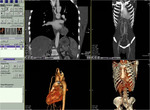
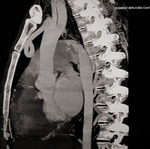
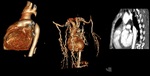
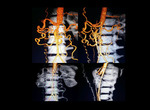
CT Technique:
CTA of the aorta should cover the area from a level 3 cm above the aortic arch to the level of the femoral heads. Currently the standard tube voltage for CTA is 120 kV. The tube current should be approximately 120 mAs, and automated dose modulation should be used. To avoid such artifacts related to beating heart, use of retrospective ECG gating is recommended for imaging of the heart, the aortic root, and the ascending aorta. In this review, images are from CTA performed on 128 slice MDCT scanner.
⇒ Aortic Dilatation:
The normal aortic annulus measures 26.3 mm ± 2.8 mm in the coronal plane and 23.5 ± 2.7 mm in the sagittal plane 12.
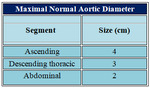
The normal ascending aorta measures 3.6 cm in females and 3.8 cm in males 13.
The proximal descending aorta is considered enlarged when it exceeds 2.6 cm and the distal descending aorta is considered enlarged when it exceeds 2.4 cm.
An aneurysm is diagnosed when the ascending aorta is larger than 5 cm and the descending aorta is larger than 4 cm 13. High risk for aortic rupture or dissection is when aortic diameter exceeds 6cm for descending thoracic aorta and 7cm for abdominal aorta.
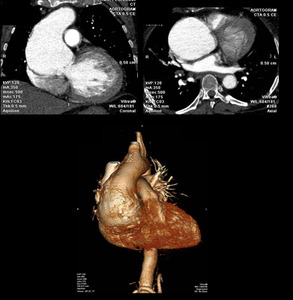
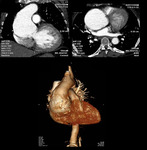
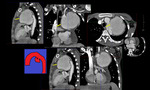
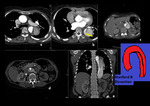
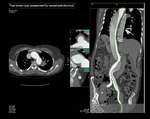
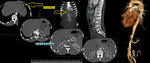
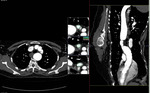
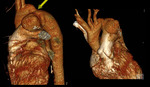
Fig. 2: Curved coronal, axial reformat and 3D voulme rendered images showing large ascending aortic aneurysm involving the sinus of valsalva and ascending aorta.
Annuloaortic Ectasia:
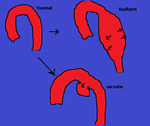
Annuloaortic ectasia or sinotubuluar ectasia is symmetric dilation of the aortic root and ascending aorta with effacement of the sinotubular junction. The ascending aorta has a pear shaped appearance.
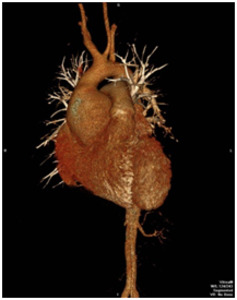
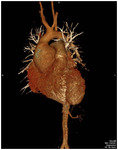
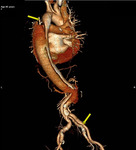
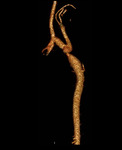
Fig. 3: Volume rendered 3D reformatted image of CT Aortogram in a young patient having pear shaped dilated aortic root and ascending aorta with effacement of the sinotubular junction consistent with Annuloaortic ectasia.
Aneurysm:
An aneurysm is defined as permanent localized dilation of the aorta, either 50% or 2 standard deviations larger than normal expected diameter for that aortic segment15.
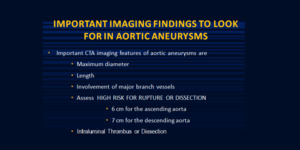
Fig. 4: What to look for in Aortic aneurysm
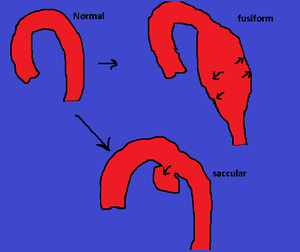
Fig. 5: A fusiform aneurysm has symmetrical dilation involving the entire circumference of the aortic wall, while a saccular aneurysm is more localized with outpouching of one portion of the aortic wall.
True and pseudo aneurysms: All the three mural layers are involved in true aneurysm. Pseudoaneurysms are usually saccular and are most commonly the result of trauma, infection, instrumentation, or penetrating atherosclerotic ulcers (Figure.6 and 7).
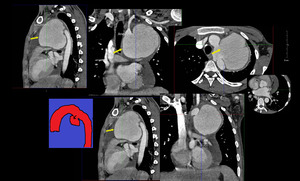
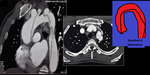
Fig. 6: Saccular Aneurysm. Multiplanar reformatted 2D images of CT Aortogram showing large saccular aneurysm of distal arch and proximal descending aorta. It has a wide neck and possibility is of mycotic aneurysm.
Traumatic pseudoaneurysm most commonly occurs at the isthmus (90%)15.
Thoracoabdominal aneurysms:
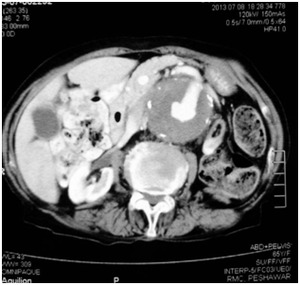
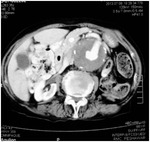
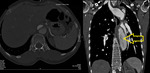
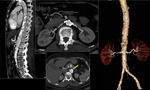
Fig. 8: Axial CT image of a 65 years old female showing a large peripherally thrombosed aortic aneurysm in abdominal aorta. It is involving the origin of Superior mesenteric artery.
Mycotic Aneurysm:Mycotic aneurysms can be multiple and are usually saccular with a wide neck15.
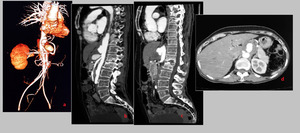
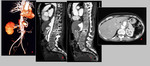
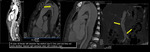
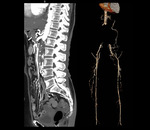
Fig. 9: Multiplanar CTA images of a 50 years old female with saccular mycotic aneurysms of aorta and celiac artery, like Tuberculous. Sagittal images show multilevel spondylodiscitis consistent with caries spine. The aneurysm has a wide neck and partly thrombosed lumen.
⇒ Dissection:
Dissection is the most common cause of acute aortic syndrome. The Stanford classification is used to describe aortic dissection (Figure.10,11).
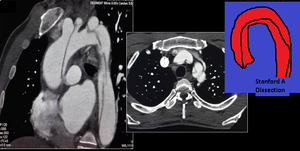
Fig. 10: 35 years old male with acute chest pain. Curved MPR images reveal STANFORD A dissection.
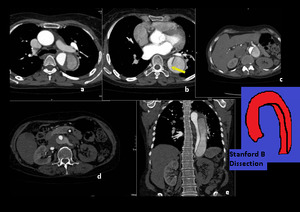
Fig. 11: STANFORD B dissection. CTA images revealdDissection flap in descending aorta with both true and false lumens. Arrow shows site of flap tear. Celiac trunk has origin from true lumen. Left renal artery is being supplied by false lumen with resultant hypoperfused left kidney.
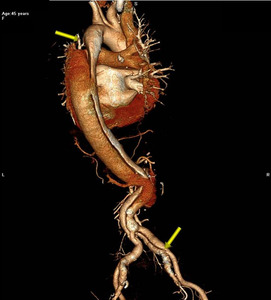
Fig. 12: 3D CT Aortogram showing Stanford B Dissection extending into iliac arteries.
CT shows an intimal flap separating true from false lumen (Figure. 10,11)). The true lumen maintains direct continuity with the undissected proximal normal aorta and is usually smaller than the false lumen. The false lumen can also be identified by the presence of cobweb sign (Figure.13).
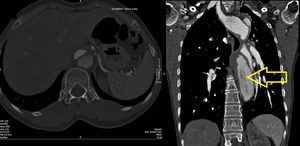
Fig. 13: Stanford B dissection in a 45 years old female. Cobweb sign seen in the false lumen.
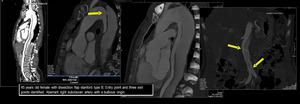
Fig. 14: Aortic Dissection (Stanford B)
CT can measure the length of dissected segment, lumen involved, volume and longitudinal extent by different post processing techniques (Figure 15, 16). Complications of aortic dissection include aortic rupture, aortic branch vessel obstruction and end-organ ischemia (Figure.17).
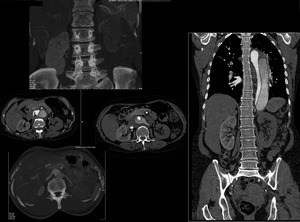
Fig. 17: Stanford B dissection and left kidney being supplied by the false lumen with resultant hypoperfusion of left kidney. Note the difference of cortical density in both kidneys.
Intramural hematoma:
Intramural hematoma (IMH) is characterized by spontaneous hemorrhage into the tunica media of the aorta.It is only visible on non-contrast CT scan ( Figure below).
Figure below).
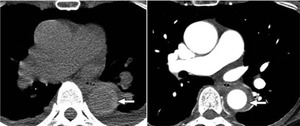
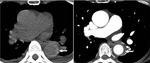
Fig. 18: 50-year-old woman with acute chest pain. Unenhanced low-dose CT image shows relatively hyperdense intramural hematoma surrounding descending aorta
On contrast-enhanced CT image, intramural hematoma is visually less conspicuous.
References: https://www.ajronline.org/doi/full/10.2214/AJR.08.2166
⇒ Traumatic Aortic Injury:
Direct CT findings of acute aortic injury include deformity of the aortic contour, intimal flap, intraluminal debris, pseudoaneurysm, and intramural hematoma 21.
⇒ Aortitis:
Aortitis (vasculitis) is characterized by inflammation of aortic wall with reactive damage to mural structures (Figure.19). CT shows thickening of the vessel wall and mural contrast enhancement in early stages; stenoses, occlusion, and aneurysms characterize the later stages19.
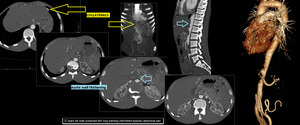
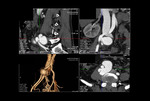
Fig. 19: Aortitis. 27 years old male presented with long standing intermittent episodic abdominal pain. CT Aortogram sagittal, coronal and 3D surface rendered images showing irregular thickening of anterior wall of upper abdominal aorta, consistent with aortitis. Numerous collaterals noted.
⇒ Atherosclerosis:
Patchy areas of calcified and noncalcified mural and intimal plaques are seen in most of the aging aortas. CT is useful in assessing involvement of main branches at their origin. Severity of disease ranges from mild to severe. Atherosclerotic disease can also manifest as protruding atheromas, debris and plaque. Plaques with high risk for embolization are those that are ≥4 mm thick.
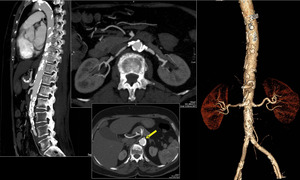
Fig. 20: Atherosclerosis. Calcified and non-calcified plaques are seen in aorta and its visualized branches.
Aorto-iliac occlusive disease:
Aorto-iliac occlusive disease is most frequently a chronic condition related to the deposition of atherosclerotic plaque at the level of the aortic bifurcation23 (Figure.21).
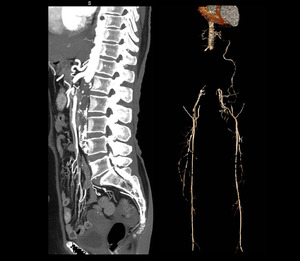
Fig. 21: Aorto-iliac Occlusive disease. Severe atherosclerotic disease occluding the abdominal aorta and aortic bifurcation. Multilevel focal stenosis seen in both lower limb arteries evident on 3D volume rendered image.
⇒ Arteriovenous Fistula (AVF):
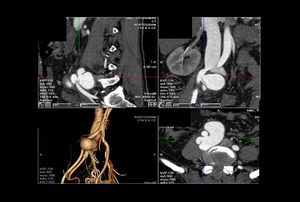
Fig. 22: CT Aortogram of a 36 years old male showing Arteriovenous Fistula of right iliac vessels with aneurysmal dilatation.
⇒ Post op Complications:
CT has important role in diagnosisng complications in operated Aorta, like Aortic valve replacement (AVR), Aortic aneurysm repair, grafting, stenting etc. Post op complications range from intramural thrombus, vegetations, dissections to rupture of repaired segment (Figure 23, 24).
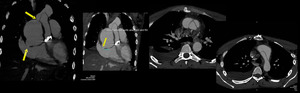
Fig. 24: 23 years old young male, post aortic valve replacement, presented with a large pseudoaneurysm with a dissection flap at aortic root region. CT aortogram revealed three connections of pseudoaneurysm with right atrium, aortic root and ascending aorta.
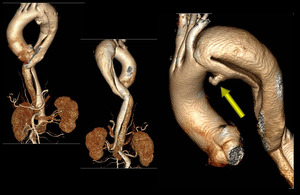
Fig. 23: 55-year-old female, post coarctation repair with chest pain. 3D volume rendering of contrast-enhanced CT show Stanford type B dissection separating smaller anterior true lumen from posterior false lumen of descending aortic aneurysm, dissection flap extending upto bifurcation and involving right common iliac artery; a small PDA aneurysm seen.
Congenital Aortic diseases:
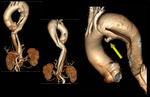
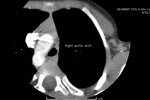
⇒ Right aortic arch:
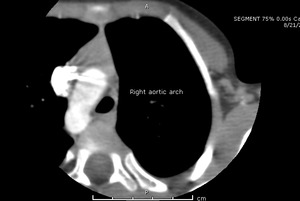
Fig. 25: Right Aortic Arch.
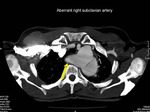
⇒ Aberrant subclavian artery:
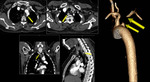
Anomalous right subclavian artery (Figure.26) that originates distal to the left subclavian artery in a left-sided arch configuration. The infundibular origin may become aneurysmal, like in Figure.26 (Kommerells diverticulum). It often exhibits circumferential atherosclerotic changes (Figure.27).
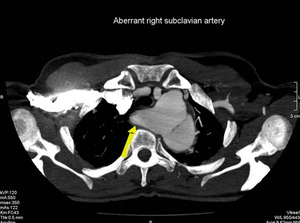
Fig. 26: There is aberrant right subclavian artery with kommerell’s diverticulum.
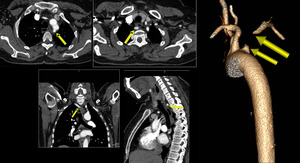
Fig. 27: Multiplanar and 3D images of CT Aortogram showing severe thrombotic occlusion of proximal segment of aberrant right subclavian artery.
⇒ Coarctation:
Coarctation of the aorta is a congenital malformation and is most commonly manifested as a focal narrowing or diaphragm-like ridge in a juxtaductal location. In addition to discrete narrowing, associated hypoplasia may be present and involve a portion or all of the aortic arch25.
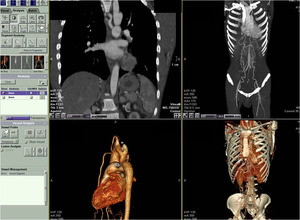
Fig. 28: Aortic Coarctation (Ductal Type). Multiple collaterals are seen. MDCT workstation allows different post processed images viewed at once i.e. MPR, curved MPR, 3D surface rendered, 3D volume rendered without bone.
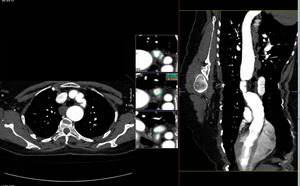
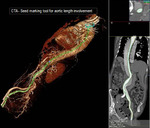
Fig. 29: Coarctation. CTA reformatted images. CT can measure the exact length of the involved segment by post processing. The slices for the measurements should be manually adjusted separately for each aortic level to get an oblique plane that is strictly perpendicular to the course of the aorta.
Role of CT in patients with aortic coarctation is to detect associated cardiac anomalies, the diameter of the aorta especially after treatment to assess stability of the repair and detect complications early, for depiction and quantification of post stenosis dilatation, ascending aortic ectasia, aortic arch hypoplasia and re- coarctation or Formation of a local aneurysm or pseudoaneurysm at the previous site of coarctation (Figure.23).
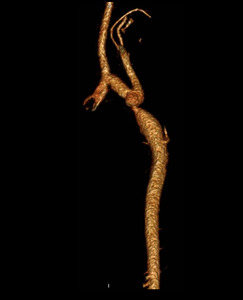
Fig. 30: Coarctation. 3D CTA image showing ductal type coarctation with pre-stenotic aneurysmal dilatation.
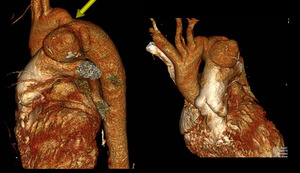
Fig. 31: Coarctation (arrow) with large PDA (persistent ductus arteriosum) and aneurysm of main pulmonary artery seen here as focal outpouching.
⇒ Aortic interruption:
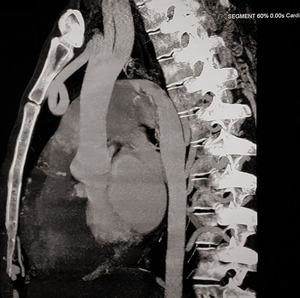
Fig. 32: Aortic Interruption. Descending aorta is being supplied by large PDA. No direct connection between arch and descending aorta seen.
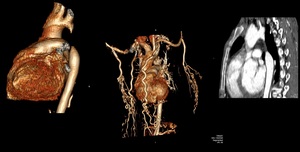
Fig. 33: Aortic Interruption. Non-visualization of small segment of proximal descending aorta seen on sagittal reformatted images.Multiple collaterals seen in middle image.
⇒ Midaortic Syndrome:
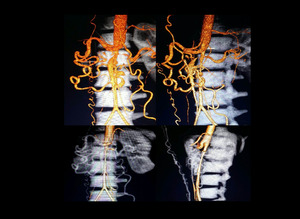
Fig. 34: CT Aortogram 3D surface rendered images showing midaortic syndrome seen as long narrow segment of abdominal aorta. There was occlusion of celiac trunk and superior mesenteric arteries with resultant opening up of various collateral pathways like arc of Riolan.