Keywords:
Performed at one institution, Cross-sectional study, Retrospective, Cirrhosis, Contrast agent-intravenous, MR, Liver, Contrast agents, Abdomen, Abdominal Viscera
Authors:
C. Gozzo, F. Vernuccio, V. Greco, R. Cannella, M. Midiri, G. Brancatelli; Palermo/IT
DOI:
10.26044/ecr2020/C-05900
Purpose
The adequacy of Portal Venous Phase (PVP) on contrast-enhanced CT and MR
imaging studies, is crucial for the evaluation of hepatic enhancement and detection of focal liver lesions [1]. According to EASL guidelines and LI-RADS, washout detected on PVP or delayed phase represents one of the major features for the characterization of hepatocellular carcinoma (HCC) [2].
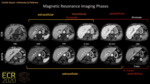
The use of hepatocyte-specific contrast agents, such as gadoxetic acid and gadobenate dimeglumine, has improved the diagnostic accuracy of MR for the diagnosis of HCC [3]. Some studies have already demonstrate significant differences in pharmacokinetic properties between gadoxetic acid and gadobenate dimeglumine in both healthy and cirrhotic livers [4,5]. Gadoxetic acid shows rapid hepatocellular uptake (starting at approximately 90 seconds after injection) which results in so-called “transitional phase” and hepatobiliary phase at 20 minutes after contrast injection [6]. Hepatocellular uptake of gadobenate dimeglumine starts later (40 min after contrast injection) with “pure” extracellular delayed phases and hepatobiliary phase at 60-180 minutes after contrast injection [6] (Figure 1).
Prior studies already demonstrated superior performance of gabodenate dimeglumine in portal venous phase in healthy patients [4,5]. Our hypothesis is that hepatic structural changes, along with a smaller dose of gadoxetic acid recommended for MR imaging compared to gadobenate dimeglumine may further hamper signal intensity of hepatic parenchyma on portal venous phase in cirrhotic patients.
The purpose of this study was to perform an intraindividual comparison of the
enhancement of cirrhotic liver parenchyma with gadoxetic acid and gadobenate dimeglumine on portal venous phase.