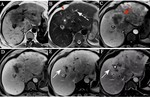
-Differential diagnosis of the most common delayed-enhancing hepatic focal lesions (Fig.4)

Fig. 4
References: Department of diagnostic radiology,Theodor Bilharz research institute,Giza/EG
1-Malignant lesions:
A-Intrahepatic cholangiocarcinoma (ICC):
- The second most common primary hepatic tumor after HCC.
- ICC may also be classified according to their growth pattern or morphologic subtype(Fig.5).
- 90% are adenocarcinomas with abundant fibrous stroma.
- The mass forming type is the most common (80%).

Fig. 5: Morphologic classification of ICC.
References: Alsaleh M et al. (2019) Cholangiocarcinoma: a guide for the nonspecialist. International Journal of General Medicine 12:13–23 International Journal of General Medicine 2019:12 13–23
-Mass forming Intrahepatic cholangiocarcinoma
- Hypointense on T1WI.
- Variable hyperintense on T2WI, depending on the relative proportions of fibrous stroma vs extracellular mucin and necrosis.
- The most common enhancement pattern is early arterial peripheral enhancement with progressive central filling with or without peripheral washout (Fig.6,7).
- In predominantly fibrotic tumors, enhancement may only be visible in the delayed phase.
- Associated secondary signs including bile duct dilatation distal to the tumor, capsular retraction and satellite nodules help in differentiation.

Fig. 6: Diagram demonstrating progressive delayed enhancement and secondary signs of mass forming intrahepatic cholangiocarcinoma.
References: Start radiology,CT abdomen general

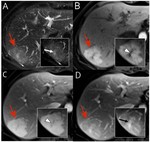
Fig. 7: Intrahepatic mass forming cholangiocarcinoma:(A)Axial precontrast T1WI demonstrating a hypointense mass in segment VIII and IV of the liver.(B)Axial T2WI demonstrating a mildly hyperintense mass with central necrotic areas of higher T2 signal(asterisk),capsular retraction(arrow head)and minimal intrahepatic biliary dilation(dashed arrow).(C,D) Arterial and portal phases demonstrating a continuous ring of peripheral enhancement corresponding to active tumoral cells (red arrows). (E,F) Delayed phase demonstrating progressive central enhancement (white arrows) with no enhancement of the necrotic areas(asterisk).
References: Department of diagnostic radiology, ALFA medical group, ALFA scan, Giza/EG
-Periductal infiltrating intrahepatic cholangiocarcinoma:
- The majority is perihilar intrahepatic in location.
- Periductal irregular thickening with or without variable parenchymal infiltration.
- Hypointense on T1WI, variable on T2WI with progressive delayed contrast enhancement (Fig.8).

Fig. 8: Periductal infiltrative intrahepatic cholangiocarcinoma:(A)Precontrast axial T1WI demonstrating a hypointense infiltrative mass in segments II and III of the left hepatic lobe (arrow).(B)and(C) Axial and coronal T2WI demonstrating an ill-defined perihilar infiltrative heterogeneous mass (white arrows) with associated intrahepatic biliary dilatation (red arrow). (D)arterial phase shows early marginal enhancement of the lesion.(E,F) portal and delayed phases show progressive enhancement of the lesion.
References: Department of diagnostic radiology, ALFA medical group, ALFA scan,Giza/EG
-Intraductal cholangiocarcinoma
- Proliferates focally within the biliary duct lumen.
- Low-grade malignancy; carries the best prognosis.
- A nodular well-defined mass that is hypointense on T1WI, hyperintense on T2WI with delayed enhancement (Fig.9).

Fig. 9: Intraductal cholangiocarcinoma: (A) Axial T2WI demonstrating a mild hyperintense intraductal mass within the dilated right and left hepatic ducts (arrow). (B) Axial precontrast T1WI demonstrating a corresponding intraductal hypointense mass. (C) Delayed post-contrast MR image demonstrating delayed enhancement of the intraductal mass (arrow).
References: Mittal P et al. (2015) Primary biliary tract malignancies. Abdominal imaging 40:1520-1557
B-Fibrolamellar carcinoma (FLC):
- A rare variant of hepatocellular carcinoma.
- It affects young adults with a history lacking known risk factors and chronic liver disease.
- Usually hypointense on T1WI and hyperintense on T2WI.
- It shows arterial enhancement and becomes hypointense on the late phases.
- Uniformly T1 and T2 hypointense radial septae and a central scar in 70% of cases show minimal or partial delayed enhancement (Fig.10,11).

Fig. 10: Diagram demonstrating enhancement pattern of fibrolamellar carcinoma with delayed partial scar enhancement.
References: Modified by department of diagnostic radiology,Theodor Bilharz research institute,Giza/EG

Fig. 11: Fibrolamellar hepatocellular carcinoma.(A)Axial T2WI shows that tumor (arrow) has heterogeneous high signal intensity. The central scar is hypointense on T2WI (arrowhead).(B) Arterial phase shows heterogeneous enhancement within the mass (arrow). No enhancement is seen within the central scar (arrowhead).(C) Delayed phase shows partial enhancement of the central scar (arrowhead).
References: Ganeshan D et al. (2014) Imaging Features of Fibrolamellar Hepatocellular Carcinoma. AJR 202: 544-552
- Calcification is frequent and difficult to identify on MRI and better seen in CT (Fig.12).

Fig. 12: FLC central scar calcification in CT
References: Mittal P et al. (2015) Primary biliary tract malignancies. Abdominal imaging 40:1520-1557
C-Metastasis:
- The most common malignant liver lesions.
- They occasionally show delayed enhancement which is caused by abundant fibrous tissue in the tumor.
- Hypointense on T1 and mildly hyperintense on T2.
- They show peripheral band enhancement on arterial phase and delayed phase central enhancement with characteristic peripheral washout(Fig.13,14).
 "Peripheral washout sign"
"Peripheral washout sign"

Fig. 13: Diagram demonstrating enhancement pattern of metastasis.
References: Modified by department of radiology,Theodor Bilharz research institute,Giza/EG

Fig. 14: Metastatic liver tumors. (A)T2WI shows multiple mild hyperintense lesions in the liver. (B) Arterial phase shows early band like enhancement of the lesions (red arrows). (c) Delayed phase shows progressive central enhancement with a hypointense rim “peripheral washout sign”(white arrows).
References: Department of diagnostic radiology, ALFA medical group, ALFA scan, Giza/EG
D-Rare malignant lesions (Fig.15):

Fig. 15
References: Mittal P et al. (2015) Primary biliary tract malignancies. Abdominal imaging 40:1520-1557
- Cholangiocellular carcinoma (Fig.16)

Fig. 16: Pathologically proven cholangiocellular carcinoma: (A) Arterial phase showing ring-like peripheral enhancement of the mass (arrow) but no enhancement of the central aspect of the lesion (hollow arrow).(B) Delayed phase demonstrating a progressive enhancement of the central aspect of the lesion (hollow arrow) with washout of its periphery(arrow).
References: Mittal P et al. (2015) Primary biliary tract malignancies. Abdominal imaging 40:1520-1557
- Primary biliary lymphoma (Fig.17)

Fig. 17: Pathologically proven primary biliary lymphoma: (A) Axial T2WI demonstrating a hyperintense lesion surrounding the right hepatic duct (arrow). (B) Precontrast axial T1WI demonstrating the corresponding low signal lesion (arrow). (C) Delayed phase demonstrating a progressive enhancing soft tissue mass (arrow).
References: Mittal P et al. (2015) Primary biliary tract malignancies. Abdominal imaging 40:1520-1557
- Lymphoepithlioma like carcinoma (Fig.18)

Fig. 18: Pathologically proven lymphoepithelioma-like carcinoma:(A)Axial T2WI demonstrating a hyperintense lesion.(C)delayed phase demonstrating a progressive enhancing mass(arrows).
References: Mittal P et al. (2015) Primary biliary tract malignancies. Abdominal imaging 40:1520-1557
2-Benign lesions:
A-Hemangioma:
- The most common benign tumor of the liver.
- It Consists of blood-filled cavities and fed by the hepatic artery.
- It is classified into small (few mm-3 cm), medium (3 cm-10 cm) and giant hemangiomas (>10cm).
- Small hemangiomas typically exhibit hypointense T1, marked hyperintense T2 signal with early peripheral nodular enhancement and progressive complete fill-in on portal and delayed phases (Fig.19,20).

Fig. 19: Diagram demonstrating enhancement pattern of hemangioma. Early phases show peripheral nodular enhancement and delayed phase shows progressive fill-in corresponding to accumulation of contrast material in the large intravascular spaces.
References: Start radiology,CT abdomen general

Fig. 20: Typical hepatic hemangioma. (A) heavy T2WI shows hyperintense lesion in segment II (arrow).(B,C) Arterial and portal phases show peripheral nodular enhancement of the lesion (arrows). (D) Delayed phase shows progressive complete fill-in (arrow).
References: Department of diagnostic radiology, ALFA medical group, ALFA scan,Giza/EG
-Small hemangiomas should be differentiated from delayed-enhancing metastasis (Fig.21).

Fig. 21: Main discriminatory features between hemangioma (A,B) and metastatic lesions (C,D).
References: Department of diagnostic radiology, ALFA medical group, ALFA scan, Giza/EG
- Giant hemangiomas usually show partial fill-in on delayed phase and sometimes difficult to differentiate it from malignant neoplasms.
- The central scar in giant hemangiomas is typically large and bright on T2WI (Fig.22).

Fig. 22: Giant hepatic hemangioma.(A) heavy T2WI shows hyperintense lesion in segment V and VI of the right hepatic lobe with bright central scar(asterisk).(B,C) Arterial and portal phases show peripheral nodular enhancement of the lesion. (D) Delayed phase shows progressive incomplete fill-in with non enhancing scar (asterisk).
References: Department of diagnostic radiology, ALFA medical group, ALFA scan,Giza/EG
B-Focal nodular hyperplasia (FNH):
- The second most common benign liver tumor.
- It is a regenerative lesion rather than a true neoplastic lesion.
- Typically show iso- or hypointense T1 and slightly hyper or isointense T2 with intense arterial homogeneous enhancement.
- The central scar is typically high on T2WI, low on T1WI and shows visible enhancement on delayed images (Fig.23,24).
- The T2 signal and enhancement of the central scar may be caused by the inflammatory reaction around the ductular proliferation and the malformed vessels within.
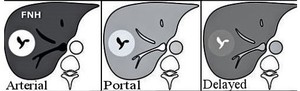
Fig. 23: Diagram demonstrating enhancement pattern of focal nodular hyperplasia. Early phases show intense homogeneous enhancement of the lesion with a non enhancing scar and delayed phase shows isointense lesion with typical scar enhancement.
References: Start radiology,CT abdomen general

Fig. 24: Typical FNH. (A) Axial SPAIR image shows a FNH lesion at segment VII (red arrows) that is hyperintense relative to the surrounding liver parenchyma. The central scar (white arrow) has slightly higher signal intensity than the lesion. (B,C)arterial and portal phases show intense homogeneous enhancement of the entire lesion, except for the central scar (arrow head). (D) delayed phase shows that the lesion has become isointense relative to the surrounding liver parenchyma, and the central scar (black arrow) has complete enhancement.
References: Department of diagnostic radiology, ALFA medical group, ALFA scan,Giza/EG
-FNH scar should be differentiated from other scar-containing lesions (Fig.25).

Fig. 25: Characteristic features of giant hemangioma, FNH and FLC central scars
References: Department of diagnostic radiology, ALFA medical group, ALFA scan, Giza/EG
C-Confluent hepatic fibrosis (CHF):
-The term confluent fibrosis means the formation of thick fibrotic scars with a mass-like appearance.
- Typically it has a wedge or geographic shape, radiates from the hilum to hepatic surface, retracts the overlying capsule and is associated with progressive volume loss in follow up studies(Fig.26).
- It appears iso- to hypointense on T1WI and slightly hyperintense on T2WI because of the underlying edema and remnant portal triads.
- It is usually non-enhancing but may show minimal enhancement in the hepatic arterial phase. It shows progressive enhancement in the delayed phase (Fig.27).

Fig. 26: Diagram demonstrating enhancement pattern of confluent hepatic fibrosis. A peripheral wedge shaped area with associated capsular retraction but no appreciable enhancement in early phases with Delayed phase enhancement.
References: Modified by department of radiology,Theodor Bilharz research institute,Giza/EG

Fig. 27: Confluent hepatic fibrosis.(A) Axial SPAIR image shows a mild hyperintense wedge shaped subcapsular area at segment VIII/IVa (arrow) and associated capsular retraction (arrow head). (B)arterial phase shows non enhancement of the lesion (arrow).(C) delayed phase shows homogeneous enhancement of the lesion (arrow).
References: Department of diagnostic radiology, ALFA medical group, ALFA scan,Giza/EG
D-Post treatment changes of HCC:
- On early phases; non-enhancement of the lesion and lack of delayed washout denote successful treatment.
- On delayed phase; a thin enhancing rim surrounding the treated cavity is usually seen, representing reactive granulation tissue, rather than a residual tumor (Fig.28,29).

Fig. 28: Diagram showing delayed marginal enhancement in a treated HCC lesion corresponding to perilesional granulation tissue/fibrosis.
References: Modified by department of radiology,Theodor Bilharz research institute,Giza/EG

Fig. 29: (A) Axial T1WI shows a well defined lesion of high signal at segment V (white arrow). (B) axial T2WI shows a corresponding hypointense lesion. (C,D) arterial and subtraction arterial phases show non enhancement of the lesion i.e no evidence of tumoral viability. (D)delayed phase shows marginal enhancement of the lesion caused by perilesional granulation tissue (red arrow).
References: Department of diagnostic radiology, ALFA medical group, ALFA scan, Giza/EG
E-Pyogenic liver abscess:
-The most common type of visceral abscess
-Fever and right hypochondrial pain usually present.
- It displays central low T1 and high T2 signal.
- The double target sign is denoted on T2WI by an iso- to hypointense inner layer (pyogenic membrane) and a hyperintense outer layer (oedema)
 double target sign.
double target sign.
- Early enhancement of the inner layer that persists in the delayed phase with delayed enhancement of the outer layer (Fig.30,31).
- Perilesional parenchymal hyperemia manifests as patchy enhancement in early phases.
- Restricted diffusion is generally seen.

Fig. 30: Diagram demonstrating enhancement pattern of a pyogenic liver abscess. Arterial and portal phases show early enhancement of the inner layer and adjacent hepatic parenchymal hyperemia. Delayed phase shows enhancement of the inner and outer layers.
References: Modified by department of radiology,Theodor Bilharz research institute,Giza/EG

Fig. 31: Pyogenic liver abscess from acute gangrenous cholecystitis i. (a) Axial T2WI shows the double target sign of the abscess wall, seen as an iso- to hypointense inner layer (arrowhead) and a moderately hyperintense outer layer (arrow) surrounding the internal high-signal-intensity content of the abscess. Note the impacted hypointense stone in the gallbladder neck (*). (B) arterial phase shows early enhancement of the inner layer (arrowhead) and adjacent segmental hepatic parenchymal hyperemia (red arrow). (c) delayed phase shows delayed enhancement of the inner and outer layers (arrow).
References: Bächler P et al. (2016) Multimodality Imaging of Liver Infections. Radiographics 36:1001-1023
F-Rare benign lesions:
-Hepatic inflammatory pseudotumor (Fig.32):
- An uncommon disorder that mimics a malignant tumor.
- Patients present with fever, abdominal pain, and jaundice.

Fig. 32: Inflammatory myofibroblastic tumor:(A)Axial T2WI demonstrating a hyperintense lesion involving segment IVA of left hepatic lobe (arrow).(B) Precontrast axial T1WI demonstrating the corresponding low signal lesion (arrow). (C) and (D) Arterial and delayed post-contrast axial images demonstrating a progressive enhancing soft tissue mass (arrow).
References: Mittal P K et al. (2015) Primary biliary tract malignancies. Abdominal imaging 40:1520-57
-Peliosis Hepatis (Fig.33):
- A rare disorder, characterized by the presence of multiple small (1–3-mm) blood-filled lacunar spaces.
- Seen in patients with chronic wasting due to tuberculosis or cancer and is associated with the administration of anabolic steroids and oral contraceptives.
- Branching appearance of contrast in delayed phase may help in diagnosis.

Fig. 33: Peliosis hepatis. A lesion (arrow) shows progressive enhancement from arterial (A) to portal venous (B) and delayed (C) phases, with “branching” appearance. Because of progressive fill-in of contrast enhancement, findings were initially thought to be consistent with hemangioma. Percutaneous biopsy of lesion (not shown) was consistent with hepatocellular adenoma. However, histologic examination performed on resected surgical specimen showed peliosis hepatis.
Centripetal enhancement in peliotic lesions is rather uncommon finding; branching appearance of contrast enhancement in delayed phase is useful sign that may help in diagnosis.
References: lannaccone R et al.(2006).Peliosis Hepatis: Spectrum of Imaging Findings. AJR 187: W43-W52
-Postcholangitic hepatic fibrosis (Fig.34):

Fig. 34: Primary sclerosing cholangitis at severe stage. The peripheral liver shows advanced fibrosis.(A)axial T2WI shows that the T2 signal in the peripheral liver is higher with defined strands of elevated T2 signal, corresponding to fibrotic tissue. Arterial phase (B) images show nodular tissue corresponding to regenerative nodules. These show an elevated signal compared to intervening fibrotic tissue. This is due to higher protein content within hepatocytes, which causes an elevated T1 signal and increased vascularity, leading to greater enhancement on arterial and venous phase images. The delayed phase image (C) shows progressive uptake and enhancement of the fibrotic tissue.
References: Chundru S et al (2013) MRI of diffuse liver disease: the common and uncommon etiologies. Diagnostic and interventional radiology 19:479–487
-Radiation fibrosis:
- It occurs along with the radiation ports and does not follow any specific anatomic distribution.
- In advanced stage, the accumulation of fibrosis causes lobar atrophy, capsular retraction, and delayed enhancement.
**The above listed delayed-enhancing hepatic focal lesion can be summarized as follows:(Fig.35,36)

Fig. 35: Diagram summarizing hepatic focal lesions with different patterns of delayed enhancement.
References: Modified by department of radiology,Theodor Bilharz research institute,Egypt

Fig. 36
References: Department of diagnostic radiology,Theodor Bilharz research institute,Giza/EG