A. VASCULAR:
Arterial/venous vascular accesses are required in clinical practices for several reasons. Different types of catheters are used to gain vascular access; tunneled/non-tunneled central venous catheters (CVC), peripheral catheters, pulmonary artery catheters, peripherally inserted CVCs, umbilical arterial or venous catheters (UAC/UVC), midline catheters, etc…
Vascular catheters can be used for administering drugs, monitoring central venous pressure, measurement of central venous oxygen saturation/ renal replacement therapy/total parenteral nutrition/cardiac catheterization/transvenous cardiac pacing.
For well-functioning, ideal position of the catheter must be provided. There are ideal positions for each catheter type.
For CVC, it is recommended that the tip is positioned at the level of mid‑lower superior vena cava to atriocaval junction.
UVCs are used for venous access in neonates. The umbilical vein joins the portal vein. Ductus venosus makes connection between left portal vein and hepatic vein which is drained by inferior vena cava. The ideal position of the tip is in inferior vena cava, in close proximity to right atrium.
Umbilical arteries are direct continuation of internal iliac arteries. UAC passes through iliac artery into aorta, provides accurate measurement of arterial blood pressure. The catheter tip is left either at high (T6-T9) or low position (L3-L5) to avoid aortic branch catheterization.
Many factors like vein tortuosity, presence of collateral vessels, congenital anatomical variations, absence of imaging guidance, migration during or after procedure may result in misplacement.
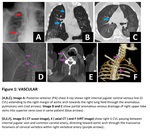
- Partial anomalous pulmonary venous return (PAPVR) is a congenital anomaly that occurs during embryological period when at least one pulmonary vein fails to communicate with left atrium, drains directly/indirectly into right atrium. It is mostly asymptomatic, and discovered incidentally or, as in our patient, after placement of CVC. (Figure 1-A/B/C). Presence of persistant left superior vena cava may be problematic during CVC placement.
- Due to absence of imaging guidance, wrong vessels may be punctured, correct access site may be damaged, tip of catheters may not be left in desired location (Figure 1/2/3). For example vertebral artery injury related to CVC is extremely rare with reported incidence of 0.2%, usually occurs during internal jugular vein catheterization attempts. Because of catastrophic complications related to inadvertent puncture of vertebral artery, image guidance plays important role to reduce incidence of malposition (Figure 1-D/E/F).
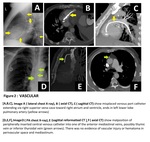
- The displacement of catheter into anterior mediastinal venous structures (as collateral vessels) is extremely rare phenomenon, only few cases reported in literature. Sagittal images may facilitate diagnosing (Figure 2-D/E/F).
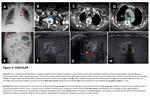
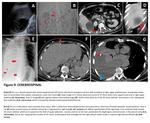
Recognizing misplaced catheter is important because poor catheter positioning may result in premature failure of CVCs, bleeding, rupture of related vessels. Furthermore usage of misplaced catheters may cause additional problems. For example, drug administration from malposed catheter may lead to extravasation which could cause compression of peripheral structures due to mass effect or turn into abscess secondary to infection (Figure 3-A/B/C/D). Moreover, malposed UVCs may lead to hepatic necrosis/TPN-omas/necrotizing enterocolitis/pericardial effusion/thrombotic endocarditis (Figure 3- E/F/G/H).
B. NON-VASCULAR
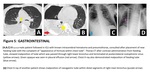
1. Gastrointestinal
There are different types of tubes, drainage catheters, stents related to gastrointestinal system. While metallic/plastic biliary stents/biliary drainage catheters/cholecystostomy catheters/pancreatic stents are related to hepatobiliary portion; nasogastric tube, gastrostomy/jejunostomy tubes, duodenal/rectal stents related to hollow viscera of GI system.
Biliary stenting/drainage are mainly done to reestablish patency of biliary system in obstructive jaundice caused by malign/benign strictures. Cholesistostomy catheters are placed directly into gallbladder lumen, employed for various gallbladder conditions, mainly cholecystitis. Nasogastric tubes are used for gastric decompression/administration of medication/contrast material/enteral nutrients/evaluation of upper GI bleedings.
Gastrostomy/jejunostomy tubes can provide long-term enteral feeding access. Duodenal/ rectal stents are placed usually for palliating luminal narrowing caused by malignancy.
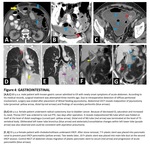
Biliary stents should be placed in common bile duct, covered strictured segments. Stent migration, either proximally or distally, is possible, can be problematic. A nasogastric tube should be located in stomach – at least 10 cm beyond gastroesophageal junction. Common malpositioning includes tip-positioning in esophagus/bronchus/lung/even cranium- spinal canal (in case of skull base fracture). Malpositioning of nasogastric tubes may cause several complications such as pneumothorax/pleural effusion/abscess. Jejunostomy tubes must be placed in lumen of jejunum which is fixed to anterior abdominal wall. Extraluminal placement rarely occurs, may cause peritonitis.
Case examples related with malposed gastrointestinal catheters are shown in (Figure 4/5).
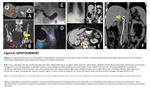
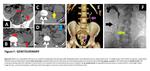
2. Genitourinary
Foley catheters/cystostomy/nephrostomy catheters/double J stents (DJS) are commonly used genitourinary catheters in clinical practice.
Foley catheter is utilized to drain the bladder through the urethra, its inflatable balloon should be located in bladder lumen. Cystostomy is performed to drain urinary bladder but catheter is placed into bladder lumen through anterior abdominal wall. Percutaneous nephrostomy tube, which is placed into renal pelvis through flank area, drains urine from obstructed urinary tract to protect kidney. Less frequently, it is performed to divert urine away from surgical anastomoses or injured (commonly iatrogenic) segments of the ureter. DJS has two J-shaped pig-tail ends. One of them is anchored in renal pelvis while other end is placed in urinary bladder lumen. It bridges the renal pelvis, ureter bladder.
Foley catheter malpositions include extra-urethral positioning due to urethral trauma/inadvertently inflated balloon in the urethra/even placement in the ureter, infrequently. In females, vaginal catheterization is possible. The most common extravesical positions of cystostomy catheters are space of Retzius/peritoneal space. The nephrostomy tip can be incorrectly positioned in dilated calyx or extrarenal space. DJS displacements are relatively rare in comparison to other complications including migration or kinking. In case of misplacement stent may penetrate ureter/collecting system/renal parenchyma.
Case examples related with malposed genitourinary catheters are shown in (Figure 6/7).
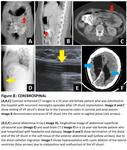
3-Cerebrospinal
In radiological studies, ventricular shunts are the most commonly encountered catheters related with central nervous system. Besides ventricular shunts, different types of devices like morphine pumps/ central nervous system simulators could be visualized.
Ventricular shunts are indicated to treat congenital/acquired causes of hydrocephalus, divided into subgroups regarding anatomic locations of termination points; ventriculoperitoneal (VP) shunts/ventriculoatrial shunts/ventriculopleural shunts/lumboperitoneal shunts. Due to effective absorption capacity of peritoneum, ventriculoperitoneal shunting is mostly preferred. However, intraabdominal adhesions and peritonitis may interfere with optimal drainage of ventriculoperitoneal shunt. In those cases, distal tip of ventricular shunts could be placed in gall bladder/ureter/stomac/even fallopian tube, according to literature. Knowledge of those unusual termination sites may prevent confusion, falsely-reported malposition.
The superior tip of ventriculoperitoneal shunt catheter is placed in ventricle. The external portion is connected to a valve which regulates cerebrospinal fluid flow based on a preset pressure. The distal end is tunneled under skin, and anchored into peritoneal cavity, usually in right lower quadrant of abdomen.
Case examples related with malposed cerebrospinal catheters are shown in (Figure 8/9).
4. Bronchopulmonary Catheters
Different types of tracheobronchial (endotracheal intubation tubes, tracheal stents, tracheostomy) and pleural catheters/tubes can be visualized in thorax studies.
Main indications for endotracheal entubation are keeping airway open, and support breathing in critically ill patients. The ideal position for endotracheal tube tip is 5±2 cm above the carina. Selective intubation (mainly right), and highly placed catheter tip may cause complications such as one-sided atelectasis, aspiration pneumonia or inadvertent extubation.
Tracheal stents prevent airway collapse, and generally is placed for palliation. The main indications for chest tubes and pleural catheters, which are placed into pleural space, are pneumothorax , collection of effusion/pus/hemorrhage in pleural space. Extrapleural placement of the chest tube may result in recurrent pneumothorax/inefficient drainage/accidental tube removal.
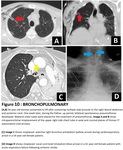
Case examples related with malposed cerebrospinal catheters are shown in (Figure 10).