1. Genitally active period:
a-Ectopic pregnancy:
First and foremost, in case of acute pelvic pain in genitally active period, pelvic imaging will aim to eliminate at first an ectopic pregnancy which constitutes a leading cause of maternal death. Main risk factors are tubal surgery or pelvic inflammatory disease(PID)history, intrauterine device, medically assisted reproduction and endometriosis. It mostly occurs in the ampullary and isthmic portions of the fallopian tube .Clinical context is made of amenorrhea, spotting, unilateral pelvic pain and haemorrhagic shock in case of rupture with positive beta-HCG.Ultrasonography is considered the initial imaging modality for the diagnosis. It can show an extrauterine gestational sac with or without an embryo, lack of intrauterine gestational sac and tubal adnexal mass with positive Doppler signal. Tubal swelling with echogenic content (hematosalpinx), decidualized endometrium and free intra peritoneal echogenic fluid (hemoperitoneum) can also be seen. MR imaging is helpful when the diagnosis or location of ectopic pregnancy is unclear. MR finding identify an extrauterine adnexal sac, often separate from the ovary, which follows the signal characteristics of a cyst: low internal signal intensity on T1 wieghted images (T1WI) and high signal intensity on T2 weighted images (T2WI). An hematosalpinx also may be present. Enhanced sequences show parietal enhancement of the gestational sac and tubal wall within an hematoma.
b/ Pelvic inflammatory disease (PID):
PID accounts for approximately a quarter of emergency department visits for pelvic pain.PID is caused by an ascending infection beginning as a cervicitis and can progress to endometritis, salpingitis, and to tubo-ovarian abscess. Main infection agents are Chlamydia Trachomatis, Neisseria gonorrhoeae and Mycoplasma genitalium. Clinical onset is usually vague made of fever,fetid leucorrhoea and inflammatory biological syndrome. PID remains a leading cause of infertility, increases the risk of ectopic pregnancy and may cause chronic pelvic pain. Ultrasonography can identify uni or bilateral dilated tubes and tubal wall thickening with heterogenous echogenic content (pyosalpinx) or heterogenous adnexal mass. CT scan identify tubular adnexal masses with thickened and enhanced walls, ill-defined pelvic fluid with thickening of peritoneal sheets in case of pelviperitonitis. MR imaging may contribute by adding information in case of a disease refractory to initial treatment. Pyosalopinx manifests as a dilated fluid filled tubulated structure with thickened enhanced walls on fat-satured postcontrast T1WI. In addition pelvic inflammation manifests on T2WI as an ill-defined heterogenous isosignal intensity that can be either localized or extensive throughout the pelvis.
*Particular case: Pelvic inflammatory disease due to atypical pathogen: pelvic actinomycosis
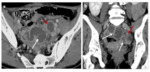
It is a rare chronic suppurative disease favoured by long use of intrauterine device. It is caused by Actinomyces Israelii, an anaerobic Gram-positive bacterium. Clinical presentation is aspecific made of chronic or acute abdominal pain associated with sepsis a.CT and MR findings confirm the infiltrative nature of the disease, which tend to invade across tissue planes and boundaries. CT and MR can also identify inflammatory masses involving the uterus and ovaries.
c/Aseptic context:
*Adnexal torsion :
Adnexal torsion commonly accompanies an ipsilateral ovarian mass or cyst but can also occur in enlarged ovaries (ovarian hyperstimulation, multicystic ovary). Ultrasonography findings identify an enlarged displaced ovary with stroma oedema, peripheral displacement of follicles and often a lead-point cystic or solid ovarian mass. Twisting of the vascular pedicle is pathognomonic. CT and MR findings show an enlarged displaced ovary with displacement of the uterus to the torsion side and fat stranding around the twisted adnexa. In case of haemorrhagic infarction, the ovary may appear spontaneously hyperdense on CT. MR imaging findings include ovarian enlargement, stromal oedema depicted as diffuse high signal on T2WI and in some cases high signal on T1WI and T2WI within the ovary indicating haemorrhagic infarction and necrosis.
*Ovarian cyst rupture:
Corpus luteum cyst > functional cyst> endometrioma, rarely organic cyst.
Ultrasonography findings can often confirm the diagnosis showing a cystic adnexal mass with intracystic non-vascular heterogenous and echogenic pelvic effusion. CT and MR imaging are performed in case of unclear diagnosis showing an haemorrhagic spontaneously hyperdense cyst with disruption of the lateral wall associated with hemoperitoneum.
On MRI, if hematoma begins to develop, the areas of clot will appear as lobulated T2 hypointensitiy with surrounding T2 hyperintense fluid.
*Degenerating fibroids:
Fibroids degeneration often occurs to pedunculated fibroids during pregnancy or post-partum period due to peripheral vessels obstruction. Patients with degenerating fibroids may present with fever, leucocytosis, and physical examination findings that mimic other disease processes such as acute appendicitis or adnexal torsion. They typically appear as a hypodense uterine mass with haemorrhagic hyperdense areas, peripheral wall enhancement surrounded by fat stranding. MR images show peripheral hyperintensitity and central hypointensity on T2WI, peripheral hyperintensity and central hypointensity on T1WI with peripheral wall enhancement of the myoma.
2/ Particular contexts :
a-Post operative/post-partum period :
*Ovarian veins thrombosis :
It is a rare condition most often seen in the immediate postpartum period and more common after a caesarean section on the right side (right ovarian vein compression between the pelvic bones and the uterus) favoured by Virchow triad (venous stasis, hypercoagulability during pregnancy and vascular intimal lesions due to obstetrical maneuvers). CT and MR findings identify a vascular clot and a lack of enhancement in a dilated right ovarian vein with peripheral wall enhancement.
*Post-operative pelvic hematoma or abcess:
Ultrasonography findings include hyperechogenic collection in case of hematoma or heterogenous hypoechogenic collection in case of abscess adjacent to the operation site. CT can confirm the diagnosis showing spontaneous ill-defined hyperdense pelvic hematoma or a fluid collection with peripheral wall enhancement surrounded by fat stranding in the pelvic region.
b-Pregnancy context:
*Placental abruption :
Placental abruption is a serious obstetric complication that often occurs in the third trimester. Diagnosis is usually based on clinical and ultrasound findings showing retroplacental collection with signal characteristics of hyperacute, acute or subacute blood. MRI may be an alternative modality to diagnose abruption and define the size and location of peri placental hematoma.
*Uterine rupture :
Prior caesarean section is the greatest risk factor. It is a rare condition that occurs mostly during labor. Diagnosis is mostly clinical based on abdominal pain with hemodynamic instability. Ultrasonography and MRI can be effective tools to identify partial uterine dehiscence and pre-rupture stages.
c-Puberty context:
*Hematometra and hematocolps
Hematometra and hematocolpos often complicate a pre-existent utero-vaginal malformation and manifest with periodic acute pelvic pain.
Ultrasonography demonstrates a large complex fluid filled structure posterior to the bladder with finely echogenic content surmounted by a dilated small uterine horn. MRI is the best imaging technique showing accurately the underlying malformation and a hyperintensity on T1WI, and hypointensity on T2WI in the proximal vaginal pouch.