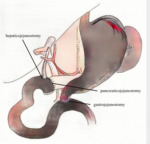
The classic pancreaticoduodenectomy consists of the resection of the pancreatic head, neck and uncinate process, along with the duodenum, gallbladder, distal bile duct and proximal jejunum, while also removing the gastric antrum and the regional lymph nodes. The resection is followed by the creation of three anastomoses: pancreaticojejunostomy, hepaticojejunostomy, and gastrojejunostomy (Fig. 1) [2]. In some cases, instead of the pancreaticojejunostomy, a pancreaticogastrostomy (Fig. 5) is preferred; however, studies have failed to show advantage of a particular technique, therefore the method of choice is still debatable [4].
Normal postoperative findings
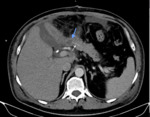
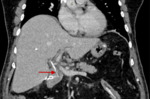
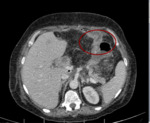
The normal postsurgical anatomic findings consist of the detection of the aforementioned anastomoses [pancreaticojejunostomy (Fig. 2), hepaticojejunostomy (Fig. 3), gastrojejunostomy (Fig. 4)] and the identification of the superior mesenteric vein and splenomesenteric junction, located to the right of the pancreatic stump and more posteriorly, towards the inferior vena cava [1].
Pneumobilia is found in up to 80% of the postoperative CT examinations and can enable the visualization of the hepaticojejunostomy [5].
Perivascular cuffing, described as increased attenuation of the mesenteric fat surrounding the vascular structures such as the celiac axis or superior mesenteric artery, is common and should not be misinterpreted as residual tumor or tumor recurrence, since it is most likely caused by local inflammation, particularly in patients with negative surgical margins [1,2,5].
- TRANSIENT FLUID COLLECTIONS
Transient fluid collections, represented by poorly delineated fluid collections with thin walls, are an acceptable finding during the first 2 weeks post-surgery, while the presence of air bubbles inside of them, even though it is not a definite sign of infection, should raise suspicion of a pancreatic fistula (Fig. 6) [1,5].
Lymph nodes measuring up to 1 cm in size can also be identified surrounding the surgical bed and should be interpreted as reactive lymphadenopathies (Fig. 7) [1,2,5].
Edema of the gastrojejunostomy, illustrated by thickening of the anastomosis, has been described as a relatively common finding, along with dilatation of the pancreatic duct due to edema of the pancreaticojejunostomy and mild intrahepatic biliary dilatation caused by edema of the hepaticojejunostomy [1,2].
The first postsurgical examination stands as a baseline for follow-up examinations, which should depict either resolution or stability of all these findings [2].
Complications
The development of a pancreatic fistula represents the most significant cause of morbidity and mortality following the Whipple procedure, with a rate of occurrence varying from 0% to 25 %. It is defined as the presence of an anastomotic leak at any time on or after the third postoperative day, with an amylase content higher than three times the upper normal serum value, but clinical relevance is also to be taken into consideration [6]. Even though the analysis of the drainage fluid is essential for the diagnosis, CT findings such as a focal fluid collection or hemorrhage in the proximity of the pancreaticojejunostomy or in contiguity with the pancreatic duct might suggest the existence of a pancreatic fistula (Fig. 8) [2]. In 80% of cases, fistulas heal with conservative management, 10-15% require percutaneous drainage and only 5% undergo repeat surgery due to the suspicion of severe anastomotic dehiscence [7].
The presence of an intraabdominal or retroperitoneal abscess is usually secondary to a pancreatic fistula, superinfection of the acute postoperative fluid collections or leakage from the hepaticojejunostomy or gastrojejunostomy (Fig. 9) [2]. Percutaneous abscess drainage is possible under ultrasonographic or CT guidance [7].
Postoperative hemorrhage can be caused by active bleeding from the gastroduodenal artery stump due to improper ligation or vascular erosions [2]. When replacement of more than 3 units of blood later than 24 hours after the surgery is required, it should raise suspicion of intraabdominal bleeding and indicate the need for endoscopic evaluation or urgent surgical exploration [5,7].
An increase in serum amylase or lipase greater than three times the normal value later than 3 days post-surgery might indicate inflammation of the pancreatic remnant, but the accuracy of these measurements might be affected by the surgical manipulation of the pancreas, thus elevating the values of these markers [2, 5]. The presence of peripancreatic inflammatory changes, fluid and infiltration surrounding the pancreatic remnant can be suggestive of pancreatitis (Fig. 10) [2].
- LEAKS FROM GASTROJEJUNOSTOMY
Leaks from gastrojejunostomy are suggested by the presence of fluid collections adjacent to the anastomosis (Fig. 11). If a leak is suspected, positive oral contrast material can be administered, with direct extravasation at the site of the anastomosis [2].
- PORTAL VEIN AND SUPERIOR MESENTERIC VEIN THROMBOSIS
While the changes concerning tumor resectability have made a greater number of patients eligible for surgery, the procedure now requires more complex vascular reconstructions, which come with the major drawback of a higher rate of complications. Venous thrombosis can lead to intestinal ischemia, ascites, hepatic ischemia and even death. Coronal images are extremely helpful in making this diagnosis, especially for thrombi located in the SMV [2].
Hepatic infarction can be caused by an underlying abnormality in the patient's mesenteric vasculature, by an intraprocedural injury of the hepatic or celiac arteries or thrombosis of the hepatic artery or portal vein. The mortality is approximately 50%, since most cases develop other major complications such as biliary necrosis, hepatic superinfection and local abscesses (Fig. 12) [2].
- LEAKS FROM HEPATICOJEJUNOSTOMY
Bile leaks are rare and most often occur due to technical failure. Visualization of a focal fluid collection in the proximity of the anastomosis, with elevated levels of bilirubin in the drainage fluid are highly suggestive of a bile leak [2].
Delayed gastric emptying can be found in up to 50% of patients. The prolonged need for a nasogastric tube after surgery and the presence of an extremely distended stomach filled with oral contrast material should raise suspicion of this complication [2,5].
Anastomotic strictures can appear as a delayed complication. They cause dilation of the pancreatic duct or intrahepatic biliary ducts, requiring differential diagnosis between benign strictures and malignant strictures due to local tumor recurrence. The treatment is nonsurgical, consisting of balloon dilatation [2, 7].
CT can detect disease recurrence with an accuracy of 95%. Local recurrent disease appears as an infiltrating mass located in the surgical bed, associating perineural invasion and encasement of the mesenteric vessels (Fig. 13) [1,5]. The levels of CA 19-9 can be used to differentiate between local recurrence and post-operative inflammatory changes [5].