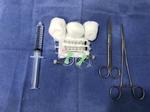
EQUIPMENT:
- A conventional digital X-ray equipment consisting of a X-ray tube and Bucky table. No fluoroscopy required.
MATERIALS:
- A Short-acting topical ophthalmic anesthetic (Proxymethacaine Hydrochloride 0.5%) - 2 drops in each eye.
- 2 Dacryocystogram catheters. See below how to easily make it.
- Gauze pads.
- Cotton balls.
- Oil-based contrast agent (Lipiodol®);1.5 ml for each lacrimal apparatus.
- Two 3 ml syringes.
- Adhesive tape to fix the catheters in the skin.
CATHETER MAKING MATERIALS:(Fig.1)
- Two 27-gauge venous access catheters.
- One straight Kelly tweezers.
- One scissors.
- One 10ml syringe.
- 10 ml of distilled water.
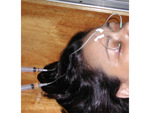
Making dacryocystogram catheters (Fig. 2:video 1):
Use two 27-gauge venous access catheters. Remove their metal end from the plastic tube portion, invert it and insert it back with the bevelled end inwards. Flush them with the distilled water.
TECHNIQUE:
We routinely performed the examination in both eyes. This provides a comparative analysis between the lacrimal pathways (LPW) and also enables to find any abnormalities in the asymptomatic side, while not significantly increasing lens irradiation.
The medial canthus and lacrimal sac (LS) are compressed to empty the LS contents of any fluid present. This enables a better estimation of the size of the LS and also reduces the formation of oil-based contrast droplets that do not dissolve in the tear fluids.
Two drops of anesthetic eye drops are instilled into the conjunctival sac of each eye.
Aspirate 1.5 ml of oil-based contrast material (eg, Lipiodol®) into two 3ml syringes with a luer-lock nozzle. Carefully remove any existing gas bubbles.
The lower eyelid is slightly everted to show the inferior punctum and the inferior canaliculus (IC) is catheterized, first directing the cannula perpendicularly to the lid margin, then rotating it 90 degrees medially, with slight lateral traction of the lower eyelid to cannulate the horizontal portion of the IC. Care must be taken not to place the end of the catheter too medially so as to occlude the origin of the superior canaliculus (SC). With the use of metal catheters, it is not necessary to dilate the punctum. In general, even very stenosed punctuns can be catheterized.
Secure the plastic tube portion of the catheters to the skin of the patient's frontal region with addesive tape (Fig.3), attach the syringes to the catheters and slowly inject the contrast media.
Perform frontal projections approaching the Water's view and obliques views, injecting some amount of contrast media before each x-ray projection, carefully wiping any excess that runs down the face.
Then the catheters are removed, the patient is seated for 5 minutes and then a final frontal radiograph is performed to assess any possible retention of the contrast medium in the LPW.
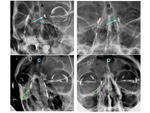
NORMAL ANATOMY:
The LPW is composed of superior canaliculus, inferior canaliculus, commom canaliculus, lacrimal sac and nasolacrimal duct (NLD). There are also some valves created by mucosal folds, mucosal constriction, change in direction of the strutures and kinking and also small anatomic diverticula (see figures 4, 5 and 6 for detailed anatomy).
PATHOLOGY OF THE NASO-LACRIMAL DRAINAGE SYSTEM:
OBSTRUCTION:
Lacrimal system obstruction can be classified as incomplete (10%) or complete (90%) and can be divided into congenital or acquired causes, the second being the most common. Acquired obstruction has several etiologies. It is essential to identify history of trauma, previous surgery, infection, systemic inflammatory conditions or tumors.
The most common cause of obstruction is inflammatory processes involving the NLD, leading to fibrosis and subsequent obstruction. The most common site of strictness is the junction between the LS and the NLD - the valve of Krause, usually associated with increased LS diameter (Fig.7). Middle-aged women are the subgroup with the highest incidence of this condition. Other obstructive causes: topical or systemic medication, radiation, chemotherapy, and even bone marrow transplantation. The next most frequent site of obstruction is the commom canaliculus (CC) (Fig.8). The exact location of the canalicular obstruction site is important because it has therapeutic implications (the type of surgery is different). Obstructions in the distal portion of the CC are more frequent than in the proximal portion. Acquired NLD obstructions tend to be incomplete and are usually associated with paranasal sinus inflammation or neoplastic processes (Fig.9).
LS or NLD neoplasms are rare, they originate from the pseudostratified columnar epithelium and usually cause irregular obstruction, a nonspecific finding, that may suggest the neoplastic possibility.
FISTULAE:
Fistulae are usually associated with long-standing obstruction of the nasolacrimal drainage system and most commonly originates from the LS. They can have a cutaneous opening or the fistulous tract may be incomplete and end bindly in the subcutaneous tissue. They may be congenital, postinflammatory (chronic dacryocistitis), postsurgical or posttraumatic (Fig.10).
DIVERTICULA:
Diverticula result from long-standing obstructions and will remain until the obstructive process resolves. They can be located at the canaculi, LS or NLD (Fig.11).
LACRIMAL CALCULI:
Dacryoliths are conccretions formed in the LS and NLD and are a common and often unrecognized cause of chronic epiphora, recurrent dacryocistitis, punctal discharge and localized swelling. Dacryoliths may be suspected by their intermittent symptons due to positional changes of the lacrimal calculi, and by the inconsistent findings at irrigation (Fig.12). They consist of epithelial cells, lipids, and amorphous debris with or without calcium. Dacryocystorhinostomy with removal of the dacryoliths is the treatment of choice.
CHRONIC CANALICULITIS:
Chronic canaliculitis is more prevalent in women and affects the IC more than the SC. It rarely affects more than one canaliculus and the disease is usually unilateral, having infectious cause by many microorganisms, including bacteria (Actinomyces israelli, Sthaphylococcus, etc.) and virus (herpes, vaccinia, etc) (Fig.13).
POSTTREATMENT:
Dacryocystorhinostomy (DCR) is a surgical procedure with a success rate of about 85%. The procedure consists in promoting a new passage of the tear directly to the nasal cavity, through an osteotomy in the lacrimal bone and suture of the LS in this opening. The operative approach to the LS may be external or endoscopic. Recurrence or persistence of symptoms (epiphora and dacryocystitis) are signs of surgical failure. DCG may then unravel the cause of failure such as lower residual portion of the LS (Fig.14), closure of the osteotomy site, synechia, fibrosis or granulation tissue at the surgical ostium or errors in ostium location.