Endometrial cancer is basically divided into two groups according to histology1:
- Type 1: endometrioid adenocarcinoma in its mid-low grades.
- Type 2: formed by clear cell carcinoma, papillary serous and grade 3 endometrioid adenocarcinoma.
The most frequent subtype of all of the above is endometrioid adenocarcinoma (75% of cases), for which there are two types of risk factors, the most predominant being type I or estrogen dependent (85%), which develops from a hyperplasia. Less frequent is type II or non-estrogen dependent (15%), which is not related to endometrial hyperplasia and is much more aggressive than the previous one.
|
ENDOMETRIOID ADENOCARCINOMA TYPE I
|
ENDOMETRIOID ADENOCARCINOMA TYPE II
|
|
Frequency 85%.
Estrogen-dependent (endometrial hyperplasia).
Women with this type of cancer are usually obese, diabetic, nulliparous, hypertensive or have late menopause.
|
Frequency 15% and more aggressive.
Non-estrogen dependent (not related to endometrial hyperplasia).
Older postmenopausal women.
|
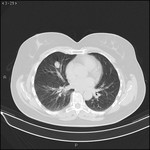
The two possible routes of dissemination are lymphatic, being able to reach para-aortic ganglia through the ovarian chain and without pelvic involvement; and the hematogenous route giving metastases in lung, bone and brain as target organs.
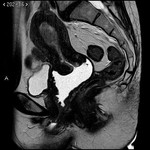
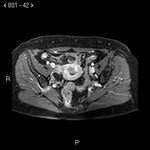
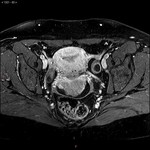
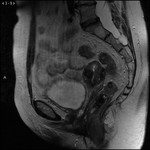
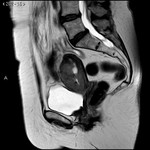
The first test to confirm the diagnosis is endovaginal ultrasound, where endometrial thickening will be appreciated, although this is not definitive. Staging is essential for treatment, and for this purpose the utility of MRI with diffusion sequence and intravenous contrast has been demonstrated before surgery, since it allows to see the tumor size, location, myometrial, cervical and distant invasion, with an accuracy between 85 and 93%2. In addition, in patients with high surgical risk due to comorbidity, MRI is useful for planning a non-surgical treatment, with radiotherapy or hormonal therapy.
The basic sequences that should be included in any study of MRI of the pelvis for suspected endometrial neoplasia are:
- Enhanced sequences in T2 TSE in axial, sagittal and coronal planes, with high resolution T2 sequences: endometrial carcinoma will be discreetly hypointense in regard to normal endometrium and slightly hyperintense in regard to the adjacent myometrium.
- Sequence enhanced in axial T1: the lesion is usually isointense to the myometrium, so its visualization is difficult.
- Power sequences in diffusion and ADC map: the neoplasms usually make diffusion restriction, this means that they shine in diffusion sequence and are hypointense in the ADC map. The diffusion allows us to determine the degree of myometrial invasion, the corn invasion and is useful to differentiate benign lesions from malignant ones.
- 3D gradient echo sequence after gadolinium administration with dynamic study. There are three phases of dynamic study:
• The early phase (minute 0 and 1): allows you to identify the subendometrial zone, which enhances before most of the myometrium. This phase is important to detect early invasion of the myometrium.
• The equilibrium phase (2-3 minutes after the injection of the contrast): it allows to better assess the degree of depth of the infiltration of the myometrium.
• The late phase (at 4-5 minutes): to see the invasion of the cervical stroma (the carcinoma is isointense in regard to the normal endometrium in the T1 enhanced sequences without contrast).
In our report we must reflect the following key points: the depth of the myometrial invasion (most important factor), the invasion of the cervical stroma, the existence of nodes and the extrauterine extension, since the prognosis depends on these factors3.
Based on the description of the findings, it is necessary to classify the lesion according to the staging of FIGO (International Federation of Gynecology and Obstetrics)4. We find four stages that are subdivided into A and B, as described below along with illustrative images:
Stage I: tumors limited to the uterine body.
• IA: tumor that affects less than 50% of the myometrium. We can identify the transition zone and the irregular or interrupted subendometrial early enhancement band (Fig. 1).
• IB: tumor that affects more than 50% of the myometrium. We will find a deep infiltration of the myometrium when we observe during the equilibrium phase hypointense tumor in the external myometrium (Fig. 2).
Stage II: tumors that go beyond the uterine body and reach the cervix.
• IIA: the infiltration of the endocervix appears as a dilation of the internal cervical orifice and the endocervical canal, with preservation of the normal fibrocervical stroma that is hypointense (Fig. 3).
• IIB: interruption in the T2 enhanced sequences of the normal cervical stroma, hypointense, due to the high signal of the tumor (Fig. 4).
Stage III: tumors that go beyond the uterus but not the true pelvis.
• IIIA: involvement of the parametria. The interruption of the serosa with direct extension to the adjacent fat is identified (Fig. 5).
• IIIB: extension to the upper part of the vagina. It is identified as a loss of normal hypointensity of the vaginal walls (Fig. 6).
• IIIC: appearance of adenopathies:
or IIIC1: positive pelvic nodes.
or IIIC2: positive para-aortic ganglia.
Stage IV: tumors that extend beyond the true pelvis, infiltrate the rectum or bladder.
• IVA: loss of normal hypointensity of the bladder or rectal wall.
• IVB: appearance of distant metastases, malignant ascites or peritoneal implants. Peritoneal implants are best detected in the late phase of dynamic contrast studies (Fig. 7).
Depending on the stage of the FIGO obtained, the treatment will be focused in a different way:
- Surgical treatment: surgical staging of endometrial cancer includes total extrafascial hysterectomy, bilateral anexectomy, pelvic lymphadenectomy and aorto-cava lymphadenectomy. The indication of lymphadenectomy added to the hysterectomy and anexectomy will depend on the following factors:
o Stage: lymphadenectomy can only be missed if the disease is confined to the uterine body.
o Type and histological grade: serous, clear cell or endometrioid grade 3 carcinomas require lymph node removal.
o Degree of myometrial infiltration: only lymphadenectomy will be canceled in myometrial infiltrations under 50%, since it implies a very low risk of adenopathic extension.
o In some cases of size: in tumors with histological grade 2 and myometrial infiltration less than 50%, without extension to the cervical stroma.
- Radiotherapy treatment: its indication depends on the depth of the myometrial invasion, the degree of tumor differentiation and the suitability of surgery, being necessary to take into account other factors for the type of radiotherapy treatment.
- Chemotherapeutic treatment: chemotherapy can be considered after radiotherapy treatment when the endometrial tumor has a high risk of recurrence. In addition, in stages IIIC and IV after cytoreductive surgery, adjuvant treatment with chemotherapy should be performed.
- Hormonal treatment: the use of progestogens is not recommended if there is adequate surgical staging, since it has not demonstrated a protective effect against recurrence. Therefore, it is a primary treatment option in the clinically inoperable patient or who does not want surgical treatment, and in the treatment of recurrence when the tumor is well differentiated and or expresses hormonal receptors.