Of the 55 patients, two patients died within 3 months (5.5%) and 53 had at least one radiological assessment of TARE response. During a median follow-up of 12.5 months, 49 patients had tumour progression (either intra or extra-hepatic, 89.1%); of these, 40 patients died (72.7%), resulting in a median PFS of 6 months and an OS of 16.7 months.
The 53 patients having at least one available radiological assessment of TARE response showed, as their best radiological response during follow-up, CR of the target lesion in 4 cases (7.6%), PR in 26 cases (49.1%), stable disease (SD) in 19 (35.9%) and progressive disease (PD) in 4 (7.6%), providing an OR in 30 cases (56.6%).
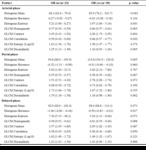
Texture analysis findings (Figere 1)
During the arterial phase, iCCs with OR had a higher mean of grey levels (p<0.001), indicating that the tumour had a higher uptake of iodine contras. The higher amount of white pixels resulted in lower kurtosis of the OR cases (p=0.043). The distribution was more homogeneous, as reflected by the higher GLCM Homogeneity (p=0.005) and the lower GLCM Contrast of the OR cases, a measurement of the variance of the intensity contrast between neighbour pixels (p=0.004) and by their higher GLCM Correlation value (P=0.030), a measurement of the dependency of grey levels of the neighbouring pixels. All these findings converged to a lower value of GLCM Dissimilarity in the OR cases (p=0.005).
In the portal phase cases with OR maintained a higher mean of grey levels (p=0.005), but the magnitude of the differences in GLCM Homogeneity (p=0.067), GLCM Contrast (p=0.073) and GLCM Dissimilarity (p=0.062) were consistently reduced.
In the delayed phase only the skewness appeared lower in the OR cases (p=0.037), suggesting a more symmetrical distribution of grey levels during the washout of the iodine contrast in the OR cases.
Development of the radiomic signature (Figure 2)
Of the textural features entered into the LASSO logistic regression, five explained the difference between the OR and the non-OR cases: the mean of grey levels (coeff: 0.0364) and the GLCM Homogeneity in the arterial phase (coeff: 14.6286); the skewness (coeff: 0.1316), the kurtosis (coeff: -0.0122) and the GLCM Dissimilarity (coeff: 1.9183) in the delayed phase. The intercept was -12.259. The combination of these textural features provided an area under the curve (AUC) for the prediction of an OR of 0.896 (95% confidence interval (CI) 0.814 – 0.977).
Determinants of survival (Figure 3)
 The median PFS of the 15 patients with a
The median PFS of the 15 patients with a  favourable radiomic signature was 12.1 months (95%C.I.:7.8 – not reached) whereas that of the 40 patients with an unfavourable signature was 5.1 months (95%C.I.: 3.0–6.7; p=0.008). The corresponding median OS of the favourable radiomic signature was 27.8 months (95%C.I.:11.1 – not reached) and that of the unfavourable radiomic signature was 14.5 months (95%C.I.:9.6–20.4; p=0.140).
favourable radiomic signature was 12.1 months (95%C.I.:7.8 – not reached) whereas that of the 40 patients with an unfavourable signature was 5.1 months (95%C.I.: 3.0–6.7; p=0.008). The corresponding median OS of the favourable radiomic signature was 27.8 months (95%C.I.:11.1 – not reached) and that of the unfavourable radiomic signature was 14.5 months (95%C.I.:9.6–20.4; p=0.140).
The strongest determinants of PFS were CA19-9 (p=0.002) and the radiomic signature (p=0.036) whereas the best determinants of OS were the history of previous surgery or embolo-therapies (p=0.001), CA19-9 (p=0.002) and largest diameter (p=0.001). The radiomic signature slightly  correlated with OS (p=0.148).
correlated with OS (p=0.148).