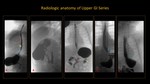
The technique of pediatric UGIS is not the scope of this poster, as it was discussed in details in our previous poster. [ 1]
1]
(Figure 1)
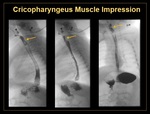
Crico-pharyngeus Muscle Impression:
Normally, a small non-obstructive posterior esophageal indentation at the level of C5-C6. [ 2,
2,  3](Figure 2)
3](Figure 2)
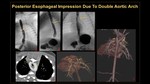
Posterior Esophageal Impressions:
1. Due to Double Aortic Arch (Figure 3)
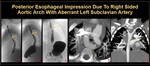
2. Due to right sided aortic arch with aberrant left subclavian artery (Figure 4)
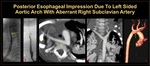
3. Due to left sided aortic arch with aberrant right subclavian artery (Figure 5)
Anterior Esophageal Impression:
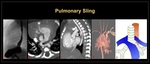
Due to Pulmonary sling (Figure 6)
Whenever the presence of aortic or pulmonary sling is suspected, CT angiography is recommended for better delineation of the vessels.
Esophageal atresia/ Tracheoesophageal fisulta (EA/TEF):
The esophagus and trachea begin as a single tube which divides into 2 separate tubes between 4th and 8th weeks of gestation, if this separation fails to occur properly, EA/TEF is the result.
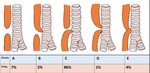
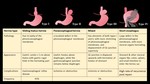
There are several types of EA/TEF, according to Gross classification (Figure 7)
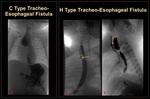
Type C EA/TEF:
It is the most common type TEF, antenatal polyhydramnios is documented, presents in the newborn with vomiting and coiling of the NGT in the blind ended proximal esophagus, which is dilated secondary to the fetus' efforts to swallow amniotic fluid, which may compress the trachea resulting in tracheomalacia.
A fistulous connection between the distal esophageal pouch and the trachea above the carina exists.[ 4]
4]
(Figure 8-A)
Type E (H type fistula)
It is the only type that can be encountered in an UGIS, an ascending tract from the esophagus to the trachea is seen on the lateral view without EA. (Figure 8-B&C)
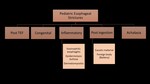
Esophageal strictures: (Figure 9)
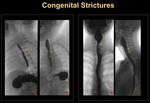
Congenital Esophageal stenosis/webs:
§ Membranous web, usually seen in the proximal or mid esophagus, due to the presence of ectopic tracheobronchial tissue.
§ Esophageal stenosis found in the distal esophagus due to segmental fibromuscular hypertrophy. (Figure 10)
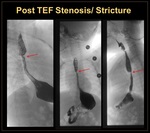
Post TEF correction stenosis:
Anastomotic strictures occur in one third of patients with TEF/EA following surgical repair. Its development is multifactorial, and can be attributed to tension on the anastomosis, gastroesophageal reflux disease, or early postoperative leak. Usually the proximal esophagus continues to appear dilated, as it was dilated antenatally. (Figure 11)
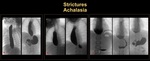
Achalasia
It is a motility disorder of esophagus with absent neurons of the myenteric plexus resulting in impaired relaxation of the lower esophageal sphincter. Mean age of diagnosis in pediatric population is around 8 years. (Figure 12). Follow up UGIS are obtained following balloon dilatation sessions[ 5,
5,  6].
6].
Foreign body Ingestion:
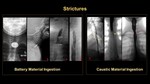
Ingested foreign bodies, like coins and batteries, are most common in children younger than 3 years old. Complications are more likely with a lodged battery in the esophagus, as it can induce severe tissue damage in 15 minutes because of the electrical and chemical injury. The UGIS is helpful in assessing complications, like strictures, perforation, or fistula formation (Figure 13).
Caustic material ingestion:
It is common in children under 5 years of age. Esophageal stricture develops later, in as little as 3 weeks post injury. UGIS help in assessing the stricture progression or improvement following the consecutive balloon dilatation (Figure 13- E till J) [ 5].
5].
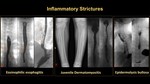
Inflammatory strictures:
Eosinophilic esophagitis:
It is a chronic inflammatory disease that manifests in older children with dysphagia and symptoms of atopy like asthma, or dermatitis[ 5]. (Figure 14-A).
5]. (Figure 14-A).
Juvenile Dermatomyositis (JDM)
JDM is a systemic, autoimmune inflammatory muscle disorder with vasculopathy, presenting with skin rash and muscle weakness. Patients with severe disease may experience dysphagia, due to pharyngeal muscle weakness [ 7]. (Figure 14-B)
7]. (Figure 14-B)
Epidermolysis bullosa:
EB is a rare genetic blistering skin disease. Esophageal stricture is the most common gastrointestinal complication, since the minor trauma of chewing and swallowing results in blister formation and consequent scarring in the proximal esophagus. (Figure 14-C)
STOMACH:
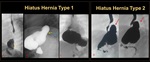
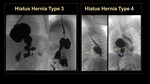
Hiatus hernia (Figure 15-17).
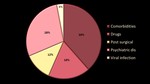
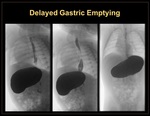
Gastroparesis: Delayed gastric emptying in the absence of mechanical gastric outlet obstruction. Can be due concurrent comorbidities (i.e. seizure disorders, cerebral palsy, developmental delay, prematurity) other psychiatric conditions like ADHD, Bipolar disorder and anxiety, drugs, viral infections and upper abdominal surgeries.
When suspected on UGIS, gastric emptying scintigraphy test with the use of Technetium-colloid labeled meal is done for confirmation. (Figure 18 & 19)
Intestinal atresia:
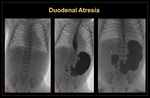
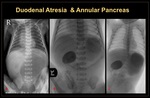
1. Duodenal atresia It is a congenital complete intestinal obstruction due to failure of duodenal re-canalization in 3rd-8th gestational weeks. Obstruction is distal to the ampulla of Vater in 80% of cases. (Figure 20 & 21)
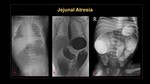
2. Jejunal or ileal atresia It occurs due to an ischemic insult in utero. (Figure 22)
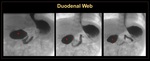
Duodenal stenosis/webs: They are formed due to incomplete recanalization of the duodenum. The double-bubble sign can be seen on abdominal X-ray, with at least a small amount of gas noted distal to the duodenum. (Figure 23)
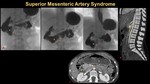
Superior mesenteric artery (SMA) syndrome:
SMA syndrome is due to extrinsic compression and obstruction of the third part of the duodenum by the SMA anteriorly and the aorta posteriorly resulting in failure to thrive.
CT diagnostic criteria:
§ < 10 mm distance between SMA and aorta in sagittal and axial images and
§ Aorta-SMA angle: 6-22°. (Figure 24)
The normal midgut rotation: During embryogenic development, the midgut undergoes 270 degrees of counterclockwise rotation in 3 complex steps (counterclockwise rotation of 90 degrees in each step) to reach its final normal location. Arrest at any of these steps will result in a different abnormal location, ‘malrotation’, which is risky for midgut volvulus.
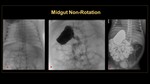
Midgut non-rotation:
It occurs if there is arrest in embryologic rotation after the initial 90 degrees of counterclockwise rotation. (Figure 25)
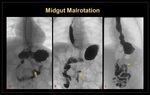
Midgut malrotation: Progression of the midgut rotation process beyond the nonrotation stage brings the duodenojejunal junction and the cecum into closer proximity. Therefore, pathologic arrest along this spectrum will result in a shorter mesenteric pedicle, which increases the midgut volvulus risk. (Figure 26) Midgut malrotation was also documented in cases of congenital diaphragmatic hernia, omphalocele and gastroschisis.
False mimickers of Malrotation:
-Mass effect from: Gastric distension, Left retroperitoneal mass, Splenomegaly
-Chronic bowel dilatation (previous jejunal or ileal atresia).
-Lax ligamentum of Treitz.
-Scoliosis.
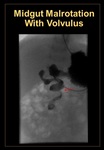
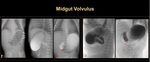
Midgut volvulus: Acute midgut volvulus occurs due to rotation of the duodenum around the axis of the superior mesenteric artery with consequent obstruction at its third portion. Most of the patients present before the first month of life with an acute onset of bilious vomiting. UGI is considered the gold standard examination, where volvulus is seen as a spiral twisting of the duodenum like a “corkscrew” or in the form of a dilated duodenum with complete abrupt obstruction at that level. (Figure 27-28)
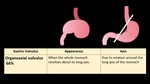
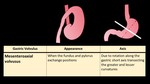
Gastric volvulus types are shown in (Figure 29-30)