We can evaluate CW with a multiplanar reconstruction view and standard technical parameters. CTA has a comparable diagnostic accuracy with DSA for detecting CW, while it is more available and less invasive. Moreover, CTA is more reliable than carotid Doppler ultrasound and is more applicable than MR angiography in the setting of acute stroke. [7,11]
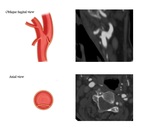
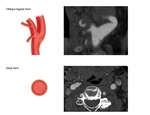
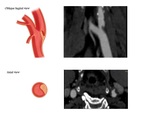
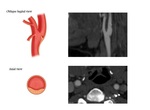
Oblique Sagittal View (OSV): This is the key view in CTA for the detection of CW. [9] There is no further need to coronal nor axial view for the detection of a CW if a proper angle for a well-visualized carotid bulb is used in OSV. In case of finding a sharp intimal protrusion in OSV, a radiologist should confirm or exclude CW by the axial view. In OSV, CW is located exactly in the carotid bulb, and could not be originated from common carotid artery or ICA. There is no available cutoff point for length or thickness of CW. Therefore, any sharp intimal protrusion in OSV, regardless of its length, thickness or angulation, should be cross examined in the axial view. [4] In the multiplanar reconstruction view of each case, a radiologist should consider the direction and position of ICA just at the common carotid bifurcation in axial view for angle adjustment of OSV.
Axial view: A radiologist should establish the diagnosis after the confirmation of CW in the axial view. [6,9] In this view, CW is a complete luminal bridge that arises from one lateral wall reaching to the other side. [Figure 3] Incomplete transverse bridge should not be considered as CW as it seems not to have a significant blood stasis distal to the carotid bulb. [Figure 4] Also CW is normally located in the posterior half of the carotid bulb in the axial view. The bridge located in the anterior third of the carotid bulb should be interpreted cautiously. Moreover, CW in the axial view is not oriented anteroposteriorly, with an exception in the cases that carotid bifurcation is oriented transversely in the axial view.
Differential Diagnosis
A radiologist can confidently report the absence of CW with a properly adjusted OSV in which the posterior wall of the carotid bulb is smooth and without intimal pathology. In the other cases, however, the axial view should also be reviewed in combination with OSV, and differential diagnoses should be considered.
Atherosclerotic plaque: A sharp or ulcerated plaque is the most important differential diagnosis of a CW. The axial view is helpful to distinguish the plaques from CW. The clues which are in favor of the plaque are thick and irregular course, calcified foci, and circumferential or cuplike shape. [Figure 5,6]
Focal intimal thickening: This is a common finding in OSV which has no significant counterpart in the axial view. [Figure 4]
Dissection flap: Dissection flap may sometimes extend down to the carotid bifurcation. CTA shows other signs of dissection such as an abnormal vessel contour, enlargement of the dissected artery, and narrowed lumen. Therefore, this entity can be easily distinguished from CW.
Artifacts: Blood flow artifact can mimic a CW by forming a hypodense puff parallel to the posterior wall of the carotid bulb in OSV. It could be differentiated from CW by scrolling the images in OSV and correlating with the axial view. [Figure 7] Motion artifacts are less confusing as the resultant hazy lines are not limited to the carotid bulb area.
Carotid tortuosity: External folding of a tortuous carotid can indent the lumen and mimics a sharp protrusion in OSV. However, it has no luminal counterpart in the axial view.
Missed CW
Table 1 demonstrates the conditions in which a CW may not be detected in CTA. It is possible to avoid the poor technique image/reconstruction and the poor technical adjustment. However, partial or complete occlusion of the carotid bulb is an inevitable challenge for the detection of CW in CTA. Even a small thrombus can obscure an adjacent CW.