gaz
2/ CT :
- It is currently the key examination for the diagnosis
- CT findings include:
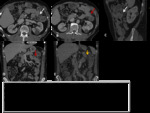
- * Focal and asymetric thickening of the intestinal wall(figure 1 )
- * Abscess adjacent to the jejunal loop
- * eEdema of the surrounding mesenteric fat ( figure1,2)
* inflammatory mass and edema in the surrounding peridiverticular fat(figure1)
- * ‘’arrowhead-shaped collection of contrast’’ sign : which is a nonspecific sign of jejunal diverticulitis as it may be found in appendicitis
- In very rare cases, the inflammation may be very extensive which suggests concomitant inflammation of more than one diverticulum
-- - Pneumoperitoneum is usually found after perforation. However, rarely it can be found without obvious perforation or signs of peritonitis ( figure2,3)
3/ MRE
- It is useful especially when CT is not contributory
- MRE findings include :
* Pronounced focal inflammation of the mesenteric fat adjacent to small bowel wall
* Asymmetric focal wall thickening with less than 5 mm thickness and more than 3 cm length
- * non complicated multiple jejunal diverticula
COMPLICATIONS :
3 important complications :
1/ Perforation : (figure 2,3)
- Perforation is a rare complication : 2.1 to 7% of diverticulitis
- Causes are multiples :
- necrotizing inflammatory reaction
- progressive ulceration
- blunt trauma
- foreign body's impaction
- It leads to localized or generalized peritonitis and digestive fistula
2/ Acute intestinal obstruction :
We can Quote 3 mechanisms :
- Extrinsic intestinal compression by an inflammatory pseudotumor due to jejunal diverticulitis
- Small bowel volvulus due to adhesion band which forms after repeated outbreaks of pauci-symptomatic diverticulitis;
- Fibrous stenosis of the intestine after one or more outbreaks of diverticulitis.
3/ Diverticular bleeding
TREATEMENT :
-Uncomplicated jejunal diverticulitis can be managed with systemic antibiotic therapy and fasting, that should be considered as the first line therapy for stable patients without signs of peritonitis
- However, there is a high risk of recurrence and complications because of the inflammation
- Peri-diverticular abscesses when they are smaller than 5 cm can be treated with CT-guided drainage and antibiotic therapy
- When they are bigger than 5 cm surgery is recommended with - Laparotomy and bowel resection
- Management for perforated jejunal diverticula has no clear guidelines and it is based on isolated reports
- Conservative management with intravenous antibiotics and drainage has been proposed .A few case reports have documented successful management with observation and laparoscopic lavage in cases of micro-perforation
- Because of the high incidence of coexistent colonic diverticula all patients with jejunal diverticulitis must have routine colonoscopy